Note: Descriptions are shown in the official language in which they were submitted.
CA 02422219 2003-03-12
WO 02/25468 PCT/USO1/29303
TITLE OF THE INVENTION
Transfer of Organs from Donor to Recipient Using an On-Line Communication
System
FIELD OF INVENTION
This invention relates to a network based system for selecting, controlling,
and
dispersing such medical items as organs and tissues from donor to recipient.
BACKGROUND OF THE INVENTION
It is believed that the transfer of organs from donor to recipient is an
increasingly
extraordinarily important means of treating and, in many cases, saving the
lives of
individuals.
The current provision of organs from a donor to a recipient may provide a very
complicated, time consuming and inefficient process. At one end of the process
is the
organ donor; at the other end is the recipient. Between these two, information
may need
to be generated and collected in accessible means in numerous individual
steps. The
information may be critical to protect the organ and recipient, including
assuring that the
organ reaches a recipient for successfully transplanting.
The process may be as follows: The patient/donor is admitted to a hospital,
where he/she is examined by a physician. The physician determines if the donor
is
appropriate by making a judgment according to the donor's age, health history,
and other
factors. Consent to harvest the organ may be obtained from the guardian or,
where
permitted by law, from the hospital administrator. Once brain death has been
declared
by the attending physician, the patient may be prepared for the removal of the
organ to
be donated.
If the donor's condition makes his/her organs a candidate for transplant, the
attending physician may notify a donor network, an individual, an organ
procurement
agency (an "OPA"), or an organ procurement organization (an "0P0") -- which is
generally referred to herein as an OPA. Once the information has been
reduced.to
writing on the appropriate paper form of. numerous pages, it may be sent from
the
physician by a facsimile machine to the OPA. Much time may pass from form
preparation to transmittal.
-1-
CA 02422219 2003-03-12
WO 02/25468 PCT/USO1/29303
The OPA may use the received information to make a match between the organ
to be donated and the potential recipient. Once a match on the OPA's list is
made, the
OPA may need to contact the recipient's physician, which further delays the
system.
The physician may or may not be immediately available and, if available, may
not be in
a location to receive and/or review the information. Further, it may be
necessary that the
OPA be able to ascertain that it is, in fact, making contact with the
recipient's attending
physician so that the decision to accept or reject the donated organ is
appropriately and
authentically made.
When the recipient's physician has been contacted, the recipient may be
contacted and requested to come to the recipient's hospital to be prepared to
receive the
donated organ. At the same time, the donor patient, in the operating room, may
be
opened to remove the organ. The organ may be examined to provide information
necessary to determine if the selected organ is an appropriate candidate for
harvesting.
This information, which is well known in the art and may include matching of
the age
and physical size of the donor's organ with the recipient's organ
requirements, as well as
biochemistry, immunology, blood type, pathology, and the like, may be placed
upon a
written form. The organ may be removed and studied again. Additional data may
be
taken and placed upon a written form. The organ may be flushed and the
examination
may continue and may be recorded.
When the organ removal is finished, the now-deceased donor may be prepared
for removal from the operating room. Once the patient is removed, the
physician may
leave the operating room and send by facsimile the gathered information to the
OPA. It
is believed that this exercise presents yet another disadvantage to the
present system. No
communication may be made of the information by the donor's physician to the
recipient's physician during the period of time of the removal of the organ.
If, at the end of this procedure, the necessary information has been
transmitted to
the OPA, it may be determined by the recipient's physician that there is no
match. At
this point, the proposed recipient, who has now been in the hospital for
several hours (as
much as 3 to ~ hours), must now be advised that the operation cannot take
place. The
OPA may now search for a new recipient.
After the donation organ is removed, it may be packaged for transportation to
the
recipient's hospital. Exact records may be kept of the organ, its condition,
and how it
-2-
CA 02422219 2003-03-12
WO 02/25468 PCT/USO1/29303
was packed. These records may then be distributed to the OPA and the
recipient's
physician. The organ, as packaged, may be tracked so that it may be sent first
to the
proper OPA and then on to the proper recipient.
Before the organ reaches the proper recipient, however, the organ may go to a
holding area maintained by the OPA. Again, the organ and its packaging may be
checked and additional recorded information may be sent to the recipient's
physician.
