Note: Descriptions are shown in the official language in which they were submitted.
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
SENSOR AND METHOD FOR DETECTING A PATIENT'S
MOVEMENT VIA POSITION AND OCCLUSION
FIELD OF THE INVENTION
This invention relates generally to monitoring systems and more particularly
concerns devices and systems used to monitor seated or lying patients in homes
or in
medical environments such as hospitals, institutions, and other care-giving
environments so as to reduce the risk that such patients will develop
decubitus ulcers.
BACKGROUND OF THE INVENTION
It is well known that patients who are confined to a bed or chair for extended
periods of time are at risk of developing decubitus ulcers, i.e., pressure
sores, or bed
sores as they are more commonly known. These ulcers are often seen to develop
within soft tissue that is compressed between a bed or chair -surface and a
patient's
weight-bearing bony prominences, the compressed tissue being at least
partially of
deprived of oxygenated blood flow. A continued lack of blood flow, and
resultant
lack of oxygen, can result in cell death, which may be evidenced in the form
of
pressure sores. Pressure sores do not develop immediately, but rather form
over time,
with the development speed depending on a number of factors including the
firmness
and friction of the supporting surface against the patient's skin, the
patient/ambient
temperature, the amount of moisture in contact with the skin, and the health
and
susceptibility of the skin due to age, illness, and/or nutrition.
One venerable and generally accepted means of reducing the risk of decubitus
ulcer development in bedfast patients is to turn them regularly, usually at
approximately two hour intervals. For example, a patient in a back rest
position might
be periodically rolled to one side or the other, such motion helping to
maintain blood
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
flow to soft tissue that is under compression. Similar strategies are employed
for
patients that are confined to a chair for long periods of time. Obviously, an
assisted-
movement strategy relies largely on the vigilance of the (often harried)
attending staff
to insure that the patient is properly relocated. Further, it is far too easy
for the busy
caregiver to let the time for turning the patient slip by in the press of
other daily
emergencies. To the extent that the caregiver is too busy or forgets to
perform this
service, this method can fail to achieve its purpose. Further, this sort of
strategy can
be counterproductive for use with the patient that has some capacity for self-
movement when, for example, the patient may have turned himself just before
the
caregiver arrived to manually turn him, in which case the caregiver will
likely place
the patient back in the position from which he recently moved, thus
inadvertently
exacerbating the problem. Further, after being rolled to a new position the
patient
might return to the original "comfortable" position after the caregiver leaves
which
would obviously negate the effects of the reposition.
The process of moving a patient to another position is admittedly disruptive
to
the patient and this is especially true at night, since the patient - if he or
she were
sleeping - will be awakened for the purpose of relocation. The typical two-
hour
movement interval must be observed around the clock if the method is to be
effective,
so it is necessary to disturb the patient - who might be sleeping soundly at
the time
- to make the required adjustment in position. Further, this adjustment might
not
have even been necessary, or even counter indicated, if the patient had
recently
moved of his or her own volition. Thus, in many situations it would be
advantageous
for the caregiver to know if and when the patient last moved his or herself.
Then, if
the last movement were within a prescribed period of time, it might be
possible to
2
CA 02532600 2009-10-05
spare the patient an unnecessary interruption in his or her healing sleep. The
caregiver would then relocate the sleeping patient, only if that relocation
were
actually required. Further, knowing which patients do not need to be moved
could
result in a substantial savings in labor costs, as the time that would
otherwise be
devoted to moving the patient that did not actually need to be moved could be
productively applied elsewhere. That being said, as useful as this sort of
information
might be to the health care provider, however, the present state-of-the-art in
patient
management does not provide this sort information.
Generally speaking, there are two broad approaches to dealing with decubitus
ulcers: mechanical and medicinal. The medical approach is concerned with the
development of medicinal compounds and methods for treating the ulcer after it
occurs. This approach is obviously quite useful but ultimately it is reactive,
rather
than proactive, because it attempts to minimize the damage occasioned by the
ulcer
after it has formed.
