Note: Descriptions are shown in the official language in which they were submitted.
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
MEDICAL DIAGNOSTIC APPARATUS WITH SLEEP MODE
BACKGROUND OF THE INVENTION
The present invention relates to medical diagnostic
devices, and particularly to battery-powered pulse oximeters.
Diagnostic monitors are used to monitor various
physiological parameters of a patient. In particular, such
monitors are used for heart rate, respiration rate, blood
pressure, temperature, and arterial oxygen saturation. Pulse
oximeters, for example, illustrate the different aspects of
such monitors, and are used as an example herein.
Pulse Oximeters are commonly used to monitor the
level of oxygen in the blood of a patient. This is
particularly critical during an operation, or during post-
operation recovery. In addition, pre-delivery monitoring of
the oxygen in a fetus provides important ir.iformation. A
typical oximeter directs light to the skin of a patient, with
either transmitted or reflected scattered light being
measured by a light detector. The amount of light detected
will be diminished by the amount of light absorbed by the
oxygen in the patient's blood. By using appropriate
wavelengths of light emitters, and their known absorption
characteristics along with appropriate mathematical
algorithms, the oxygen saturation of a patient can be
monitored.
Because of the need to quickly react to a change in
a patient's condition, it is oftentimes important for a pulse
oximeter to be in a continuous monitoring mode, with alarm
limits set to generate an alarm in case the patient exceeds
certain parameters. It is also desirable to be able to
provide a portable pulse oximeter so that it can be moved
from room to room without requiring it to be plugged in to a
power outlet. In such a portable pulse oximeter, power
1
CA 02241964 1998-07-02
WO 97/28739 PCTIUS97/01538
consumption is of concern, and it is desirable to minimize
the power consumption. Such a portable oximeter may not only
consume power in performing the measurements, but might also
transmit signals to a remote host computer for monitoring.
In a portable oximeter, such transmissions may be done using
wireless methods.
In one existing pulse oximeter, the Nellcor N-20, a
snapshot mode is provided. In this mode, the oximeter can be
turned on for a short period long enough to acquire a signal
and provide a pulse oximeter reading, and then automatically
shuts down. This method is useful primarily for taking a
reading of a healthy or stable patient, and is not useful for
a patient which requires continuing monitoring due to the
patient's condition. When the snapshot mode button is
pushed, five pulses are qualified and an oxygen saturation
and pulse rate are displayed. No more measurements are made
unless the snapshot button is pressed agair.. If the snapshot
button is not pressed for 30 seconds, the N-20 automatically
turns itself off. The N-20 also has an extended mode in
which it continuously takes data and calculates and displays
oxygen saturation and pulse rate.
The inventors of the present invention recognized
that sleep-mode techniques used in other technologies could
be imported into medical diagnostic devices, such as pulse
oximetry, under the appropriate conditions. In particular, a
sleep mode could be entered under carefully prescribed
conditions for short periods while a patiert's physiological
state is stable.
Sleep-mode techniques have been Lsed in other
technologies, notably for lap-top computerE which run on
batteries. In a typical sleep-mode, power to certain
components of the computer is turned off, cr they are slowed
down by reducing the clock speed, to reduce power
2
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
consumption. Typically, these take advantage of the fact
that a computer user is not always using the computer. Thus,
for instance, circuitry in the computer may detect the
absence of a keystroke for a certain amoun-_ of time, and
enter a sleep mode in response. Enough circuitry is left on
to detect an interrupt due to a keystroke, and the rest of
the circuitry is awakened on such an occurrence. Certain
microprocessors have a sleep or standby mode built in, with
some microprocessors being able to be shut down completely,
while others accept a vastly reduced clock speed. The
microprocessor will automatically save the state of its
registers and take any other action necessary to be able to
resume from where it left off in its program.
Certain aspects of a computer system may be
required to have power supplied to them constantly. For
instance, DRANI memory is required to be periodically
refreshed in order to save the memory contents. Other types
of memory which are non-volatile, and do not require
refreshing, are available. However, non-volatile memory is
typically much more expensive, and thus there is a cost/power
savings trade-off.
Sleep mode techniques have also been used in other
technologies. For example, Patent No. 4,77.6,463 discusses
the use of batteries to keep a television powered during a
power failure. Sleep mode is entered automatically upon
detection of a power failure. Patent No. 5,142,684 discusses
the use of a sleep mode in a portable bar code reader. U.S.