The organ may also be received at the recipient's hospital, where more
information may
need to be gathered to determine if this organ should be transplanted. At this
stage, the
recipient may be advised that the organ is not acceptable, the OPA would be
notified and
another match would need to be found.
It is believed that the recipient's physician is handicapped not only by the
inefficiencies of the system, but also by the lack of immediate knowledge
necessary to
make a determination. The end result may be damaged or unusable organs, lost
time,
inconvenience and unneeded stress upon recipient patients, thereby decreasing
the
success of the medical procedure. It is believed that the process of
harvesting organs
from donors and getting them to recipients on a timely basis is, however, not
a simple or
straightforward procedure. Recipients may be identified and may be assigned
points so
that an order of selection based upon such concerns as the age of the
recipient, his/her
health, the type of organ desired, and the like may be determined. A registry
of such
information may be maintained. The selection process may be under the
supervision of
the recipient's physician. The donor's organs may need to be identified in
every aspect
(e.g., the age of the donor, the condition of the organ and the like). When
the organ is
available, information about it may be transmitted to the recipient's
physician for
evaluation. Procedures may be in place for determining if the person contacted
for
approval for receipt of the organ by the recipient is the recipient's
physician. If the organ
is refused, the next eligible recipient may be identified and the process of
approval and
transmittal of the organ begun again.
STJMMARY OF THE INVENTION
It is an object of this invention to provide a novel means of collecting and
distributing data concerning organ transplants. It is another object of this
invention to
provide real time data about the condition of an organ and to transmit the
real time
-3-
CA 02422219 2003-03-12
WO 02/25468 PCT/USO1/29303
information from the organ to a recipient's physician and an OPA. It is yet
another
object of this invention to provide access codes so that the OPA may have
access to the
information and the OPA may provide a more restrictive access code to a
physician
qualified to receive the information.
In accordance with this invention, there is provided a method for gathering
and
transmitting data of organs and tissues for use of the data, for example, in
the harvesting
and transferring of the organ from a donor to a recipient. The method includes
providing
on-line, real time communications means between the location of the organ and
at least
one receiver of the data. The method also includes monitoring the status and
condition
of the organs and tissues from removal from the donor until transplanted into
the
recipient. The method further includes inputting the data into the
communication means
as the data becomes available, and transmitting the data to the receiver.
There is also provided a system for gathering and transmitting data of organs
and
tissues for use in harvesting and transferring the organs and tissues from a
donor to a
recipient. The system includes a database that receives and stores data,
including a status
and condition of at least one of an organ and tissue and a processor that
communicates
between a location of the at least one of an organ and tissue and at least one
receiver and
transmits the data to the at least one receiver.
BRIEF DESCRIPTION OF THE DRAWING
In the drawings:
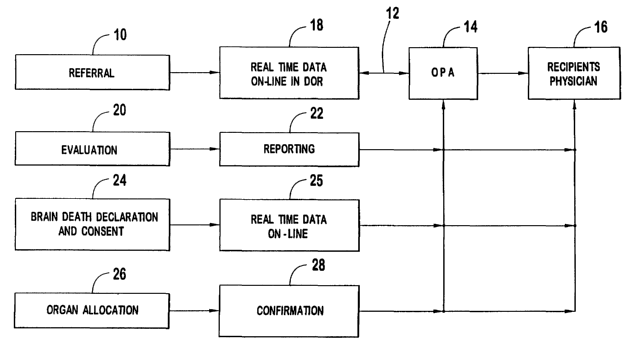
FIG. 1 is an overall flow diagram of the invention;
FIGS. 2 and 3 are detailed flow of the process of removing and placing an
organ
in accordance with invention; and
FIGS. 4 through 6 are exemplars of input forms which may be used in the
performance of the invention.
