Note: Descriptions are shown in the official language in which they were submitted.
CA 02288465 1999-11-04
-1-
SINGLE BREATH INDUCTION ANESTHESIA APPARATUS
The present invention relates to improvements in the field of
anesthesia. More particularly, the invention is concerned with a single breath
s induction anesthesia apparatus. Single breath induction anesthesia is also
often referred to in the litterature as vital capacity induction anesthesia.
When it is necessary to anesthetise a patient, it is highly
desirable to pre-oxygenate the patient prior to inducing anesthesia in order
to
~o increase the pulmonary alveolar partial pressure in oxygen so as to
increase
the safety of the induction anesthesia as well as of a subsequent ventilation
and endotracheal intubation. Pre-oxygenation of the patient is carried out by
using a parallel oxygen supply and breathing system connected by means of
a conduit to a face mask affixed to the patient. Due to the complexity of
such a technique, pre-oxygenation is often skipped.
In the case where pre-oxygenation is effected, while the
patient is being pre-oxygenated, the doctor usually closes with his hand the
distal end of the conduit connected to an anesthesia machine and adapted to
zo deliver an oxygen/anesthesia gas mixture to the patient, during operation
of
the anesthesia machine, so as to permit the anesthesia gas in the mixture to
reach a preset concentration sufficient to induce anesthesia of the patient
with a single breath. Since it is often impossible to close with one's hand
the
anesthesia gas conduit in a gas-tight manner, leaks of anesthesia gas can
z5 occur, which pollute the operating room. In addition, since the doctor has
only one hand free, he is limited in his movements to perform other tasks.
When the desired concentration of anesthesia gas has been reached, the
oxygen conduit is disconnected from the face mask and the anesthesia gas
conduit connected thereto. Alternatively, the face mask which is connected
3o to the oxygen supply and breathing system is removed and another face
mask to which the anesthesia gas conduit has been connected is affixed to
the patient. After induction of anesthesia, the face mask is then removed
from the patient's face to permit the installation of a ventillation device
such
as an oropharyngeal airway, an endotracheal tube or a laryngeal mask.
35 During these disconnection and connection of conduits and removal of the
CA 02288465 1999-11-04
-2-
face mask, important leaks of anesthesia gas occur, which significantly
pollute the operating room.
It is therefore an object of the present invention to overcome
s the above drawbacks and to provide a single breath induction anesthesia
apparatus which readily permits pre-oxygenation of the patient and single
breath induction anesthesia thereof, without causing pollution of an
operating room with anesthesia gas.
~ o In accordance with the invention, there is thus provided a
single breath induction anesthesia apparatus for anesthetising a patient,
comprising gas delivery means for delivering at least one gas to the patient,
and an oxygen supply system for providing oxygen and an
oxygen/anesthesia gas supply system for mixing oxygen and at least one
anesthesia gas at a preset optimum ratio sufficient to induce anesthesia of
the patient with a single breath, thereby providing an oxygen/anesthesia gas
mixture. The apparatus of the invention further includes a valve for
providing selective gas flow communication between the oxygen supply
system and the gas delivery means or between the oxygen/anesthesia gas
zo supply system and the gas delivery means. The valve is operable for first
establishing gas flow communication between the oxygen supply system and
the gas delivery means to deliver oxygen to the patient and permit pre-
oxygenation thereof, while inhibiting gas flow communication between the
oxygen/anesthesia gas supply system and the gas delivery means to allow
z5 the oxygen/anesthesia gas mixture to reach the preset optimum ratio, and
thereafter establishing gas flow communication between the
oxygen/anesthesia gas supply system and the gas delivery means to deliver
the oxygen/anesthesia gas mixture to the patient and permit single breath
induction anesthesia thereof, while inhibiting gas flow communication
3o between the oxygen supply system and the gas delivery means.
According to a preferred embodiment, the valve comprises a
valve body having a first port in gas flow communication with the oxygen
supply system, a second port in gas flow communication with the
3s oxygen/anesthesia gas supply system and a third port in gas flow
CA 02288465 1999-11-04
-3-
communication with the gas delivery means, and a valve member within the
valve body. The valve member is movable between a first position whereat
the first port is in gas flow communication with the third port and the second
port is closed, and a second position whereat the first port is closed and the
s second port is in gas flow communication with the third port. Preferably,
the
valve body has first, second and third tubular branches, the first, second and
third ports being defined at respective proximal ends of the first, second and
third tubular branches, respectively.