Patent No. 4,924,496 discusses the use of a sleep mode in a
telephone with incoming telephone call number display
capability,
A number of patents discuss various uses of a sleep
mode in an implantable device such as a pacemaker. Examples
include U.S. Patent No. 4,554,920, Patent No. 4,561,442, and
3
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
Patent No. 4,856,524. Clearly, in an implantable device
which is required to run on a battery, extending battery life
is important so that another operation is not necessary to
remove and replace the implanted device. Pacemakers can be
put into a sleep mode for a variety of conditions. In
particular, these patents discuss putting =he pacemaker into
a sleep mode during the refractory period, which is a period
between heart beats when the heart muscle is non-responsive
to electrical stimuli. U.S. Patent No. 4,404,972 discusses
not only implantable pacemakers, but also implantable devices
for controlling bladder function, producing muscle
contractions effective to combat scoliosis, to assist in
countering pain-producing nerve impulses, -and to control the
infusion of various solutions into the body. These devices
are all therapeutic, delivering material or energy to the
body at controlled times. They do not collect data for
diagnostic purposes, where the condition of the patient is
unknown.
SUMMARY OF THE INVENTION
The present invention provides a method and
apparatus for conserving power in a medical diagnostic
apparatus by using a sleep mode during a monitoring state.
The invention monitors a physiological parameter of the
patient and enters a sleep mode only after it has been stable
for a predetermined period of time. The apparatus is
periodically awakened from the sleep mode to take additional
measurements and to ascertain that the stability of the
physiological parameter has not changed. In one embodiment,
the sleep period is chosen to be consistent with the period
in which an alarm condition would need to be generated if a
patient's condition started to quickly change.
4
CA 02241964 1998-07-02
WO 97/28739 PCTIUS97/01538
The stable period during which saeep mode can be
used may vary depending on the type of diagnostic apparatus
and the characteristic being measured. Physical
characteristics can include the five vital signs: heart rate,
respiration rate, blood pressure, temperature and arterial
oxygen saturation. Blood constituents typically include
oxygen, carbon dioxide, blood glucose, hemoglobin
concentration and blood analytes, such as sodium, potassium,
chlorine, bicarbonate and blood urea nitrogen. Stability is
defined as a condition where one or more predetermined
variables change within a predetermined window of values
defined by a predetermined rule set, the rule set allowing
for the change to be measured in relative or absolute values,
and the rule set allowing for the passage of time to
constitute an integral part of the rules.
In one preferred embodiment, the apparatus is a
pulse oximeter, and both the blood oxygen saturation and
heart rate are monitored. These may be corisidered stable if
the heart rate does not vary by more than _,-20% and the blood
oxygen saturation does not vary by more than 2-10 saturation
percentage points for a predetermined stab3.e time period of
5-50 seconds (other preferred percentages and time periods
are set forth in the description of the preferred
embodiments). Upon attaining such stability, sleep mode can
be entered. In a preferred embodiment, the sleep period is
between 20 and 60 seconds, after which the pulse oximeter is
awakened for a sufficient amount of time to make new
measurements of blood oxygen saturation and heart rate.
Since the patient is presumed to still be stable, the pulse
oximeter does not need to use an initialization routine to
acquire pulses which would typically require at least five or
more pulses. Rather, data for 1-2 pulses (alternately, 1-15
pulses) is acquired and compared to the previously acquired
;:s
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
data before re-entering the sleep mode (assuming stability is
re-confirmed). If the patient has not remained stable, the
sleep mode is discontinued and continuous monitoring is done
until the patient is again determined to be stable.
In a preferred embodiment, a ma-ority of the pulse
oximeter electronic circuitry is turned off, excepting in
particular a memory storing the data acqui_red while the
patient was stable. Elements which are turned off in a sleep
mode include the CPU, the light emitting diodes and driver
circuitry, as well as the analog-to-digital converter
connected to the detector. Preferably, the circuitry is
turned off for a period of 20 seconds, and then awakened to
acquire data associated with two pulse maximums.
Alternately, the pulse oximeter could be put in a sleep mode
in between pulses, such as preferably during the diastolic
decay portion of a heart pulse (after the maximum and before
the minimum).
