Note: Descriptions are shown in the official language in which they were submitted.
r.. .... .r- .. . .-..r ......... . ... _..,..,_ ... ......~ rrv.rv. . . "T
CA 02270932 1999-OS-06
I
pull Back Scent )delivery System With Pistol Grip Retraction Handle
Baekgtround o the Inye 'on
1. )~ipld of t a Inventing
The present invention relates to an improved wire pull back delivery
system. More specifically, the invention relate to a wire pull-back scent
delivery systam
which utilizes a pistol grip retrac.~tion handle to retract the retractable
outer sheath and
deploy a:nedical implant for W ninim,ally ln~wsive application, such as an
endovascular
stent grat<, versa cai-a filter, self-expanding scent, balloon expandable
scent, or the tike.
2, Tlp~.~r;ntinn Of the Bela ed Art
IO Delivery system for deployi,-tg medical implants, such as an endovascular
scent graft, ,~ena cava filter, self-expanding stem, balloon expandable scent
or the like, arc
a highly developed and well known field of medical technology. These medical
devicxs
>7ave many well known users and applications. In particular, a scent is a
prosthesis which
is generally tui;ular and which is axpanded radially in a vessel or lumen to
maintain its
I 5 patency. Stents are widely used in body vessels, body canals, ducts or
other body
lumens. A self-expanding scent is a stmt which expands from a compressed
delivery
position to its original diameter when released from the delivery device,
exerting rfuiial
force un the ;;onstricted portion of the body lumen to re-establish patency.
One common
sell-exptwding 5~t;,nt is raaattfactured of Nitirol, a nickel-titanium shape
memory a.Iloy,
%0 .which can be formed and anre3.led. deformed at tt low temperature, and
recalled to its
original sr~ape with heating. such as when deployed at body temperatuxe in the
body.
Wire pull-back scent delivery systems are disclosed in US 5360401 and
1.'S 5571135. One important factor in delivering the stent is a controlled
precise
retraction of the retractable outer sheath. What is necdrd i~ a wli~e pull-
back scent
ZS delivtty system which pcovidcs For a controlled and precise retraction of
the retractable
cuter sheath and cnahles the physici2r. to accurately determine proper
positioning of the
stint, as well as track the retraction of the cout~r sheath.
EP 1127201 shows a catheter for delivery of a medical device, with a
retractable outer sheath. US Sz49~30 shows a balloon catheter with radiopaque
markers
30 on the guide wire and catheter. E)? S 1883 $ shows an implantation device
with an
aperatin~ rz2eaixs ~ located at the proximal end of the device.
%0
~nmmurv of the Invention ~t~,C~G
P
CA 02270932 1999-OS-06
WO 98/23241 PCT/US97/20589
2
The inventive stmt delivery system for delivering a self expanding stem
to a predetermined location in a vessel includes a catheter body having an
axial
guidewire lumen and a pull-wire lumen. A medical device such as a self
expanding
stmt is held in a reduced delivery configuration for insertion and transport
through a
body lumen to a predetermined site for deployment. The stmt is carried axially
around
the catheter body near its distal end and held in its reduced conf guration by
a
retractable outer sheath. A proximal retraction handle is connected to the
proximal end
of the catheter body and includes a pistol grip trigger engaging a racket
mechanism,
which is connected to a pull-wire which extends through the pull-wire Lumen
and is
connected to the retractable outer sheath.
Brief Description of the Drwvin~s
A detailed description of the invention is described below with specific
reference being made to the drawings, in which:
Figures 1 and 2 are side views of the inventive stmt delivery system;
Figure 3 shows the distal end of the inventive stmt delivery system;
Figure 4 is a cross-sectional view of the catheter body taken along
section line 4-4 of Figure 3;
Figure 5 is a cross-sectional view of the catheter body taken along
section line S-S of Figure 3;
Figures 6-8 show details of Figure 3 in greater detail;
Figure 9 shows the connection of the pull-wire to the strip portion of the
racket mechanism;
Figure 10 shows the Y-luer;
Figure 11 shows one side of the two-piece snap fit proximal retraction
handle with its components in place;
Figure 12 shows the other side of the two-piece snap fit proximal
retraction handle with the strip retracted into a channel;
Figure 13 and 14 show the delivery system partially and fully deployed;
Figure 15 shows the flexible ratcheting pawl in more detail, and
Figures 16 and I7 show an alternate embodiment for attaching the pull-
wire to the pull-ring.