DESCRIPTION OF THE PREFERRED EMBODIMENTS
There is provided, in accordance with this invention, a unified system for
providing information and effecting the ongoing transfer of data of organs or
tissues
from a donor to a recipient. While the description that follows is directed to
organs, it
should be understood that this invention pertains to all body parts that might
be
-4-
CA 02422219 2003-03-12
WO 02/25468 PCT/USO1/29303
transplanted from a donor to a recipient. First and foremost, there are
provided three
levels of access to the system. The highest access, which is the Administrator
Level or
Level 1, permits entry of data, reading and editing of data, creation and
cancellation of
access codes, addition and deletion of accounts, review of user logs of the
system, and
programming changes in the system. Donor Organization Level (OPA) or Level 2
permits the providing of information to the recipient's physician and is able
to read and
edit all data concerning the organ. Recipient Physician Level or Level 3 is a
read-only
level in which the data can be received and evaluated, but no changes or
additions may
be made to the data.
The Administrator provides Level 2 and Level 3 access codes to the OPA, which
can cancel the codes or provide the codes to the recipient physician. These
access codes
enable only authorized individuals to gain access to the system. The OPA
administrates
Level 3 access codes to recipient physicians.
FIG. 1 shows the system employing the Internet, microwave communication,
satellite communication or the like. The donor's physician makes a referral 10
to the
OPA 14. The OPA 14 then contacts the recipient's physician 16 by any available
means.
The referral 10 is input into a terminal in the donor's operating room ("DOR")
18 and
instantly transmitted on line 12 through to the OPA 14. The OPA 14, who can
only
access the system at Level 2 contacts and activates the Level 3 access codes
of the
recipient's physician 16. The OPA 14 also communicates with the staff of the
DOR 18.
The organ evaluation 20 continues in the DOR 18. Data relating to the organ,
especially the vital signs of the organ, including its condition, chemistry,
and the like, are
taken in a manner well known in the art. These data are directly input into an
I/O device,
such as a personal computer, which may be directly connected to the Internet
or similar
means of communication. The forms, examples of which may be seen in FIGS 4-6
(FIGS 4A and 4B represent one form), which in the past, were on paper, are now
immediately entered into a database. Once the data are entered, they may be
instantly
viewed in a report 22 by the OPA 14 and the receiver of the data, typically
the recipient's
physician 16 or representative of the recipient's physician, providing they
have logged
on with their access codes. In some cases, there may be multiple receivers of
data, e.g.,
prior to there being a final selection of the transplant recipient. Upon the
declaration of
brain death and with the consent 24 in place, the real time data 25 may be
simultaneously
-5-
CA 02422219 2003-03-12
WO 02/25468 PCT/USO1/29303
transferred to the OPA 14 and physician 16 via the Internet or any other real
time
communication system. The OPA 14 confirms the organ allocation 26 and sends
the
confirmation 28 to the physician 16.
The information that is provided is now enlarged by use of on-line direct
S communication. Thus, the data entered into the form is instantly stored in a
database, as
is well known in the art. Further, throughout the processing of the organ,
from the DOR
18 through the packaging and transplantation, the organ, and its status, i.e.,
its chemistry,
its physical condition, and the like, can be continuously monitored and the
data
accumulated can be directly input into the database and made available to
interested
parties on a real time basis. Thus, additional and significant information is
provided that
has not previously been available. This may also include jpg pictures, or
images, of the
organs made immediately available to the recipient's physician 16 and the OPA
14. The
vital signs of the organ can be continuously monitored by means of mpeg
imaging.
Thus, the OPA 14 and physician 16 get instantaneous information not available
in any
form at present. This information may be stored in an accessible database for
both the
OPA 14 and any physician or investigative or research organization for future
study and
research.
This increase of significant information gives the recipient's physician 16
better
and more timely, thorough, and accurate data upon which to determine if a
harvested
organ is suitable for a predetermined recipient. The recipient need not be
bothered until
the last possible moment when the recipient's physician 16 is reasonably
certain that the
organ is a match for his patient. The process in the DOR 18 is instantly
monitored by the
OPA 14 and the recipient's physician 16 at all times.