An additional requirement for entering sleep mode
in one embodiment is that the patient be stable at a "high"
saturation value. High is preferably defined as being a
predetermined amount higher than the alarni limit of the
oximeter for low saturation or heart rate.
For a fuller understanding of the nature and
advantages of the invention, reference should be made to the
ensuing detailed description taken in conjunction with the
accompanying drawings.
BRIEF DESCRIPTION OF THE DRAWINGS
Fig. 1 is a block diagram of a pulse oximeter with
sleep mode according to the present invention;
Fig. 2 is a flow chart of the automatic sleep mode
according to the present invention; and
6
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
Fig. 3 is a diagram of a heart pulse illustrating
periods during which sleep mode can be entered.
DETAILED DESCRIPTION OF THE PREFERRED EMBODIMENTS
The present invention applies to a diagnostic
device which enters a sleep mode while a patient is stable.
By way of example, a pulse oximeter is described, although
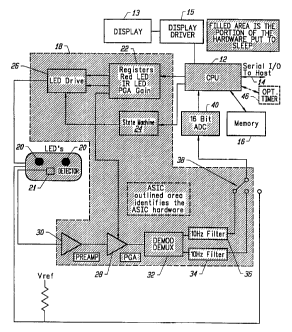
the invention could apply to any diagnostic device. Fig. 1
is a block diagram of one embodiment of a pulse oximeter
according to the present invention, illustrating an example
of the type of components which could be put into a sleep
mode to conserve power. The pulse oximeter includes a CPU 12
which may be connected by a serial I/O port 14 to a remote
host computer. Port 14 can either be a hardwired connection
or a wireless connection. CPU 12 is connected to its own
memory 14. The CPU is also connected to electronic circuitry
in the form of an Application Specific Integrated
Circuit (ASIC) 18 which includes the drive and detection
circuitry for a pair of Light Emitting Diodes (LEDs) 20 which
provide light to the patient's skin.
As shown, ASIC 18 includes a number of registers 22
and a state machine 24. State machine 24 offloads some of
the routine functions from CPU 12, such as the alternate
switching and controlling of power levels for the drive
circuitry 26 connected to the two LEDs 20. In addition, the
state machine 24 adjusts the gain of a programmable gain
circuit 28 which adjusts the signal detected in a light
detector 21 associated with LEDs 20 and pro-Jided through a
preamplifier 30. Typically, this gain is adjusted to take
maximum advantage of the range of the analog--to-digital
converter to provide more sensitivity for smaller signals,
and more range for larger signals.
7
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
Completing the circuitry is a demodulator/
demultiplexer 32 which provides the detected signal through
two different filters 34 and 36 and a switch 38 to an analog-
to-digital converter (ADC) 40..
During a sleep mode, all the elements shown in
Fig. 1 except for memory 16 are put into a sleep mode.
"Sleep mode" may mean the removal of power, or the use of a
lower power state, such as a slower clock frequency for
CPU 12.
The oximeter also has a display 13 and a display
driver 15. This will typically include a riumeric display of
the heart rate and the oxygen saturation. In addition, there
may be a bar graph which rises and falls wi.th the heart rate,
or a waveform display. In a sleep mode, some or all of the
display may be put into a sleep mode. Preferably, the
numerical displays continue to receive power and are active
in a sleep mode, while any bar/blip display and waveform
display is disabled. The CPU can thus provide the display
driver 15 with the latest data before the C'PU goes to sleep,
with display driver 15 staying awake and maintaining the last
data throughout the sleep mode period. Power is saved by
limiting the amount of display illuminated. Alternate
methods are possible, such as dimming the numerical display
during sleep mode or having a slow, blinking display to save
additional power. Preferably, the numeric display is
maintained constantly to make the sleep moae somewhat
transparent to the user.
When put into the sleep mode, the pulse oximeter
can be awakened by a signal from the remote host on I/O line
14 (which can be a wire or wireless telemetry connection).
Alternately, a stand-alone pulse oximeter may have its own
optional timer 46 which is set by the CPU before going into
sleep mode. The timer will then generate an interrupt to the
8
CA 02241964 1998-07-02
WO 97/28739 PCTIUS97/01538
CPU upon expiration of the sleep mode time to awaken the CPU.
