Note: Descriptions are shown in the official language in which they were submitted.
Geddes-Hinds-Bourland-Voorhees 1-1-1-1 !~iJ
METHOD AND APPARATUS FOR THERMALLY
DESTROYING A LAYE~ OF AN ORGAN
Technical Field
This invention relates to catheters and, in particular,
method and apparatus including a catheter for heating the
layer of an organ.
Background of ~he Invention
Gallstones are a common problem in the United States and
the most frequent cause of gallbladder inflammation. About
500,000 cholecystectomies are performed each year with an
overall medical cost nearing approximately two billion
dollars. Patients of all ages with cholecystitis have a
mortality rate of 1.3% to 5%. For those over 65 years of
age, the rate increases to 10%. When empyema of the
gallbladder is present, the mortality rate is close to 29%.
As the population ages, there will be more and more poor-
risk patients with troublesome gallstones.
Removal of only gallstones, without a cholecystectomy,
offers promise of reducing risk, but only solves the problem
temporarily. Nearly 50% of the patients having a surgical
cholecystostomy with the gallbladder left intact will have
a recurrence of gallstones within three years or less, and
80% will develop stones within 15 years. As yet, there are
no long-term follow-up studies for nonsurgical removal of
gallstones by extracorporeal shockwave lithotripsy or by
methyl-tertiary-butyl ether treatment. However, one study
evaluating the recurrence of gallstones following another
nonsurgical method of removal, bile-acid treatment, found
the recurrence rate to be 24% at one year, rising to 58% at
two years, 63% at three years, and 100% at five years.
Other bile-acid treatment studies have indicated somewhat
lower rates of recurrence, but 50% eventual recurrence seems
to be generally accepted. Therefore, the need for
preventing the recurrence of gallstones is significant.
Geddes-Hinds-Bourland-Voorhees 1-1-1 1 ~ c- r
This is further heightened by eliminating the problem with
a nonsurgical solution that will reduce the costs and the
mortality rate associated with surgical methods.
Summary of the Invention
The foregoing problems are solved and a technical
advance is achieved by a method and apparatus for thermally
destroying the layer of an organ such as by thermally
coagulating the mucosal layer of the gallbladder to reduce,
if not eliminate, the recurrence of gallstones.
Illustratively, the apparatus includes a catheter comprising
an elongated member having a current-emitting electrode
positioned about the distal end thereof for emitting
radiofrequency current. The catheter also includes a
capacitive balloon electrode that is positioned about the
distal end of the elongated member and surrounds the
current-emitting electrode for performing a number of
advantageous functions~ First, the balloon electrode
distributes the radiofrequency current-from the current-
emitting electrode to the layer~ This facilitates a more
uniform distribution of the emitted current to the mucosal
layer. Next, the balloon electrode is expanded with an
electrolyte solution for making contact with the mucosal
layer and for containing the electrolyte solution. The
electrolyte solution has a resistivity less than the
resistivity of the mucosal layer for selectively heating the
mucosal layer.
The change in resistivity from a lesser to a higher
level at the interface of the electrolyte solution and the
mucosal layer causes a concentrated deposition of power
within the mucosal layer of the gallbladder. The degree of
resistivity change at the interface controls the
concentration of power deposited in the mucosal layer and
consequently the selective heating of the mucosal layer.
The greater is the resistivity change; the greater is the
concentration of power in the mucosal layer. Furthermore,
~ Geddes-~inds-Bourland-Voorhees 1~ r 7~
~: ., ;J
a power deposition peak occurs at the interface of the
electrolyte solution and the mucosal layer.
The capacitive balloon electrode is also expanded for
conforming the shape of the gallbladder and the balloon
electrode together. This brings the capacitive balloon
electrode in physical and electrical contact with the
mucosal layer for distributing the radiofrequency current to
the mucosal layer in a more uniform manner. The balloon
electrode also contains the electrolyte solution and brings
the solution within close proximity of the mucosal layer.
As a result, electrolyte solutions that have resistivity
levels much lower than that of the mucosal layer, as well as
the gallbladder bile, may be used to expand the balloon
electrode. This containing feature is particularly
advantageous since some of the lower resistivity level
solutions are caustic to the surrounding tissue. These
lower resistivity level solutions can also be made radio-
opague, thereby allowing fluoroscopic visualization of the
balloon electrode in the gallbladder prior to applying the
radiofreguency current. A filling lumen extending
longitudinally through the elongated member and a plurality
of sideports about the distal end thereof are utilized to
fill and expand the balloon electrode with the electrolyte
solution.