CA 02270932 1999-OS-06
WO 98/23241 PCT/US97/20589
3
Description of the Preferred >!smbodiment
While this invention may be embodied in many different forms, there are
shown in the drawings and described in detail herein a specific preferred
embodiment of
the invention. The present disclosure is an exemplification of the principles
of the
invention and is not intended to limit the invention to the particular
embodiment
illustrated.
Figures 1 and 2 show side views of the inventive delivery system. The
preferred embodiment discussed below specifically discusses delivering a self
expanding stmt, but it should be understood that the inventive delivery system
can
I O deliver any medical implant for a minimally invasive application, such as
an
endovascular stmt graft, vena cava filter, self expanding stmt, balloon
expandable stmt
or the like.
The preferred embodiment is a two-part system including an implantable
medical device such as a self expanding stmt and a delivery catheter. The
delivery
15 catheter is shown generally at i 0 and includes the catheter body 12, the
retractable outer
sheath 14 and the proximal retraction handle 16.
Figure 3 shows the distal end of the delivery system 10, and the
retractable outer sheath 14 in more detail. A medical device is held in its
delivery
configuration by outer sheath 14, and in the preferred embodiment the medical
device is
20 a self expanding stmt 18 which is carried concentrically around the single
lumen
extrusion 35 near the distal tip 20.
Figure 4 shows that catheter body 12 is a tri-lumen catheter, and in the
preferred embodiment is a nylon extrusion with a guidewire lumen 22, a stent
flushing
lumen (priming port) 24 and a pull-wire lumen 26. The guidewire lumen
25 accommodates a .035 inch guidewire 28. The guidewire lumen 22 and stmt
flushing
lumen 24 terminate at the point shown generally at 30, and a stainless steel
pull-wire 32
is shown extending from the pull-wire lumen 26 and which attaches to a
stainless steel
ring 34 (best seen in Figure 6). A nylon single lumen (guidewire lumen)
extrusion 35 is
thermally lap welded to the catheter body 12 at point 30 and has a nylon
extrusion
30 which is thermally molded to the distal end of the nylon single guidewire
lumen 35 and
tapered to create smooth atraumatic tip 20.
CA 02270932 1999-OS-06
WO 98/23241 PCT/US97/20589
4
Figure 5 shows a. cross-section view, of the single guidewire lumen
extrusion 35 along section lines 5-5 of Figure 3.
In the preferred embodiement, tantalum radiopaque marker bands 36 and
38 are bonded to the single lumen extrusion 35 using cyanoacrylate adhesive,
although
it should be understood that marker bands 36 and 38 could be attached using
other well
known techniques such as weld swaging or crimp/swaging. Marker bands 36 and 38
are
used in connection with an imaging procedure to aid in determining proper
positioning
of the stmt in the body lumen. Although fluoroscopy is the most common imaging
procedure typically employed, x-ray, MRI or any other well known imaging
techniques
may also be utilized. In the embodiment of Figure 3 marker bands 36 and 38
show the
proximal and distal ends of the stent 18 as carried in its delivery
configuration. An
alternate embodiment may locate marker bands 36 and 38 to mark the proximal
and
distal ends of the stmt 18 in its expanded position, which would have a
slightly shorter
length than the stent in its delivery configuration. A nylon band stmt stop 40
is also
bonded to the single lumen extrusion 35 and prevents the stmt 18 from moving
proximally along the single lumen extrusion 35 as the outer sheath 14
retracts, assisting
in accurate stmt placement. Stop 40 could also be attached using any standard
technique, such as overmolding or ultrasonic welding.