~o According to another preferred embodiment, the second and
third ports are generally disposed along a first axis and the first port is
generally disposed along a second axis extending transversely of the first
axis. The second and third tubular branches extend along the first axis and
the first tubular branch extends along the second axis. In such an
~s embodiment, the valve member preferably has a T-shaped gas passage
formed therein.
According to a further preferred embodiment, the first and
second ports are generally disposed along a first axis and the third port is
zo generally disposed along a second axis extending transversely of the first
axis. The first and second tubular branches extend along the first axis and
the third tubular branch extends along the second axis. In such an
embodiment, the valve member is preferably rotatably mounted in the valve
body for movement about a rotation axis which is co-axial with the second
z5 axis.
According to yet another preferred embodiment, the valve
includes stop means for arresting the movement of the valve member at each
of the first and second positions. Preferably, the stop means each comprise
3o cooperating abutment means disposed on the valve member and the valve
body.
According to still another preferred embodiment, the first
tubular branch is provided with gas vent means for venting excess oxygen,
3s or venting gases exhaled by the patient during pre-oxygenation when the
CA 02288465 1999-11-04
-4-
valve member is in the first position. The first tubular branch preferably
comprises a first tubular section and a second tubular section which is
removably connected to the first tubular section by means of a bayonet-lock
type mechanism. Preferably, the second tubular section is provided with a
s gas outlet having a gas vent orifice defining the gas vent means. Thus, when
pre-oxygenation of the patient has been completed, the second tubular
section to which the oxygen supply system is connected can be disconnected
from the first tubular section and removed.
~o Due to the provision of the aforesaid valve enabling selective
gas flow communication between the oxygen supply system and the gas
delivery means or between the oxygen/anesthesia gas supply system and the
gas delivery means, the apparatus according to the invention permits pre-
oxygenation of a patient and single breath induction anesthesia thereof,
without causing pollution of the operating room with anesthesia gas.
The present invention therefore also provides, in another
aspect thereof, a single breath induction anesthesia valve adapted to be used
with gas delivery means for delivering at least one gas to a patient, with an
zo oxygen supply system for providing oxygen and with an oxygen/anesthesia
gas supply system for providing a gas mixture containing oxygen and at
least one anesthesia gas at a preset optimum ratio sufficient to induce
anesthesia of the patient with a single breath. The valve according to the
invention comprises a valve body having a first port adapted to be in gas
Zs flow communication with the oxygen supply system, a second port adapted
to be in gas flow communication with the oxygen/anesthesia gas supply
system and a third port adapted to be in gas flow communication with the
gas delivery means, and a valve member within the valve body. The valve
member is movable between a first position whereat the first port is in gas
3o flow communication with the third and the second port is closed, whereby to
permit delivery of oxygen to the patient and pre-oxygenation thereof, and a
second position whereat the first port is closed and the second port is in gas
flow communication with the third port, whereby to permit delivery of the
oxygen/anesthesia gas mixture to the patient and single breath induction
35 anesthesia thereof.
CA 02288465 1999-11-04
-5-
Further features and advantages of the invention will become
more readily apparent from the following description of preferred
embodiments thereof as illustrated by way of examples in the accompanying
drawings, in which:
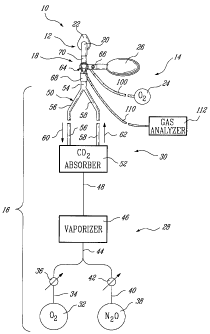
Figure 1 schematically illustrates a single breath induction
anesthesia apparatus according to a preferred embodiment of the invention;
~o Figure 2 is a partial top view of the apparatus illustrated in Fig.
1, showing the valve with the valve member thereof in a first position;
Figure 3 is another partial top view of the apparatus illustrated
in Fig. 1, showing the valve with the valve member thereof in a second
15 position;
Figure 4 is a partial side view of a single breath induction
anesthesia apparatus according to another preferred embodiment of the
invention, showing the valve with the valve member thereof in a first
zo position;
Figure 5 is a view similar to Fig. 3, but showing the valve with
the valve member thereof in a second position;
z5 Figure 6 is an exploded perspective view of the valve
illustrated in Fig. 4;
Figure 7 is an exploded perspective view of the valve
illustrated in Fig. 5 and shown with a safety cap; and
Figure 8 is a perspective view of the valve illustrated in Fig. 7,
showing the safety cap installed on the valve member.
