Note: Descriptions are shown in the official language in which they were submitted.
2026~3
ATTOR~lE;Y DOCXE;T NO. 9155
2 OMBS t 9155PA/DR4 / O O 9
~:LS~rOI~ P~lMP
~c~.r,3~)~n nF T~: DTS('T.n!;~RF~
This invention relates to blood pumps, particularly to
a temporary circulatory assist pump adapted for insertion into
the vascular system of a patient to provide temporary circulatory
assistance for a dys~inetic left or right ventricle of the heart.
Death and disability from heart disease are most
commonly due to the pumping inadequacy of an infarcted left or
right ventricle. The heart of a patient suffering from this
condition functions in many other respects but does not provide
sufficient blood flow to keep the patient alive. Typically, a
patient suffering from this condition would require major surgery
to maintain the heart and provide suffic~ent blood flow for the
patient.
Another area where temporary circulatory assistance may
be required is in allograft cardiac replacement or heart
transplants. Although one year survivals after a heart
transplant now approach 80%, a great many patients die waiting
for a transplant, as do many of the 20% who might be saved by
circulatory assistance while immunosuppressive agents are
combat~ng the body's natural rejection response of a transplanted
heart. There is a great need for an effective circulatory assist
pump for maintaining the life of a patient until the transplant
can be accomplished and the allograft is stabilized. As the
average life expectancy of the U.S. population continues to
increase, coronary artery disease and chronic congestive heart
failure can be expected to significantly increase the utilization
of mechanical circulatory assistance. A realistic estimate of
the number of potential candidates for mechanical circulatory
assistance would be approximately 300,000 patients each year in
202~6~
the United States. This number will grow at a rate of 6% per
year until the population of ~baby boomers" peaks around the year
2020.
~ ethods and apparatus exist ln the prlor art for
circulatory ass$stance of a heart. In U.S. Patent No. 4,625,712
a hlgh capacity ~ntravascular blood pump ~ disclosed. The pump
ln inserted into the heart through the femoral artery and driven
via a flexible cable from an external power source. The drive
cable is contained within a catheter attached to the pump. The
pump is rotated in the range of 10,000 - 20,000 rpm to produce
blood flow on the order of 4 liters per minute.
U.S. Patent No. 3,505,987 discloses a counterpulsation
system for aiding coronary circulation. The system includes an
expandable impeller located within the aorta of a patient. The
impeller is expanded and contracted while simultaneously being
reciprocated within the aorta and synchronized with the pumping
activity of the heart for reducing aortic pressure during systole
and increasing aortic pressure during diastole.
U.S. Patent No. 3,567,069 discloses an implantable jet
pump for replacing or assisting the right heart. The jet pump
comprlses an elongated tubular structure including an upstream
driving nozzle from which a driving flow of arterial blood under
pressure is ejected into a suction nozzle creating its own
reduced pressure to cause venous blood to be sucked into and
admlxed with the driving flow for distribution to the pulmonary
circulation system. The jet pump may be powered by blood pumped
from the left heart or an artificial replacement for the left
heart.
U.S. Patent No. 4,051,840 discloses an aortic patch
which may be surgically implanted in the thoracic aorta. The
aortic patch is systematically inflated and deflated to generate
pressure wave~ in the blood stream. The pressure waves assist
the heart by augmenting the circulation of the blood to the body.
~2i6~93
Generally, the methods available for circulatory
assistance of the heart require major surgery for the
implantation of the de~ice which presents a great risk to the
survival of the pat~ent. The device disclosed in U.S. Patent
No. 4,6~5,712 may be introduced into the heart through the
illofemoral artery thus avoid~ng major surgery and reducing the
riQ~ to the patient. However, adequate blood flow requires that
the pump and drive shaft be rotated at extremely high rpm through
the bends and sharp curves of the iliofemoral and aortic arteries
and therefore, extreme care must be taken to avoid creation of
hot spots in the arteries.
Another disadvantage associated with high rpm blood
pumps is the high ris~ of damaging a substantial percentage of
the blood cells of the blood. Damaged blood cells are expelled
by the body and new blood cells must be generated to replace
them. This may create additional strain on the system of a
patient who is already ~n critical condition. The prior art has
thus been unable to provide an easily implanted low risk
temporary circulatory assist pump capable of providing sufficient
blood flow to assist a heart so that the heart ~ay heal itself or
keep the patient alive while waiting for a transplant to become
available.