In the preferred embodiment the retractable outer sheath 14 is a clear
medical grade PTFE (polytetrafluoroethylene) extrusion which covers the distal
10-20
cm (depending on stmt length) of the catheter body 12. However the outer
sheath 14
could be made of any suitable fluropolymer material. A specific alternate
embodiment
could utilize a fluropolymer material which is transparent to visible light to
enable the
operator to directly view deployment in an endoscopic delivery procedure. Such
materials are well known in the art. In the preferred embodiment self
expanding nitinol
stems of from 6-14 mm in diameter and ranging from 20-100 mm in length can be
accommodated. It should be understood that any type of self expanding stmt
could be
employed, although nitinol self expanding stems are preferred. The retractable
outer
sheath 14 is connected to the proximal retraction handle 16 by stainless steel
pull-v~~ire
32 which is welded to stainless steel ring 34 (best seen in Figure 6). Ring 34
is swaged
in place to the outer sheath 14 with tantalum radiopaque marker band 42. The
distal
CA 02270932 1999-OS-06
WO 98/23241 PCT/US97/20589
end of retractable outer sheath 14 is designed to flush fit with tip 20 to
create a smooth
profile. The proximal end of retractable outer sheath 14 is finished with a
smooth
transition consisting of a thermally molded nylon extrusion swaged in place
with a
tantalum radiopaque marker band 44 (best seen in Figure 7). It should be
understood
S that tapered transition could be molded in place, which would eliminate the
need for a
marker band swaged in place to attach the nylong extrusion. It should also be
understood that the marker band could be bonded or crimp/swaged. The tapered
smooth transition of the proximal portion of outer sheath 14 allows catheter
body 12 to
be more easily extracted from the body lumen and introducer sheath. The
proximal end
of retractable outer sheath 14 slidably seals to catheter body 12 permitting
it to slide
proximally along catheter body 12 when retracted by pull-wire 32. The nitinol
stmt 18
is compressed at low temperature for loading into delivery system 10 and held
in its
reduced delivery configuration by retractable outer sheath 14. Upon deployment
in vivo
at body temperature the original stmt shape is restored as the nitinol stent
self expands,
exerting radial force on the constricted portion of the body lumen to re-
establish
patency. Marker band 45 is also bonded to extrusion 35 approximately one stmt
length
proximally of marker band 42 (in the unretracted position) and is utilized to
confirm full
stmt release as discussed further below. It should be understood that marker
band 45
could also be attached using swaging or crimp/swaging.
Figures 6-8 show details of Figure 3 is more detail.
Referring again to Figures 1 and 2, the stmt 18 is deployed using
proximal retraction handle 16. Proximal retraction handle 16 is a mufti-
component
assembly ergonomically designed with a pistol grip trigger 46. The trigger
mechanism
46 is contained within a two-part molded ABS (acrylonitrile, butadiene,
styrene) outer
housing that is snap-fit together. The ABS trigger 46 has a polypropylene
safety lock
mechanism 48 to prevent inadvertent stmt release. The proximal retraction
handle 16 is
connected to the catheter body 12 by the pull-wire 32, a Y-luer assembly shown
generally at 50 and a strain relief 52.
Referring now to Figure 9, catheter body 12 is connected to strain relief
52, and the proximal end of pull-wire 32 exits from lumen 26 and is threaded
and
crimped to a strip 54 by crimp tube 56, which is part of the ratchet mechanism
used to
CA 02270932 1999-05-06
WO 98/23241 PCT/US97/20589
6
retract outer sheath 14. Strain relief 52 is made of Pebax~ and is insert
molded over
catheter body 12, and is constructed to fit inside the nose of proximal handle
16 (best
seen in Figures 11 and 12).