Fig. 2 is a flow chart illustrating the automatic
sleep mode control flow of the present invention. It should
be noted that in addition to the automatic sleep mode, a
manual mode can be provided wherein the ho.st can provide a
signal to instruct the pulse oximeter to gc> into a sleep
mode, and remain there until awakened by the host. In such a
mode, the host would provide the necessary timing.
As shown in Fig. 2, in a first st.ep A, automatic
sleep mode is started. After the pulse oxi.meter is turned
on, it first determines whether a sensor i:; attached to the
oximeter (step B). If no sensor is attached, the pulse
oximeter is put into a sleep mode for one second, and then is
reawakened to test again whether a sensor is attached. Since
typically only around 200 microseconds are required to
determine if a sensor is attached, this provides a
significant power savings even though the sleep mode is for
only one second at a time. In this mode, the pulse oximeter
is thus asleep for around 800 of the time.
Once a sensor has been attached, the oximeter
searches for a detectable pulse pattern to lock onto or
"acquire." In this type of pulse oximeter, the cardiac pulse
is first detected so that the oximeter readings can be made
at the same position in subsequent pulses. This is done
because the volume of blood changes depending upon the
portion of the pulse, thus changing the oximeter reading due
to more light being absorbed with the presence of more
oxygenated blood in one portion of the pulse compared to
another. Once a pulse has been acquired, there is no longer
any pulse search, and the oximeter then proceeds to collect
blood oxygen saturation data and heart rate data (step E).
The data is continuously tested to see whether it passes the
stability test compared to previous samples during a 20-
9
CA 02241964 1998-07-02
WO 97/28739 PCTIUS97/01538
second period (step F). If at any time during the 20 second
period the stability test fails, the test is reset.
A 20-second stability period is chosen for the
preferred embodiment, although other periods of time may be
chosen, preferably 5, 7, 10, 15, 20, 25, 3C, 40 or 50
seconds, and most preferably at least 15-2C seconds. The
stability criteria in the preferred embodiment is that the
heart rate not vary more than 5%, although other variation
limits may be used, preferably no more thar. 20%, more
preferably 15%, more preferably 10%, optionally more than 50
or 30. The clinical empirical tests known to the inventors
show that a+/- 5 beats per minute (bpm) variation of heart
rate can be expected from a normal patient during the course
of oximetry monitoring. In addition to the heart rate, in
the preferred embodiment, the oxygen saturation value may not
vary more than two saturation points out of a maximum scale
of 100 in order to be stable. Alternately, this stability
limit is preferably chosen to be less than 1G, 8, 6, 5, 4, 3
or 2 saturation percentage points. The inventors have
determined by empirical test that a +/- 2% variation of
oxygen saturation (SAT) can be expected from a normal patient
during the course of oximetry monitoring. Alternately, the
saturation variation can be a percentage of the optimum
saturation for the patient or last saturation value. This
would be significant, for example, where a normal adult with
a saturation in the high nineties is compared to a fetus with
a saturation typically in the seventies or lower. An
absolute limit of 10s of a 100-point range produces different
percentage values of a normal saturation in a healthy adult
versus a fetus, and accordingly, different limits may
optionally be imposed.
If the patient is determined to he stable, sleep
mode is entered (step G). Sleep mode is entered by first
1 0
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
saving the baseline oxygen saturation valuE, (SAT) and heart
rate value in memory 16. The pulse oximeter then goes to
sleep for a period of 20 seconds in the preferred embodiment.
In the study of apnea, the normally accepted times when a
patient is to be checked are 15, 20 or 30 Seconds.
Preferably, the sleep period is no more than 60, 50, 40, 35,
30, 25, 20 or 15 seconds. Optionally, the same period of
time used to determine stability (preferab7.y 20 seconds) is
also used for the sleep period between checks of the patient
(also 20 seconds).
Upon awakening from the sleep mode, the saturation
and heart rate value are read for the next two complete
pulses (step H). These are compared to the baseline values
stored in memory from the stability period (step I). If the
values collected during the two pulses are within the
baseline value limits, indicating the patient is still
stable, sleep mode is reentered for another, 20 seconds
(step J). Otherwise, the continuous monitoring operation is
reinstated, and the sleep mode cannot be entered again until
at least 20 seconds of stable data have again been collected.
The two pulses read when the pulse oximeter awakes
from the sleep mode are preferably not used to adjust the
baseline value, though optionally they could be so used.
Keeping the baseline fixed prevents the baseline from slowly
changing without having to be stable for a 20-second period.