Referring first to Fig. 1, there is illustrated a single breath
induction anesthesia apparatus which is generally designated by reference
CA 02288465 1999-11-04
-6-
numeral 10 and seen to comprise a gas delivery system 12 for delivering at
least one gas to a patient (not shown), an oxygen supply system 14, an
oxygen/anesthesia gas supply system 16 and a valve 18 for providing
selective gas flow communication between the oxygen supply system 14 and
5 the gas delivery system 12 or between the oxygen/anesthesia gas supply
system 16 and the gas delivery system 12. The gas delivery system 12
comprises a connector tube 20 defining an elbow and a face mask 22
connected thereto. The oxygen supply system 14 comprises an oxygen
source 24 and an oxygen bag 26 defining an oxygen reservoir. The
~o oxygen/anesthesia gas supply system 16, on the other hand, includes an
oxygen/anesthesia gas source circuit 28 and a breathing circuit 30 in gas
flow communication with one another.
The oxygen/anesthesia gas source circuit 28 comprises an
oxygen source 32 for supplying oxygen which flows through line 34
provided with a valve 36 and a flow-meter (not shown), a nitrous oxide
source 38 for supplying nitrous oxide which flows through line 40 provided
with a valve 42 and a flow-meter (not shown), lines 34 and 40 merging into
line 44, and a vaporizer 46 which is connected to line 44 and mixes the
zo oxygen and nitrous oxide with an anesthesia gas such as sevoflurane at a
preset optimum ratio sufficient to induce anesthesia of the patient with a
single breath. The nitrous oxide is another anesthesia gas which increases
the anesthesia effect of sevoflurane. The vaporizer is controlled so as to
provide a mixture containing oxygen, nitrous oxide and sevoflurane in
z5 which the sevoflurane is present in a concentration of about 8 vol. %. The
breathing circuit 30 which is in gas flow communication with the
oxygen/anesthesia gas source circuit 28 via line 48 comprises a Y-shaped
conduit 50 and a carbon dioxide absorber 52 connected thereto, the Y-
shaped conduit 50 comprising three conduit sections 54, 56 and 58. The
3o conduit sections 56 and 58 are provided with one-way valves (not shown) so
as to direct the flow of gases exhaled by the patient through expiratory
conduit section 56 along the direction indicated by arrow 60 and through
inspiratory conduit section 58 along the direction indicated by arrow 62.
Thus, when the valve 18 is operated to establish gas flow communication
35 between the oxygen/anesthesia gas supply system 16 and the gas delivery
CA 02288465 1999-11-04
_7_
system 12, gases inhaled and exhaled by the patient pass through the gas
delivery system 12 and the valve 18 and circulate through the breathing
circuit 30. The carbon dioxide absorber 52 absorbs carbon dioxide from the
gases exhaled by the patient, thereby allowing the oxygen/anesthesia gas
s mixture to be returned to the patient with less carbon dioxide.
As shown in Figs. 2 and 3, the valve 18 is a manually operated
two-way valve comprising a generally T-shaped valve body 64 having three
tubular branches 66, 68 and 70 with ports 72, 74 and 76 defined at the
~o respective proximal ends of the tubular branches 66, 68 and 70,
respectively,
and a valve member 78 arranged within the valve body 64 at the intersection
of the tubular branches 66, 68 and 70. The valve member 78 has a T-shaped
gas passage 80 formed therein and is movable between a first position
shown in Fig. 2, whereat the port 72 is in gas flow communication with the
15 port 76 and the port 74 is closed, and a second position shown in Fig. 3,
whereat the port 72 is closed and the port 74 is in gas flow communication
with the port 76. A handle 82 is provided for manually moving the valve
member 78 between these two positions. The valve body 64 has a cylindrical
portion 84 provided with an arcuate cut-out 86 defining at the longitudinal
Zo ends thereof two abutment surfaces 88 (shown in Fig. 3) and 90 (shown in
Fig. 2). The valve member 78, on the other hand, is provided with an arcuate
stop member 92 extending into the cut-out 86 and having two abutment
surfaces 94 (shown in Fig. 3) and 96 (shown in Fig. 2). The abutment
surfaces 88 and 94 cooperate with one another to arrest the movement of the
is valve member 78 at the first position, whereas the abutment surfaces 90 and
96 cooperate with one another to arrest the movement of the valve member
78 at the second position.