Referring now to Figure 10, the Y-luer assembly SO is shown, and
S consists of a nylon Y-luer with a nylon single lumen extrusion overmoided to
each leg
of the "Y". It should be understood that the extrusion could also be bonded to
each leg
of the "Y". Leg 58 of the "Y" forms the stmt flushing port and leg 60 forms
the
guidewire port. Each single lumen is thermally lap welded to the catheter body
12 and
provides communication between the Y-luer and the guidewire lumen 22 and the
stmt
flushing lumen 24. The stmt flushing lumen is used to fill the retractable
outer sheath
14 with fluid to purge air out of the outer sheath 14 prior to insertion of
the catheter
body 12 into the body.
Referring now to Figure 11, the proximal retraction handle 16 is shown
in more detail and is a mufti-component assembly ergonomically designed with a
pistol
grip 46, which is engaged by trigger spring 62. The pistol grip 46 or trigger
has two
cylindrical protrusions 64 on either side of trigger 46 which extend outwardly
and are
received by pivot mounts molded into the proximal retraction handle 16 to
attach the
pistol grip 46 to the handle 16 as well as provide a point about which the
pistol grip
rotates. A trigger stop 66 defines the normal trigger position and the trigger
46 is
maintained in this normal position by trigger spring 62. As the trigger 46 is
squeezed it
rotates to its compressed position, and when released the trigger spring
forces the trigger
to rotate back to its normal position flush with the trigger stop 66. Trigger
46 includes a
pair of gear engaging members 68 which are spaced apart to form a channel wide
enough to receive the larger gear 72 of gear 70. Gear 70 includes gear 72 and
a pair of
gears 74 fixedly attached on either side of gear 72. Gears 74 engage the gear
engaging
portions 68 of trigger 46 to rotate gear 70 as trigger 46 rotates. Axle 76 is
received by
molded mounts in the two parts of handle 16 to attach the gear to the handle
16. Gear
72 engages the ratchet mechanism which is attached to the pull-wire 32. The
ratchet
mechanism is comprised of a rack driver which is comprised of 2 parts, a rack
80 and a
rack tab 82, which snap fit together, to form a channel for receiving strip
84. As can be
seen best in Figure 15, strip 84 contains ramp shaped stops 86, each adjacent
pair of
CA 02270932 1999-OS-06
WO 98/23241 PCT/US97/20589
7
stops forming detents 88 (best seen in Figure 15). Rack tab 82 contains a
flexible
ratcheting pawl 89 which engages with detents 88 such that when the rack
driver is
moved proximally when the trigger 46 is squeezed to its compressed position,
strip 84 is
moved proximally, but when the rack driver is moved distally when trigger 4G
is rotated
to its normal position, the flexible ratcheting pawl 89 slides up ramp shaped
stop 86 to
disengage from strip 84.
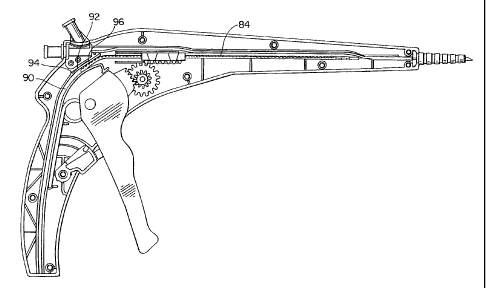
As is best shown in Figure 12, strip 84 is received by channel 90. A
second spring, strip spring 92 is securely held to handle 16 by tail 94 and
its locking
head portion 96 lockingiy engages with detents 88 to hold strip 84 in place
when trigger
46 is released and rack tab 82 is moved distally to lockingly engage with the
adjacent
distal detent 88. The ramp shaped stops 86 (best seen in Figure 15) allow the
strip to be
moved proximally in channel 90 by rack tab 82 until the adjacent detent
lockingly
engages with strip spring 92. The detents are each approximately 2 mm apart so
that
each complete squeeze of the trigger 46 retracts the pull-wire 32 and outer
sheath 14
approximately 20 mm. By repeatedly squeezing and releasing trigger 46 the
outer
sheath 14 is fully retracted to release the stmt 18 to self expand. The rachet
mechanism
is designed to work with any stent of lengths between 20 and 100 mm, although
it could
easily be designed to accept any desired length stmt.