~JMM~RY ~ ~ TUVF:N'rr~ N
- The present invention is directed to a miniature
temporary circulatory assist pump adapted to be inserted in the
heart of the patient for circulatory assistance. The pump in a
preferred embodiment is introduced into the left ventricle of the
heart by a catheter passed through the arterial system of the
patient. The pump utilizes a helical-shaped foil impeller housed
within a cylindrical housing to deliver large volumes of blood at
relat$vely low rpm with$n a nominal physicological pressure.
2~2~3
DF!TATT.F:l) nF..C~,~TTCN ~F THF'. DRAWTl`lGS
So that the manner in which the above recited features,
advantages and objects of the present invention are attained and
can be underQtood in detail, more particular descriptlon of the
invention, briefly summarized above, may be had by reference to
the embodiments thereof which are illustrated in the appended
drawings.
Xt is to be noted, however, that the appended drawings
illustrate only typical embodiments of this invention and are
therefore not to be considered limiting of its scope, for the
invention may admit to other equally effective embodiments.
Fig. 1 is an illustrative view of a section of a human
heart depicting the preferred position of the pump of the
invention in the left ventricle of the heart;
Fig. 2 is a schematic view illustrating the insertion
of the pump of the invention through the femoral artery of a
patient;
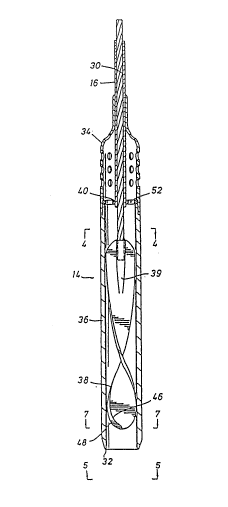
Fig. 3 is a partial sectional view of the pump of the
invention;
Fig. 4 is a sectional view of the pump o~ the invention
taken along line 4-4 of Fig. 3;;
Fig. 5 is a sectional view of the pump of the invention
taken along line 5-5 of Fig. 3;
Fig. 6 is an illustrative view of of the helical-shaped
foil impeller of the invention depicted in a two dimensional
plane; and
Fig. 7 is a sectional view of the pump of the invention
taken along lines 7-7 of Fig. 3.
i
nF~T~T.F.n n~ t`RTPTTON ~F' T~ PREF~!RRl;~n F.MROnTMF'.NT ;
Referring first to Figs. 1 and 2 of the drawings, the
blood pump of the invention is shown inserted in the left
ventricle 10 of the heart 12. The blood pump is generally
identified by the reference numeral 14 and is carried at the
2~2~3
forward end of a catheter 16. Acces-~ to the heart 12 is provided
in the preferred embodiment through the femoral artery 18. This
is the preferred insertion point, however, it is understood that
the heart 12 may be accessed through other arterie~ or other
su~gical means. In the prererred embodiment, the blood pump 14
is located in the left ventricle 10. However, in some
circumQtances it may be desirable to locate the blood pump 14 in
the right ventricle 20. Access to the right ventricle 20 may be
provided through the pulmonary artery 22. In operation, the
intake end of the blood pump 14 shown in Fig. 1 is located within
the left ventricle 10. The outlet or discharge end of the blood
pump 14 is located in the aorta 24. The blood pump 14 thus
extends partially into the left ventricle 10 through the heart
valve 26. Blood is pumped through the blood pump 14 from the
left ventricle 10 in the direction of the arrows 28 into the
aorta 24.
Referring now to Fig. 3, the pump 14 is shown in
greater detail. The pump 14 is driven by a flexible drive shaft
30 which extends through the catheter 16. The drive shaft 30 is
driven by a motor 31 located outside the patient's body, as best
shown ~n Fig. 2. The pump 14 is secured to the distal end of the
catheter 16. The pump 14 and catheter 16 are guided through the
femoral artery to the left ventricle 10. When the left ventricle
10 is reached, the pump 14 is positioned in the left ~entricle 10
of the heart. Ut~lizing known insertion techniques, the pump 14
is positioned so that the intake end 32 extends through the heart
valve 26 into the left ventricle 10. The discharge end 34 of the
pump 14 is positioned outside the left ventricle 10 so that
pumped blood is discharged into the aorta 24 as shown in Fig. 1.