A second lumen is also provided in the elongated member
for draining the bile from the gallbladder as the balloon
electrode expands. Draining the bile from the gallbladder
permits the lower resistivity level electrolyte solution to
be positioned in close proximity to the mucosal layer.
The wall of the balloon electrode comprises a relatively
thin flexible material such as latex which has a relatively
large predetermined capacitance. Consequently, the
impedance of the capacitive balloon electrode to the
radiofrequency current is relatively low. The
radiofrequency current is thus negligibly impeded by the
capacitive balloon electrode.
G~ddes-Hinds-Bourland-Voorhees 1-1-1-1 , ' ;;, ~5
The catheter also includes a sensor positioned about the
distal end of the member for sensing a temperature of an
environment about the distal end. Illustratively, this
sensor includes a thermistor for sensing the temperature of
the current-emitting electrode and the surrounding
electrolyte solution which is indicative of the tempe~ature
of the mucosal layer. A pair of electrical conductors
connected to the thermistor extends through a third lumen in
the elongated member to a control circuit. In response to
the sensed temperature, the control circuit regulates the
amount of radiofrequency current supplied by a generator to
the current-emitting electrode.
The radiofrequ~ncy current is supplied to the current-
emitting electrode via a conductor extending throush a
fourth lumen in the elongated member to the current-emitting
electrode.
The apparatus also includes the radiofrequency current
generator and the control circuit that cooperate to supply
current to the current-emitting electrode. The electrode is
used to heat the mucosal layer of the gallbladder to a
predetermined temperature for a predetermined period of time
to thermally coagulate the mucosal layer. Consequently, the
mucosal layer is thermally destroyed along with the mucosal
layer of the cystic duct for advantageously preventing the
recurrence of gallstones within the gallbladder. The
selective deposition of power in the mucosal layer also
prevents thermal destruction of the outside wall of the
gallbladder ~nd the surrounding tissue.
To significantly reduce the risks associated with
surgery, the method of the invention includes inserting the
distal end of the catheter endoscopically into the
gallbladder by a retrograde route through the duodenum,
common bile duct and cystic duct.
According to the invention, there is provided apparatus
including an extendible arrangement which when extended
would conform to the normal contour of the inner wall of a
Geddes-Hinds-Bourland-Voorhees 1-1-1-1
gallbladder and would serve to position or locate the RF
emitter arrangement within the inner wall. The extendible
arrangement can take several forms, in one of which the
distal end of the elongated member may be found in
expandable strips which can expand to contact the wall of
the gallbladder. The current-emitting electrode is
internally affixed to the distal tip of the member and
operated to expand the strips radially and hold the
electrode in the center of the gallbladder. The expanded
strips engage and make contact with the inner mucosal layer
of the gallbladder. Experiments with this conductive
electrode catheter indicated that an electrode temperature
of 72 was needed to maintain the mucosal layer at 50C
while the outer wall temperature was approximately 41C.
The radiofrequency generator utilized in these experiments
had a tentative frequency of two megahertz with signal
amplitude ranging between 0-2 amps rms of radiofrequency
current. In such an arrangement, the bile in the
gallbladder is used to conduct the RF energy to the said
wall. Some form of seal, additional to the presence of the
apparatus, could be required to enclose and maintain the
bile within the bladder.
If the possibility of gallbladder rupture is a problem,
when the leakage of bile from such a rupture could be
prevented by providing a balloon about the said distal end.
The latter would be expanded by inserting liquid therein to
expand the balloon to the normal boundary of the
gallbladder.
If bile leakage were not a problem then a balloon could
be partially expanded by partially filling it with liquid.
Some bile could be retained thereabout in the bladder.
In both of these latter embodiments, the balloon would
serve the function of both locating the emitter and
containing liquid within the bladder. The liquid within the
bladder can have any resistivity which is consistent with
the objective of assisting in the destruction or coagulation
Geddes-Hinds Bourland-Voorhees 1~
(burning) of the inner wall of the bladder. It may also be
made radio-opaque.