The tubular branch 66 has a gas inlet 98 connected by means
30 of a conduit 100 to the oxygen source 24 shown in Fig. 1, for providing gas
flow communication between the port 72 and the oxygen source 24. The
tubular branch 66 is also connected at its distal end to the oxygen reservoir
bag 26 for providing gas flow communication between the port 72 and the
oxygen reservoir bag 26. The tubular branch 66 is also provided with a gas
35 outlet 102 having a gas vent orifice 104 for venting excess oxygen, or
CA 02288465 1999-11-04
_g_
venting gases exhaled by the patient when the valve member 78 is in the
first position.
The tubular branch 68 is connected to the conduit section 54 of
s the Y-shaped conduit 50 for providing gas flow communication between the
port 74 and the oxygen/anesthesia gas supply system 16. Such a tubular
branch is provided with a gas outlet 106 having a gas discharge orifice 108
in gas flow communication with the port 74. The gas outlet 106 is connected
by means of a conduit 110 to a gas analyzer 112 (shown in Fig. 1) for
~o providing gas flow communication between the port 74 and the gas analyzer
112 to permit gas analysis of the oxygen/anesthesia gas mixture.
The tubular branch 70 is connected to the tube 20 for
providing gas flow communication between the port 76 and the gas delivery
~ s system 12.
The tubular branches 66, 68 and 70 each have a circular cross-
section with inner and outer diameters selected so that the tubular branch 66
can be fitted to any standard oxygen reservoir bag 26, the tubular branch 68
zo to any standard breathing circuit 30 and the tubular branch 70 to any
standard gas delivery system 12.
In operation, the face mask 22 is affixed to the patient with the
valve member 78 of the valve 18 being in the position shown in Fig. 2. In
z5 this position of the valve member 78, the port 72 is in gas flow
communication with the port 76 and the port 74 is closed. The oxygen
source 24 is opened to allow oxygen to flow through the conduit 100, the
gas inlet 98, the valve 18 along the direction indicated by arrow 114 and the
gas delivery system 12, the oxygen also filling the reservoir bag 26. This
3o permits a pre-oxygenation of the patient. The oxygen reservoir bag 26
enables the patient to inhale a larger volume of oxygen. At the same time,
valves 36 and 42 are opened to allow oxygen and nitrous oxide to flow via
lines 34,40,44 from the oxygen and nitrous oxide sources 32,38 to the
vaporizer 46 where the oxygen and nitrous oxide are mixed with the
35 sevoflurane contained in the vaporizer 46, the resulting gas mixture
flowing
CA 02288465 1999-11-04
-9-
from the vaporizer 46 to the breathing circuit 30 via line 48. When the
sevoflurane has reached the desired concentration indicated by the gas
analyzer 112, the valve member 78 of the valve 18 is moved to the position
shown in Fig. 3. In this position of the valve member 78, the port 72 is
s closed and the port 74 is in gas flow communication with the port 76. The
oxygen/anesthesia gas mixture thus flows from the oxygen/anesthesia gas
supply system 16 through the valve 18 along the direction indicated by
arrow 116 and the gas delivery system 12. This permits single breath
induction anesthesia of the patient. Excess oxygen is vented through the gas
~o vent orifice 104. Valves 36 and 42 can then be partially closed to reduce
the
flow of oxygen and nitrous oxide.
Instead of using sevoflurane, it is possible to use any other
type of anesthesia gas available on the market. The optimum concentration
~s of anesthesia gas sufficient to cause anesthesia of a patient with a single
breath may of course vary depending on the patient and the type of
anesthesia gas used. The use of nitrous oxide is also optional.
Although a breathing circuit 30 of recirculatory type has been
zo illustrated, it is possible to use other types of breathing circuits or
systems,
such as Mapleson systems, including Bain and Ayers T systems.
The apparatus illustrated in Figs. 4 and 5 is similar to the
apparatus shown in Figs. 1-3, with the exception that the apparatus of Figs. 4
zs and 5 comprises a valve 118 of different construction. As best shown in
Figs. 6 and 7, the valve 118 is a manually operated two-way valve
comprising a generally T-shaped valve body 120 having a hollow cylindrical
portion 122 and three tubular branches 124, 126 and 128 with ports 130, 132
and 134 defined at the respective proximal ends of the tubular branches 124,
30 126 and 128, and a valve member 136 arranged in the cylindrical portion
122 of the valve body 120. The tubular branches 124 and 126 extend along a
common axis 138, whereas the tubular branch 128 extend along a
longitudinal axis 140 which is disposed at right angle relative to the axis
138. The valve member 136 has a tubular portion 142 of cylindrical cross-
ss section defining an inner gas chamber 144 in gas flow communication with
CA 02288465 1999-11-04
-10-
the port 134, and a top portion 146 disposed over the tubular portion 142,
the top portion 146 being provided with a handle 148. The tubular portion
142 has an aperture 150 formed therein. The cyclindrical portion 122 of the
valve body 120 receives the tubular portion 142 of the valve member 136.