On the other hand, the mechanical approach typically utilizes a specialized
mattress, pad, or other arrangement, which is designed to lessen the weight-
pressure
that is brought to bear on the patient's bony prominences. These devices might
be
either static (e.g., foam, air, or water mattresses) or dynamic (e.g.,
compartmentally
inflatable mattresses that dynamically shift the locus of support pressure
under the
patient over time. Examples of inventions in the prior art that are generally
concerned
with this subject matter include U.S. Letters Patent 4,425,676, 5,926,884, and
5,072,468. Generally speaking, a mechanical approach is to be preferred
because it seeks
to spare the patient the discomfort and risk associated with bed sores and
reduces the costs
3
CA 02532600 2009-10-05
associated with treating such, which costs can potentially accrue to the
facility under
some circumstances.
One enhanced variant of the mechanical approach utilizes a proactive strategy
that seeks to avoid tissue death by using a combination of automatic
monitoring of the
patient's movement together with notification of a caregiver if the patient's
movement
pattern does not meet or exceed some predetermined level. Upon receipt of such
notice, the caregiver will then manually turn the patient, as has been the
custom
heretofore. This approach, if properly implemented, has the potential to
dramatically
reduce the risk of pressure sores while keeping the cost of such preventative
measures
within the reach of small institutions and individual patients.
It is this last approach, electronic patient monitoring combined with
caregiver
intervention, which has been adopted by the instant inventors. As such,
general
information relating to mat-type sensors and electronic monitors for use in
patient
monitoring is relevant to the instant disclosure and may be found in U.S.
Letters
Patent Nos. 4,179,692, 4,295,133, 4,700,180, 5,600,108, 5,633,627, 5,640,145,
5,654,694, and 6,111,509 (the last of which concerns electronic monitors
generally).
Additional information may be found in U.S. Letters Patent Nos. 4,484,043,
4,565,910, 5,554,835, 5,623,760, 6,417,777 (sensor patents) and U.S. Letters
Patent
5,065,727 (holsters for electronic monitors). Further, U.S. Letters Patent
numbers
6,307,476 (discussing a sensing device which contains a validation circuit
incorporated
therein), U.S. patent number 6,544,200, (for automatically configured
electronic monitor
alarm parameters), and U.S. patent numbers 6,696,653 (for a binary switch and
a
4
CA 02532600 2009-10-05
method of its manufacture), and 6,864,795 (for a lighted splash guard).
Additionally, sensors other than mat-type pressure sensing switches may be
used in patient monitoring including, without limitation, temperature sensors,
patient
activity sensors, toilet seat sensors (see, e.g., U.S. Patent No. 5,945,914),
wetness
sensors (e.g., U.S. Patent No. 6,292,102), decubitus ulcer sensors (e.g., U.S.
Patent
6,646,556), etc. Thus, in the text that follows the terms "mat" or "patient
sensor" should
be interpreted in its broadest sense to apply to any sort of patient
monitoring switch or
device, whether the sensor is pressure sensitive or not.
Finally, pending U.S. Patent Serial Number 6,897,781, discusses how white
noise can be used in the context of decubitus ulcer prevention.
Heretofore, as is well known in the patient monitoring and, more particularly,
the decubitus ulcer prevention arts, there has been a need for an invention to
address
and solve the above-described problems. Accordingly, it should now be
recognized,
as was recognized by the present inventors, that there exists, and has existed
for some
time, a very real need for a system for monitoring patients that would address
and
solve the above-described problems.
Before proceeding to a description of the present invention, however, it
should
be noted and remembered that the description of the invention which follows,
together
with the accompanying drawings, should not be construed as limiting the
invention to
the examples (or preferred embodiments) shown and described. This is so
because
5
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
those skilled in the art to which the invention pertains will be able to
devise other
forms of this invention within the ambit of the appended claims.
SUMMARY OF THE INVENTION
In accordance with a first aspect of the instant invention, there is provided
a
patient sensor and electronic monitor combination that continuously monitors a
bedfast or chair bound patient to determine whether or not that patient's
amount of
movement is sufficient to, for example, eliminate the next scheduled turning
by the
caregiver.