In the embodiment of the invention shown in Fig. 3, the
pump 14 comprises a substantially cylindrical elongate housing
36. The intake end 32 of the housing 36 is blunted so that it
may be easily inserted into the left ventricle 10 past the heart
valve Z6 without damaging the heart valve or any of the heart
tissue. The inta~e end 32 is open so that blood collected in the
2~26~
left ventricle 10 may flow freely into the pump 14. Hou~ed
within the housing 36 is a helical-shaped foil impeller 38. The
impeller 38 is connected to the drive ~haft 30. The drlve shaft
30 i3 centrally po~$tloned within the discharge end 34 of the
housing 36 by a shaft stabilizer 40.
In the preferred embodiment as shown in Fig. 1, the
pump 14 ix positioned in the left ventricle 10 of the heart 12
and blood from the left ventricle 10 is pumped into the aorta 24
upon rotation of the lmpeller 38. The impeller 38 functions in
much the same fashion as an airfoil moving through a liquid
medium. Blasius' first equation of fluid forces on a body in
motion describes forces on a submerged body. The forces may be
resolved into components in directions perpendicular to the
motion (Y-axis) and parallel to the motion (X-axis). These
forces are known as "lift" and "drag" respectively. In fluid
mechanics, lift and drag are equal to the component of thrust.
~otation of the helical-shaped foil impeller 38 within the
cylindrical housing 36 produces characteristics similar to the
lift and drag forces produced by an airflow. That is, both high
and low pressure forces are produced on either side of the
rotating helical impeller 38 within the cylinder 36 which
produces a thrust force to energize fluid motion within the
cylinder 36.
Referring now to Fig. 6, impeller 38 is shown ~n a two
dimensional plane. It will be observed that the profile of the
impeller 38 is similar to that of an airfoil and includes a
forward or leading end 42 and a trailing end 44. ~he impeller 38
tapers from th~ leading end 42 to the trailing end 44. As the
impeller 38 is rotated, high and low pressure forces are created
on either æide of the rotating impeller. The high pressure side
is defined by the surface 46 and the low pressure side is defined
by the surface 48. The cord line 49 defines the angle of attack
of the impeller 38 which is optimized to provide maximum flow
rate at the physiological pressure level.
2~2~93
Referring now to Fig. 3, it will be observed that the
impeller 38 is wrapped or twisted to form a helical profile. The
forward end of the lmpeller 38 as best shown in Fig. 5 presents a
leading edge 50 which extends across the housing 36. From the
leadlng edge 50, the impeller 38 defines a continuous contour to
the tralllng end 44 a~ shown in Fig. 4. The contour deflnes a
continuous rotat~ng passage for transform~ng the blood flow from
a simple mass displacement at the inlet 32 to transformational
blood flow producing a thrust and a streamline shape at the
discharge end 34 of the pump 14. Tha transformational flow may
be calculated and graphically described utilizing the Joukowsky
transformation. Thus, the Joukowsky transformation may be used
to calculate the thrust generated by the rotational motion of the
impeller 38 within the housing 36. The rotational motion of the
impeller 38 creates a thrust force which draws blood into the
cylindrical housing 36 and discharges the blood through apertures
52 extending through the shaft stabilizer 40 and through ports in
the discharge end 34 i~to the aorta 24 for circulation through
the patient's vascular system. ~he trailing end 44 of the
lmpeller 38 is enlarged slightly at the central portion thereof
for connect~on to the drive shaft 30. ~he enlarged portion 39
however tapers outwardly to the trailing end 44 of the impeller
38 such that it does not interfere with the blood flow to the
discharge end 34 of the housing 36.
The helical-shaped foil prof~le of the impeller 38 is
designed to maximize blood flow through the housing 36 while
minim~zing the potential damage to blood cells. The impeller 38
is rotated in the range of 6,000 to 10,000 rpm to produce a blood
flow of approximately 3 to 4 liters per minute. Turbulence
however is minimized by the continuous contour of the flow
passage defined by the impeller 38. The thrust generated by the
high pressure side of the impeller 38 draws the blood through the
pump 14 while minimizing the turbulence in the blood flow. The
impeller 38 cooperates with the cylindrical housing 36 to form a
continuous, smooth, rotating passage to transform the blood flow
2 0 ~ 3
from a simple mass displacement at the inlet end 32 of the pump
14 to a transformational flow at the trailing end 44 of the
$mpeller 38. In this manner, trauma to the blood cells is
minimized, yet ~ufficient blood flow is developed to sustain the
patient.
Wh~le the foregoing i~ directed to the preferred
embodl~ent of the present lnvention, other and further
embodiments of the invention may be devised without departing
from the ba3ic scope thereof, and the scope thereof is determined
by the claims which follow.
W~T lS t`T.ATMl;:n TS-
--8--