The number of pulses read upon awakening need not be two,
but is preferably 1, 2, 3, 5, 8, 10 or 15 pulses. In one
embodiment, if the oximeter has been in the sleep mode for a
series of 20 second periods, more time may be spent in the
awake state to re-establish the average, stable values, while
still realizing a significant power savings. This can be
done without a significant overall effect on power
consumption, since significant power savings have already
11
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
been achieved. For example, in one embodiment, if the
oximeter has been in a continuous series of: sleep modes for
more than 1-2 minutes, the oximeter could remain awake for 5
pulses, rather than 2, to establish and calculate a new
average heart rate and oxygen saturation. The awake periods
chosen can alternatively be time based, as opposed to pulse
based as previously described, in which case preferable awake
time periods could include any one of 1, 2, 3, 5, 8, 10, and
seconds, with 2, 3, and 5 seconds being preferred
10 embodiments. Some pulse oximeters use saturation calculation
algorithms which are not event based (e.g., pulse based) but
rather use data for saturation calculation without regard to
where the data is located relative to the cardiac pulse.
The limits for heart rate and blood oxygen
15 saturation to determine stability could be varied depending
upon a variety of factors. For example, the type of patient
could be used to vary the standard, especially for blood
oxygen saturation between a fetus and an adult. Alternately,
depending upon the method used to acquire the data, a
different limit could be used depending upon the amount of
averaging used in the evaluation method. The host computer
dynamically adjusts these limits in one embodiment.
In one embodiment, the pulse oximeter is not
allowed to go into sleep mode unless the patient is stable at
a"high" saturation value. "High" could be defined as a
predetermined number, or in relation to a l.ow alarm limit, if
one is used. For example, high could be greater than 90 or
95 saturation points for an adult, and greater than 50, 55,
60, or 65 for a fetus. Alternately, high could be 5, 10 or
15 saturation points above a low alarm limit, which could be,
i.e., 70, 75, 80, 85, 90 or 95 for an adult, or 10, 15, 20,
25, 30, 35, 40, 45, 50, 55, 60 or 65 for a fetus. Similarly;
sleep mode could be restricted if the heart rate is outside
12
CA 02241964 2004-10-05
.a predetermined range, or if any other monitored
physiological parameter is outside a predetermined range.
The host can adjust the high saturation and heart rate test
settings, depending on the type of patient being monitored,
the condition of the patient, whether the patient is awake or
asleep, or for any other reason.
In addition, other aspects of the pulse oximeter
operation may be modified during a sleep mode. In
particular, a pulse oximeter includes alarm limits, such as
an alarm which may be generated if no pulse is detected for a
predetermined period of time (such as 10 seconds). It may be
desirable to impose a shorter limit upon awakening from a
sleep mode since the condition may have been continuing
undetected some time prior to the awakening. In one
embodiment, the "no pulse" alarm will be generated if no
pulse is detected for 5 seconds after awakening, as opposed
to the normal 10 seconds.
A description of different states an oximeter
could be in, including noise, motion and alarm states, is
set.forth in U.S. Patent No. 5,368,026 (the "'026
patent"). Optionally, an oximeter may be required to be
in a normal state, as set forth in the '026 patent, for a
period of 20 seconds before sleep mode is entered. In
another embodiment, sleep mode is allowed in the presence
of motion, but upon awakening from the sleep mode, it must
be additionally determined that motion is absent long
enough to confirm stable readings before the oximeter is
put back to sleep.
A manual or remotely controlled sleep mode is also
provided, where the host computer controls when the oximeter
is put to sleep and when it is awakened. The host computer
mav receive inputs from other monitors, such as an EKG oraa
13
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
C02 monitor, and could use heart rate information derived
from these, for instance, to determine if a patient is
stable. The C02 monitor could also provide an indication of
the amount of oxygen the patient is receiving. The host
could also be operated in response to a human operator
viewing the patient through a remote TV monitor, or the human
operator could simply decide the patient doesn't need to be
monitored while awake and/or during the daytime, or only
periodically during the night, or for other reasons. In one
embodiment, the host can periodically determine stability
separately from the pulse oximeter monitor with data from
other sources, eliminating the need for the pulse oximeter to
establish or reconfirm stability itself.