In a first preferred arrangement of the instant invention, there is provided a
sensor for use in connection with an electronic patient monitor, wherein the
sensor
uses a resistive ladder with spaced-apart resistors as a means of determining
at least
approximately a location of the patient on the sensor as well as an
approximate length
of the sensor which is contacted by the patient. By continuously determining
both of
these quantities over time it is possible to track the patient's movement and
determine
to what extent the patient needs to be manually turned and/or the extent to
which a
next-scheduled turn can be skipped. In one preferred embodiment, the resistors
will
be linearly spaced apart within the patient sensor.
According to another preferred arrangement, a plurality of resistive ladders
arranged in a parallel configuration, one above the other, will be used to
determine the
position and contact region of a patient with these multiple sensors and,
additionally,
will be used to calculate some relative value of the shear which is being
experienced
by the patient as his or her body slides down in the bed. Preferably, the
resistive
elements will be linearly spaced apart.
6
CA 02532600 2009-10-05
In accordance with one aspect of the present invention, there is provided a
patient
sensor for use in monitoring a patient who is at risk of developing decubitus
ulcers, the
patient sensor having at least a first end and a second end, comprising: (a) a
nonconductive
upper member, the upper member having an outer surface and an inner surface,
wherein
at least a portion of the upper member inner surface is electrically
conductive; (b) a
nonconductive lower member, the lower member having an inner surface and an
outer
surface, the lower member inner surface being positionable to be proximate to
the upper
member inner surface, wherein at least a portion of the lower member inner
surface is
electrically conductive, the electrically conductive portion of the lower
member inner
surface containing at least two electrically isolated circuits thereon, (b I)
wherein a first
circuit of the at least two electrically isolated circuits contains at least a
plurality of spaced
apart resistive elements therein, and, (b2) wherein a second circuit of the at
least two
electrically isolated circuits, when taken in combination with the first
circuit, forms a
plurality of switches, each of the switches having at least one of the
resistive elements
associated therewith and each of the switches being located at a predetermined
distance
from the first end of the patient sensor; (c) a nonconductive central spacer
between the
upper member and the lower member, the central spacer electrically separating
at least a
portion of the upper member and the lower member inner surfaces, and, allowing
at least
a portion of the conductive portions of the upper member and the lower member
to come
into electrical contact when a patient is present on the patient sensor,
thereby electrically
engaging at least one of the plurality of switches and the resistive elements
associated
therewith; and, (d) an electrical line in electrical communication with the
conductive
portions of the upper and lower members, the electrical line having at least
three
electrically isolated conductors therein, wherein (dl) a first conductor of
the at least three
6a
CA 02532600 2009-10-05
conductors is in electrical communication with the first circuit, (d2) a
second conductor
of the at least three conductors is in electrical communication with the first
circuit, such
that by measuring the potential between the first and second conductors a
total resistance
in the first circuit may be determined, and (d3) a third conductor of the at
least three
conductors is in electrical communication with the second electrically
isolated circuit,
such that by measuring a total resistance between the first circuit and the
second circuit
a determination may be made of a location and extent of the at least one point
of contact.
In accordance with another aspect of the present invention, there is provided
a
patient sensor for use in monitoring a patient who is at risk of developing
decubitus ulcers,
the patient sensor having at least a length and a first end and a second end,
comprising:
(a) a nonconductive lower member, the lower member having an inner surface and
an
outer surface, wherein the lower member inner surface has at least one
resistive ladder
thereon, the at least one resistive ladder having a plurality of serially
connected spaced
apart resistive elements spanning at least a portion of the length of the
patient sensor, and,
wherein the nonconductive lower member inner surface has an electrically
isolated contact
circuit proximate to the resistive ladder; (b) a nonconductive upper member,
the upper
member having an outer surface and an inner surface, wherein at least a
portion of the
upper member inner surface is electrically conductive, (c) a nonconductive
central spacer
positionable to be between the upper member and the lower member, the central
spacer
separating the electrically conductive portions of the upper member and the
lower
member, and, allowing the electrically conductive portions of the upper member
and the
lower member to come into contact when pressure is applied to the patient
sensor, thereby
electrically shorting the resistive ladder and the contact circuit at a point
of contact when
the contact is made; and, (d) an electrical line in electrical communication
with the
6b
CA 02532600 2009-10-05
conductive portions of the upper and lower members, the electrical line having
at least
three electrically isolated conductors therein, wherein (dl) a first conductor
of the at least
three conductors is in electrical communication with the resistive ladder,
(d2) a second
conductor of the at least three conductors is in electrical communication with
the resistive
ladder such that by measuring the potential between the first and second
conductors a total
amount of resistance in the first conductor may be determined, and (d3) a
third conductor
of the at least three conductors is in electrical communication with the
contact circuit.