The ratio of gear 70 in the embodiment shown in Figure 12 is 2:1, such
that a 1 mm squeeze on trigger 46 retracts the outer sheath 2 mm. However, it
should
be understood that any desired gear ratio could be utilized. For example gear
70 is
designed optionally to allow for a gear ratio of 1:1. In that embodiment a
trigger 46
with a single gear engaging portion 68 is designed to engage gear 72, rather
than gears
74, to provide a 1:1 ratio such that a 1 mm squeeze on the trigger will
retract the outer
sheath 14 1 mm. In order to accommodate this detents 88 would be spaced
approximately 1 mm apart on strip 84 and it should be understood that the
stops 86 and
detents 88 could be arranged in any desired spacing. Gear 70 could also be
designed if
desired to have a ratio of 1:2, such that a 2 mm squeeze of trigger 46
retracts outer
sheath 14 1 mm.
In operation, pre-placement imaging or other standard procedure is
normally performed to identify an insertion tract and assess the site. A
guidewire (.035
CA 02270932 1999-OS-06
WO 98/23241 PCT/US97/20589
inch diameter in the preferred embodiment) 28 is maneuvered through the tract.
The
delivery system 10, with the preloaded medical device (a self expanding stmt
in the
preferred embodiment) is then passed through an introduces sheath and tracked
over the
guidewire until the medical device is positioned as desired. In the preferred
embodiment markers 3G and 38 are used with standard imaging techniques such as
fluoroscopy, x-ray, MRI or the like to aid in proper positioning of the stmt
18 across the
stricture. As the trigger 46 is repeatedly squeezed, the outer sheath 14 is
retracted
proximally to release the stmt to self expand. To aid in confirming complete
stent
deployment and release the operator observes marker 42 move to meet marker 45.
I O Figures 3, 13 and 14 show the distal end of delivery system I 0 in a pre-
deployed state (Figure 3), partially deployed state (Figure 13) and fully
deployed state
(Figure 14).
Referring now to Figures 16 and 17, an alternate embodiment of the
inventive delivery system is shown where the pull-wire 32 is U-shaped with the
U loop
portion I00 of the pull-wire 32 looping around a notch 102 in the pull-ring
34. The 2
ends of the U-shaped pull-wire extend through pull-wire lumen 2G to attach to
the
ratchet mechanism. As shown in Figure 17, if desired a plurality of pull-wires
32 could
by looped around a plurality of notches 102 spaced around pull-ring 34. A
second pull-
wire lumen could be provided to carry one or more pull-wires 32 to allow the
pull-ring
to be retracted with the pulling force more evenly distributed around the pull-
ring
perimeter. Two U-shaped pull-wires 32, each carried by a separate lumen and
each
looping around pull-ring 34 as shown in Figure 17 would provide 4 points
arranged
around pull-ring 34 to more evenly distribute the pulling force on the pull-
ring. Each
pull-wire lumen could also optionally carry more than 1 pull-wire to provide
as many
attachment points on pull-ring 34 as desired.
This completes the description of the preferred and alternate
embodiments of the invention. It is to be understood that even though numerous
characteristics and advantages of the present invention have been set forth in
the
foregoing description, together with the details of the structure and function
of the
invention, the disclosure is illustrative only and changes may be made in
detail,
especially in matters of shape; size and arrangement of parts within the
principals of the
CA 02270932 1999-OS-06
WO 98/23241 PCT/US97/20589
9
invention, to the full extent indicated by the broad, general meaning of the
terms in
which the appended claims are expressed. Those skilled in the art may
recognize other
equivalents to the specif c embodiment described herein which are intended to
be
encompassed by the claims attached hereto.