The valve member 136 is removably mounted in the
cylindrical portion 122 of the valve body 120 by means of a rib 152
extending about the outer periphery of the tubular portion 142 of the valve
member 136 and engaging a circumferential groove 154 formed in the inner
~o surface of the cylindrical portion 122. The valve member 136 is also
rotatably mounted in the latter for movement about a rotation axis coaxial
with the axis 140, between a first position shown in Figs. 4 and 6, whereat
the gas chamber 144 is in gas flow communication via the aperture 150 with
the port 130 and the port 132 is closed, and a second position shown in Figs.
5 and 7, whereat the gas chamber 144 is in gas flow communication via the
aperture 150 with the port 132 and the port 130 is closed. Thus, when the
valve member 136 is in the first position, the port 130 is in gas flow
communication with the port 134 and, when the valve member 136 is in the
second position, the port 132 is in gas flow communication with the port
zo 134. The handle 148 enables one to manually move the valve member 136
between these two positions.
In order to arrest the movement of the valve member 136 at
each of the above two positions, the cylindrical portion 122 of the valve
zs body 120 has at an end thereof a radially enlarged section 156 defining an
arcuate channel 158 with two abutment surfaces 160 and 162 (shown in Fig.
7) at longitudinal ends of the channel 158. The tubular portion 142 of the
valve member 136, on the other hand, is provided with a stop member 164
extending into the channel 158 and having two abutment surfaces 166 and
30 168. The abutment surfaces 160 and 166 cooperate with one another to
arrest the movement of the valve member 136 at the first position, whereas
the abutment surfaces 162 and 168 cooperate with one another to arrest the
movement of the valve member 136 at the second position. The section 156
is provided with two small, inwardly extending projections 170 and 172
35 over which the stop member 164 passes when the valve member 136 is
CA 02288465 1999-11-04
- 11 -
moved to the first or second position so that the abutment surface 166 or 168
engages the abutment surface 160 or 172 in a snaping action.
The tubular branch 124 comprises a tubular section 124A
s which is fixed to the cylindrical portion 122 of the valve body 120 and a
tubular section 124B which is removably connected to the tubular section
124A by means of a bayonet-lock type mechanism. Such a mechanism
comprises a lock pin 174 extending outwardly from the tubular section 124A
at the distal end thereof and a L-shaped slot 176 formed in the tubular
~o section 124B at one end thereof and receiving the lock pin 174 in
releasable
locking engagement. The L-shaped slot 176 has a slot portion 178 extending
longitudinally of the tubular section 124B and a slot portion 180 extending
at right angle relative to the slot portion 178. When the tubular sections
124A and 124B are connected together, the lock pin 174 is disposed in the
slot portion 180 in the lock position shown in Fig. 8. The tubular section
124B is provided at the ends thereof with two collars 182 and 184 which are
integrally formed therewith, the collar 182 partially covering the slot
portion
178.
zo The tubular section 124B has a gas inlet 186 connected by
means of the conduit 100 to the oxygen source 24 shown in Fig. 1, for
providing gas flow communication between the port 130 and the oxygen
source 24. Since the slot portion 180 of the L-shaped slot 176 extends in a
direction opposite to the direction in which the gas outlet extends, the
weight
z5 of the gas outlet and conduit 100 biases the lock pin 174 in the slot
portion
180 to the lock position shown in Fig. 8. The tubular section 124B is also
connected at its distal end to an oxygen reservoir bag 26' for providing gas
flow communication between the port 130 and the oxygen reservoir bag 26'.
The bag 26' which also serves as an oxygen breathing bag has a tubular
3o portion 188 provided with inner and outer sleeves 190 and 192 made of a
resilient material such as rubber. The sleeve 190 is disposed about the collar
184 in gas-tight engagement therewith. The tubular section 124B is provided
with a gas outlet 194 having a gas vent orifice 196 (shown in Figs. 6-8) for
venting excess oxygen, or venting gases exhaled by the patient when the
35 valve member 136 is in the first position.