In accordance with a further aspect of the present invention, there is
provided a
patient sensor for use in monitoring a patient who is at risk of developing
decubitus ulcers,
wherein the sensor is configured to be positioned beneath the patient,
comprising: (a) a
nonconducting upper member, the upper member having a perimeter and an inner
surface;
(b) a nonconducting lower member, the lower member having a perimeter and an
inner
surface, and the lower member being sized to be at least approximately
commensurate
with the upper member, the upper and lower members being joined together along
their
perimeters, the upper and lower members taken together forming an interior of
the patient
sensor therebetween; (c) a nonconducting central spacer, positioned between
the upper and
lower members and separating at least a portion of upper member inner surface
from
contact with the lower member inner surface; (d) a first conductor within the
interior of
the patient sensor, the first conductor having a first end and a second end,
and the first
conductor comprising at least a plurality of serially interconnected resistive
elements; (e)
a plurality of spaced apart serially connected switches, wherein (el) each of
the switches
engages the first conductor at a predetermined location when activated, (e2)
at least a
portion of each of the switches is located on the upper member inner surface
and another
portion of each of the switches is located on the lower member inner surface,
and, (e3)
6c
CA 02532600 2009-10-05
each of the switches can be separately activated by the patient when the
sensor is
positioned underneath the patient, each switch being so activated only when it
is at least
approximately directly beneath the patient; and, (f) a second conductor in
electrical
communication with the serially connected switches, the second conductor
coming into
electrical communication with the first conductor if at least one of the
switches is activated
in response to a patient's presence on the sensor, whereby (f1) measuring an
electrical
property between the second conductor and the first end of the first conductor
provides a
value representative of an activated switch nearest the first end of the first
conductor, and,
(f2) measuring an electrical property between the second conductor and the
second end
of the first conductor provides a value representative of an activated switch
nearest the
second end of the first conductor.
In accordance with yet a further aspect of the present invention, there is
provided
a patient sensor for use in monitoring a patient who is at risk of developing
decubitus
ulcers, the sensor at least for providing a patient's position and an amount
of the sensor
occluded by the patient's presence thereon, the patient sensor being
positionable to be
placed beneath the patient, comprising: (a) a nonconductive upper member, the
upper
member having an outer surface and an inner surface, (b) a nonconductive lower
member,
the lower member having an inner surface and an outer surface, the lower
member inner
surface being positionable to be proximate to the upper member inner surface,
the upper
member and lower member together forming an interior of the sensor, wherein at
least a
portion of the lower member inner surface is electrically conductive, the
electrically
conductive portion of the lower member inner surface comprising at least a
plurality of
resistive elements connected in parallel by at least one conductor, the
plurality of resistive
elements and the at least one conductor comprising a resistive circuit; (c) a
plurality of
6d
CA 02532600 2009-10-05
spaced apart switches within the interior of the sensor, (c 1) wherein each of
the switches
is positioned at a predetermined location within the sensor, (c2) wherein at
least a portion
of each switch is on the upper member inner surface; (c3) wherein at least a
portion of the
switches engage a matching number of the resistive elements when the sensor is
positioned beneath the patient, and, (c4) wherein each of the plurality of
switches is
separately readable to determine which of the switches is engaged, thereby
providing
information related to the position of the patient and the amount of the
sensor occluded
by the patient; and, (c) a nonconductive central spacer between the upper
member and the
lower member, the central spacer electrically separating at least a portion of
the upper
member and the lower member inner surfaces when the sensor is not beneath the
patient,
and, allowing at least a portion of the conductive portions of the upper
member and the
lower member to come into electrical contact when a patient is present on the
patient
sensor, thereby electrically engaging at least one of the plurality of
switches and the
resistive elements associated therewith, and, (d) a plurality of electrical
lines in electrical
communication with the plurality of switches, wherein, (d 1) each of the
electrical lines is
electrically isolated from the other, (d2) each of the electrical lines is in
electrical
communication with a different one of the plurality of switches, and, (d2)
measuring an
electrical property between any of the electrical lines and the resistive
circuit provides a
signal indicative of whether the associated switch is engaged.