The balloon may have more than one compartment so that
di~ferent fluids can be forced therein, the fluid of higher
resistivity being forced into the outer compartment.
Brief Description of the Drawin~s
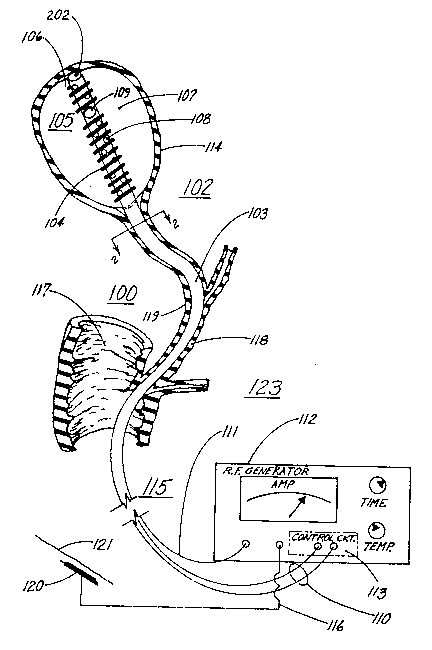
FIG. 1 depicts apparatus inserted in the body of the
gallbladder for thermally destroying the mucosal layer
thereof;
FIG. 2 depicts a cross-sectional view of the elongated
member of the apparatus of FIG. 1;
FIGs. 3 and 5 depict a spherical model of a gallbladder
and the power deposition at a radial distance from a central
electrode placed in the spherical model; and
FIG. 5 depicts an enlarged view of the distal end of the
elongated member of the apparatus of FIG. 1.
Detailed Description
Depicted in FIG. 1 is illustrative apparatus 123
including a catheter 100 having a distal end 105 that is
inserted into an organ such as body 114 of gallbladder 102
for thermally coagulating and destroying the inner mucosal
layer 101 of the gallbladder. The distal end of the
catheter is endoscopically introduced into the body of the
gallbladder by a retrograde route through the duodenum 117,
common bile duct 118, and cystic duct 119. Catheter 100
includes an elongated member 103 with a current-emitting
electrode 104 positioned about the distal end thereof for
emitting radiofrequency current to the mucosal layer of the
gallbladder. Also positioned about the distal end of the
elongated member and surrounding the current-emitting
electrode is capacitive balloon electrode 106, which is
expandable for making physical and electrical contact with
the mucosal layer of the gallbladder.
The balloon electrode is expanded with an electrolyte
G~ddes-Hinds-~3Ourland-Voorhees 1~
solution 107 that has a resistivity level less than the
resistivity level of the mucosal layer for concentrating the
deposition of radiofrequency power in the mucosal layer.
The mucosal layer 101 of gallbladder 102 has a relatively
high level of electrical resistivity approximating, for
example, 500 ohm-cm. The electrical resistivity of the
electrolyte solution is at a much lower level and
approximates, for example, 1~ ohm-cm. The solution
resistivity is also selected to be less than the resistivity
of the gallbladder bile, which typically approximates 70
ohm-cm. The change in resistivity from 10 ohm-cm to 500
ohm-cm represents a significant gradient in the order of one
and a half orders of magnitude. The radiofrequency heating
method of this invention exploits this low-to-high level
change in electrical resistivity from the electrolyte
solution to the mucosal layer at the interface thereof. A
large change in resistivity causes a concentrated power
deposition in the inner mucosal layer of the gallbladder,
because there is greater power dissipation in media of
higher electrical resistivity. It is this power deposition
as a function of distance from the current-emitting
electrode that produces selective heating.
A spherical model of a gallbladder is depicted in FIG.
3 to illustrate the selective haating feature of the
invention. A current-emitting point electrode 300 is
positioned at the center of a spherical gallbladder 301 of
1.0 cm inner radius filled with bile 302 having a
resistivity of 70 ohm-cm. Beyond 1 cm is the inner mucosal
layer 303 and outer gallbladder wall 304 of resistivity
approximating 500 ohm-cm. Beyond the outer gallbladder wall
is the liver (not shown) with approximately the same
resistivity. The deposited power density as a function of
radial distance from the electrode is illustrated by curve
305 depicted in FIG. 5. The deposited power density at any
point on curve 305 is J2 p, where J is the current density
(current I divided by area) and p is the electrical
Geddes-Hinds-Bourland-Voorhees 1-1-1-1 'iy "
resistivity. ~t any radius r, the current density
J=I/(4~r2)~ Current density J decreases as the inverse
s~uare of the distance from the electrode in the center of
the sphere. From the central electrode, the radiofrequenc~
current first encounters the low-resistivity bile and then
the high-resistivity bladder wall and extrabladder tissues.