A more detailed description (FIGS. 2 and 3) describes the steps of the organ
harvesting and transplant and transfer of data from the DOR to the OPA and
recipient's
physician on a real time basis. In the DOR, a link is established through the
on-line
communication means in step 30, providing real time data that may be
customized in
step 32 to fit the type of organ (or tissue or other body part) and potential
recipient. An
incision is made in the donor in step 34 and the donor's physician and his/her
support
staff view the potential organ in step 36. Real time imaging of the organ may
be
provided in step 38 by, for example, a video camera. Data about the organ may
be
instantly recorded on-line in step 40, as well as entered into a database
maintained by the
-6-
CA 02422219 2003-03-12
WO 02/25468 PCT/USO1/29303
administrator and/or the OPA, and real time reporting of the organ's condition
is made to
the recipient's physician in step 41. The next steps are those usually
provided in organ
removal, including dissection in step 42 and flushing the organ in step 44.
The organ is
removed in step 46. In step 48, the staff in the DOR record anatomical
information,
including statistical data, which is instantly made available in step 50
through the PC or
similar communication means.
As shown in Fig. 3, the organ is then moved to a back table flush in step 52
and
then packed in step 54 and transported to a main organ transfer center or a
perfusion
laboratory in step 56, as is well known in the art. At the transfer center or
perfusion
laboratory, sensors may be applied to the organ and additional clinical
analysis may be
made in step 58, instantly stored in the database, and transmitted to the
recipient's
physician for evaluation.
As is well known in the art, the organ is prepared for a perfusion apparatus
in step
60, and then placed on an organ perfusion pump in step 62. It is contemplated
within the
scope of this invention that the recipient's physician and/or the OPA
personnel may use
their terminals to direct cameras and sensors to view the organ and its vital
signs in step
64. The means for controlling such sensors and cameras is well known in the
art.
The organ is then described yet again and analyzed in step 66 and placed on-
line.
Further remote viewing of data and status of the organ and the comparison with
the
historical data gathered in the DOR may then be available to the OPA and the
recipient's
physician in step 68. The OPA or perfusion lab may then receive information
for the
placement of the organ in step 70. This information may be posted and made
available
to the OPA and the recipient's physician, as well as other physicians who may
be caring
for alternate recipients.
The organ is then delivered to the transplantation center in step 72 and
processed.
Once more, for the safety and care of the recipient, the condition of the
organ may be
monitored in step 74 and the resulting data may be placed on-line and/or
stored in the
database. In this way, the organ is not only continuously monitored, but the
recipient is
not involved in the process until the receiving physician is reasonably
certain that a
match has been made. If no match has been made, the next recipient will be
selected and
the stored data will be provided instantly to that recipient's physician. In
this process,
the Level 3 access code would then be removed from the first recipient's
physician and a
_7_
CA 02422219 2003-03-12
WO 02/25468 PCT/USO1/29303
riew code would be given to a new recipient's physician. The three levels of
access
codes protect the system from being tampered and restrict access to those with
a need to
know and a need to edit.
Another advantage to this system is that all data concerning organ donations
are
easily collected in a rational database for statistical comparisons.
Statistical data can be
accumulated and compared by means of graphs and similar means. The collected
information may then be used for such purposes as establishing and determining
criteria
for a potentially successful or unsuccessful organ donation.
Further, providing the receiving physician and the OPA with access to the
information on a real-time basis enables the individual reviewing the data to
remotely
manipulate, monitor and analyze medical information. For example, if a digital
camera
is provided to view the organ, it is within the contemplation of this
invention that the
recipient's physician may command the camera to obtain different views of the
organ
and/or selectively collect on-line and/or historical data concerning the
selected donated
organ. The recipient's physician may also compare that data instantly with
historical
data about such organs to better gauge and evaluate the probabilities of a
successful
transplant for a particular recipient.
Contacting the recipient's physician is also simplified and made more
efficient by
this system. The physician is provided with his/her Level 3 access code and
can be
notified by e-mail or other means of the availability of an organ. The access
code
assures that only the authorized individual (or a designee of that individual)
can gain
access to the information.
The system may also be used by a medical examiner, forensic scientist, or
similar
occupation to determine if an organ has not been subject to "foul-play," where
an
autopsy would be required. The medical examiner or forensic scientist would be
able to
view images of the organ and review the biopsy findings and histology to make
a
determination. If an autopsy is not required, the organ would be available for
transplant.
It is to be understood that the although there is shown the preferred
embodiments
of the invention, that various modifications may be made in the details
thereof without
departing from the spirit as comprehended by the following claims.
_g_