Preferably, the pulse oximeter responds differently
to a command from the host computer to go into sleep mode,
depending on the mode the pulse oximeter is in. If the pulse
oximeter does not have a sensor attached, it will wake itself
from the sleep mode every second to check for a sensor
attached, and will continue sending no sensor attached
messages to the host. If the oximeter is in the middle of
performing a noise measurement when it receives the sleep
command, it will preferably complete that measurement and
defer entering the sleep mode for up to 2 seconds. If the
oximeter is in the process of adjusting LED brightness or
amplifier gains, sleep mode may be deferred for up to one
second.
Depending on the state the oximeter was in when it
received a sleep mode command from the host, it will respond
differently when it is awakened by the host. If was doing a
pulse search, it will continue the pulse search upon being
awakened. If it was reporting valid SAT and heart rate
information, it will wait for the next good pulse. If a good
pulse is detected in 10 seconds, it will ccntinue with normal
14
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
pulse oximetry measurementse If no good pulse is detected in
seconds, a pulse time out occurs, with an alarm being
generated, unless a probationary state has been entered for
motion as set forth in the 1026 Patent.
5 Upon reawakening the pulse oximeter from a manual
sleep mode, it can go into an automatic sleep mode operation.
Preferably, the oximeter must always cycle through a normal
monitoring mode (20 seconds) before entering an automatic
sleep mode after a manual sleep mode.
10 Fig. 3 is a diagram of the optical pulse which may
be received by the pulse oximeter. This waveform 50 includes
a series of peaks 52, 54, and 56, along with intervening
minimums 58, 60, and 62. Typically, the pulse oximeter
measurements are made on the rising edge of the pulse
oximeter waveform, such as between minimum 58 and maximum 54
or between minimum 60 and maximum 56. Accordingly, in an
alternate embodiment, the pulse oximeter could be put to
sleep during a diastolic decline after a maximum and before
the next minimum. For example, the sleep mode could be
entered in the period between dotted lines 64 and 66 for each
pulse. Preferably, a margin of at least 50 of the length of
the trailing edge of the pulse is used after the maximum and
before the expected minimum to allow for variations in the
occurrence of the minimum and to avoid false peak triggering
on the maximum. Since the trailing edge of the pulse is
typically 75% of the total pulse time, this sleep mode can
produce a significant power savings.
To achieve additional power savings, the two
techniques can be combined. That is, during normal
operation, when it is being determined if a patient is
stable, the pulse oximeter could still sleep between points
64 and 66 for each pulse. Since only the rising edge of the
pulse wave form is needed, this would not degrade the
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
determination of blood oxygenation and heart rate so long as
the pulse does not vary so much from pulse to pulse that the
sleep window ends up extending beyond the falling edge. This
can be avoided by providing sufficient margin for the next
anticipated minimum to reawaken from sleep mode. Upon
entering a normal sleep mode, the operation of the pulse
oximeter to acquire data during two pulses could also be put
to sleep during the falling edges of those two pulses to
further conserve power.
As will be understood by those with skill in the
art, the present invention may be embodied in other specific
forms without departing from the spirit or essential
characteristics thereof. For example, only some of the
electronic circuitry put to sleep might be awakened for a new
measurement. Alternately, the circuitry might be awakened
only to do a measurement, and not to determine stability, or
vice-versa. For instance, stability might be re-verified
only after several sleep periods. In another example, a
sleep mode could be used for a heart rate monitor, a blood
pressure monitor, a respiration monitor, a temperature
monitor, or any other type of diagnostic monitor. A
respiration monitor, for example, could sleep for a period of
time similar to that for a pulse oximeter. Sleep mode could
be restricted, for example, based on the carbon dioxide
content of the patient's exhaled breath. A temperature
monitor, for example, could have a much longer sleep mode,
since temperature changes occur much slower than oxygen
deprivation, which could occur very quickly. A blood
constituent monitor could alternately monitor carbon dioxide;
blood glucose; hemoglobin concentration; and blood analytes,
such as sodium, potassium, chlorine, bicarbonate, and blood
urea nitrogen. Alternately, the circuitry could be
distributed, with wireless connections, and only portions
16
CA 02241964 1998-07-02
WO 97/28739 PCT/US97/01538
subject to the sleep mode. Accordingly, the foregoing
description is illustrative of the invention, but reference
should be made to the following claims which set forth the
scope of the invention.
17