It is the deposited power that produces heating. At a
distance beyond the bile of the gallbladder (r > l.Ocm), the
current density continues to decrease, but the resistivity
rises to a high level such as 500 ohm-cm. Consequently,
there is a peak in power deposition in the inner mucosal
layer 303 of the gallbladder where the resistivity gradient
at the interface is the largest changing from 70 ohm-cm to
500 ohm-cm. As a result, there is a concentration of
deposited power in and selective heating of the mucosal
layer at the bile-gallbladder interface.
Returning the reader's attention to FIG. 1, balloon
electrode 106 is expanded with an electrolyte solution lQ7
having a resistivity lower than that of the gallbladder
bile. This further enhances the resistivity gradient at the
interface and more selectively concentrates the power
deposition and heating in the mucosal layer. By way of
example, the electrolyte solution used to expand balloon
electrode 107 comprises a solution of 5% saline with
potassium iodide added to provide radio-opacity. The
addition of 5 grams of potassium iodide to 100 ml of 5%
saline reduces the resistivity of the latter by 25%. The
resistivity of the resulting mixture is 10 ohm-cm at 37
centigrade. The resistivity gradient at the electrolyte
30 solution-mucosal layer interface is now 10/500, rather than
70/500 when, as previously described, bile carried the
radiofrequency current. The steeper resistivity gradient
enhances selective power deposition and heating in the
mucosal layer.
Depicted in FIG. 2 is a cross-sectional view of the
elongated member 103 of the cathet r. The elongated member
Geddes-Hinds-Bourland-Voorhees 1-1-1-1 ; , ' s~
includes a plurality of lumens 201-204 that extend the
entire longitudinal length of the member. Filling lumen 201
is for transporting the electrolyte solution from the
proximal end 115 oP the catheter to the distal end 105. ~s
shown in FIG. 1, a plurality of side ports 108 about the
distal end connected to filling lumen 201 facilitates the
expansion of capacitive balloon electrode 106. The balloon
electrode is attached in a well-known manner to the distal
end of the catheter and expands with the electrolyte
solution to make electrical and physical contact with
mucosal layer 101 of the gallbladder. The balloon electrode
also contains the electrolyte solution and prevents caustic
solutions from causing possible undesired injury to
surrounding tissue. The shape of the gallbladder conforms
to the expanded electrode to provide a more even
distribution of radiofrequency current to the mucosal layer.
Positioning of the balloon electrode and contact with the
mucosal layer is visualized and verified by any one of a
number well-known techniques such as fluoroscopy. Such
technique is enhanced with the radio-opaque electrolyte
solution.
The balloon electrode comprises a thin wall or layer of
material, such as well-known latex, having a thickness
ranging from two to ten thousandths of an inch. Since the
balloon wall is very thin, the capacitance thereof is thus
quite large approximating, for example, 10,000 pF. The
reactance of this capacitive electrode to, for example, a
two megahertz radiofrequency current signal is thus
relatively low such as 7 ohms. As a result, the
radiofrequency signal is negligibly impeded by the balloon
wall.
A second lumen ~02 included in elongated member 103
transports gallbladder bile from distal end 105 of the
catheter to proximal end 115 for drainage therefrom.
Depicted in FIG. 4 is an enlarged view of the second lumen
202 included in elongated mem~er 103. This drainage occurs
Geddes-~inds-Bourland-Voorhees 1-l-1~
as a result of expanding the balloon electrode and
consequently forcing the gallbladder bile into the drainage
lumen.