CA 02288465 1999-11-04
- 12-
The tubular branch 126 is connected to the conduit section 54'
of a Y-shaped conduit 50' which is similar to the Y-shaped conduit 50
shown in Fig. l, for providing gas flow communication between the port
s 132 and the oxygen/anesthesia gas supply system 16 (shown in Fig. 1 ). The
conduit sections 56' and 58' of the Y-shaped conduit 50' are connected to the
carbon dioxide absorber 52. As in the case of conduit sections 56 and 58, the
conduit sections 56' and 58' are provided with one-way valves (not shown)
so as to direct the flow of gases exhaled by the patient through expiratory
~o conduit section 56' along the direction indicated by the arrow 60 (shown in
Fig. 1) and through inspiratory conduit section 58' along the direction
indicated by the arrow 62 (also shown in Fig. 1). The tubular branch 126 is
provided with a gas outlet 194 having a gas discharged orifice 196 in gas
flow communication with the port 132. The gas outlet 194 is connected by
means of a conduit 110' which is similar to the conduit 110 shown in Fig. 1
to the gas analyzer 112 (shown in Fig. 1), for providing gas flow
communication between the port 132 and the gas analyzer 112 to permit gas
analysis of the oxygen/anesthesia gas mixture. The conduit 110' extends
through a cap 198 which is removably connected to the gas outlet 194 by
zo means of a Luer-lock type coupling system 200.
The tubular branch 128 is connected directly to a face mask
22' for providing gas flow communication between the port 134 and the face
mask 22'. The mask 22' has a frusto-conical portion 202 provided with a
z5 cushioned flange 204.
The apparatus shown in Figs. 4 and 5 is operated in essentially
the same manner as the apparatus shown in Fig. 1. During pre-oxygenation
of the patient, the valve member 136 of the valve 118 is in the position
3o shown in Figs. 4 and 6. In this position of the valve member 136, the port
130 is in gas flow communication with the port 134 and the port 132 is
closed. Thus, oxygen flows from the oxygen source (shown in Fig. 1)
through the conduit 100, the gas inlet 186, the valve 118 along the direction
indicated by arrow 206 and the face mask 22', the oxygen also filling the
35 reservoir bag 26'. After pre-oxygenation has been effected, the valve
CA 02288465 1999-11-04
-13-
member 136 of the valve 118 is moved to the position shown in Figs. 5 and
7, and the tubular section 124B is disconneted from the tubular section 124A
and removed. In this position of the valve member 136, the port 130 is
closed and the port 132 is in gas flow communication with the port 134.
s Thus, the oxygen/anesthesia gas mixture flows from the oxygen/anesthesia
gas supply system 16 (shown in Fig. 1) through the valve 118 along the
direction indicated by arrow 208 and the face mask 22', causing single
breath induction anesthesia of the patient. The handle 148 is in the form of
an arrow indicating the direction of gas flow. Since during movement of the
~o valve member 136 from the position shown in Figs. 4 and 6 to the position
shown in Figs. 5 and 7, the valve member 136 moves about a rotation axis
which is coaxial with the longitudinal axis 140 of the tubular branch 128, the
pressure exerted on the valve member 136 to rotate same contributes to
providing a gas-tight seal between the cushioned flange 204 of the mask 22'
and the patient's face.
In order to releasably lock the valve member 136 in the
position shown in Figs. 5 and 7, after a ventilation and endotracheal
intubation has been performed, use is made of a safety cap 210 shown in
zo Figs. 7 and 8. The safety cap 210 comprises a dome-shaped skirt 212, a
hollow handle 214 extending outwardly from the skirt 212 and an arcuate
locking lip 216 depending from the skirt 212. The safety cap 210 is adapted
to removably fit over the top portion 146 and handle 148 of the valve
member 136 with the locking lip 216 extending into the channel 158 to
z5 prevent displacement of the stop member 164 when the valve member 136 is
in the position shown in Figs. 5 and 7. Fig. 8 shows the safety cap 210
installed over the valve member 136 and releasably locking same. In order
to prevent the locking lip 216 from having access to the channel 158 when
the valve member is in the position shown in Figs. 4 and 6, the valve
3o member 136 is provided with an arcuate flange 218 extending radially
outwardly from the tubular portion 142 of the valve member 136 and
disposed adjacent the top portion 146 thereof. The flange 218 extends over
the channel 158 when the valve member is in the position shown in Figs. 4
and 6 and thus acts as a shield preventing the locking lip 216 from being
35 inserted into the channel 15 8.