Positioned about the distal end 105 of the catheter is
sensor 109 such as a well-known thermistor for sensing the
temperature of the surrounding environment. A volume of
this environment includes the current-emitting electrode,
the electrolyte solution and the mucosal layer of the
gallbladder. Since a direct reading of the mucosal layer
temperature is not practically feasible, the temperature of
the electrolyte solution and current-emitting electrode are
utilized to closely approximate the temperature of mucosal
layer 101. This approximation is derived from a number of
experimental measurements along with knowing the power
deposition characteristics of the radiofrequency current
from the current-emitting electrode as previously described
with respect to the spherical model. A third lumen 203 in
member 103 of the catheter provides a channel for extending
a pair of electrical conductors 110 that are connected to
temperature sensor 109.
The electrical conductors from the thermistor are
connected to a well-known control circuit 113 included in
radiofrequency generator 112 for controlling the amount of
current supplied to current-emitting electrode 104 as a
function of temperature. The sensed temperature is used to
control the amount of current supplied to the current-
emitting electrode so as to maintain the temperature of
mucosal layer lOl at a temperature such as 50 centigrade to
thermally coagulate and destroy the layer. Since the power
deposition gradient is the steepest at the mucosal layer,
the outer layer 115 of the gallbladder is not thermally
destroyed since the temperature therein is less than the 42
centigrade temperature necessary to thermally destroy living
tissue.
A fourth lumen 204 is also included in elongated member
103 for housing an electrical conductor lll for
Geddes-Hinds-Bourland-Voorhees 1~
interconnecting current-emitting electrode 104 and
radiofrequency current generator 112. A large dispersive
; electrode 120 is placed on the skin 121 of the patient's
body (not shown) to receive the radiofrequency current
emitted from the balloon electrode and conducted through the
body of the patient and to reduce trauma to the body.
Another electrical conductor 116 interconnects the
dispersive electrode and the radiofrequency current
generator.
10The method for thermally destroying, or more
specifically, thermally coagulating the mucosal layer of the
gallbladder includes inserting the distal end of the
catheter into body 114 of gallbladder 102 endoscopically by
a retrograde route through the duodenum, common bile duct
and cystic duct. The capacitive balloon electrode is then
expanded with the electrolyte solution for making electrical
and physical contact with the gallbladder. The balloon
catheter also conforms the gallbladder thereto to provide a
mors uniform distribution of the radiofrequency current from
the current-emitting electrode. The use of the electrolyte
solution with a resistivity lower than gallbladder bile and
of the thin wall balloon electrode permits the concentrated
deposition of power within the mucosal layer of the
gallbladder. This concentrated deposition of power causes
the selective heating of the mucosal layer to a thermally
destructive temperature without destroying or killing outer
layer 122 of the gallbladder. The mucosal layer of the
cystic duct is also thermally destroyed to prevent the
recurrence of gallstones therein. The temperature of the
mucosal layer is maintained at a predetermined temperature
such as 50 centigrade for a predetermined period of time to
ensure the thermal coagulation and thermal destruction of
the entire mucosal layer. Heating times for thermally
coagulating and destroying the mucosal layer of the
gallbladder in dogs has been derived from experiments in
which heating times varied from 6-15 minutes at
Geddes-Hinds-Bourland-Voorhees 1~
approximately 50 C for dogs ranging in weight from 8-23kg.
The percentage of mucosal layer destroyed varied from 90-
lQ0%.
It is to be understood that the above-described method
and apparatus for thermally destroying the layer of an organ
is merely an illustrative embodiment of the principles of
this invention and that other apparatus and methods may be
devised by those skilled in the art without departing from
the spirit and scope of this invention. In particular,
different electrolyte solutions with varying resistivities
may be employed along with different degrees of radio-
opacity. In another embodiment, the capacitive balloon
electrode may be eliminated and the distal end of the
elongated member slit along the longitudinal axis thereof to
form several strips therein. The current-emitting electrode
is internally affixed to the distal tip cf the member and
operated to expand the strips radially and hold the
electrode in the center of the gallbladder. The expanded
strips engage and make contact with the inner mucosal layer
of the gallbladder. Experiments with this conductive
electrode catheter indicated that an electrode temperature
of 72 was needed to maintain the mucosal layer at 50 C
while the outer wall temperature was approximately 41 C.
The radiofrequency generator utilized in these experiments
had a tentative frequency of two megahertz with signal
amplitude ranging between 0-2 amps rms of radiofrequency
current.