In accordance with an even further aspect of the present invention, there is
provided a patient sensor for use in monitoring a patient, the sensor at least
for providing
a patient's position and an amount ofthe sensor occluded by the patient's
presence thereon,
the patient sensor being positionable to be placed beneath the patient, the
patient sensor
having an interior, comprising: (a) a resistive ladder within the patient
sensor, the resistive
6e
CA 02532600 2009-10-05
ladder containing a plurality of resistive elements therein, each of the
resistive elements
having a nominal resistive value associated therewith; (b) a plurality of
switches, each of
the switches engaging one of the resistive elements when the switch is placed
beneath the
patient, each of the switches being located at a predetermined location within
the sensor
interior; and, (c) first, second, and third leads in communication with the
resistive ladder,
whereby, (c 1) the first and second leads taken together provide a signal at
least
representative of a distance of the patient from an end of the sensor, and,
(c2) the first and
third leads taken together provide a signal at least representative of an
amount of the
sensor occluded by the patient's presence thereon.
15
6f
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
The foregoing has outlined in broad terms the more important features of the
invention disclosed herein so that the detailed description that follows may
be more
clearly understood, and so that the contribution of the instant inventor to
the art may
be better appreciated. The instant invention is not to be limited in its
application to
the details of the construction and to the arrangements of the components set
forth in
the following description or illustrated in the drawings. Rather, the
invention is
capable of other embodiments and of being practiced and carried out in various
other
ways not specifically enumerated herein. Further, the disclosure that follows
is
intended to apply to all alternatives, modifications and equivalents as may be
included
within the spirit and scope of the invention as defined by the appended
claims.
Finally, it should be understood that the phraseology and terminology employed
herein are for the purpose of description and should not be regarded as
limiting,
unless the specification specifically so limits the invention.
While the instant invention will be described in connection with a preferred
embodiment, it will be understood that it is not intended to limit the
invention to that
embodiment. On the contrary, it is intended to cover all alternatives,
modifications
and equivalents as may be included within the spirit and scope of the
invention as
defined by the appended claims.
BRIEF DESCRIPTION OF THE DRAWINGS
Other objects and advantages of the invention will become apparent upon
reading the following detailed description and upon reference to the drawings
in
which:
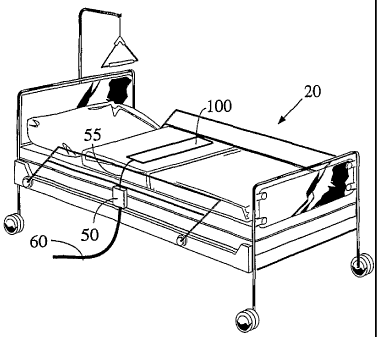
Figure 1 illustrates the general environment of the instant invention, wherein
an electronic patient monitor is connected to a bed mat.
7
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
Figure 2 illustrates the general environment of the instant invention, wherein
an electronic patient monitor is connected to a chair mat.
Figure 3 contains an illustration of the main features of a preferred
embodiment of the instant pressure sensitive mat.
Figure 4 is an electronic schematic of the preferred pressure sensitive mat of
Figure 3.
Figure 5 contains an illustration of a preferred monitor for use with the
instant
invention.
Figure 6 is a schematic diagram of a preferred microprocessor-based
electronic monitor for use with the instant inventive pressure sensitive mat.
Figure 7 illustrates another preferred embodiment of the instant invention,
wherein the resistive ladder is configured so as to provide both a lateral and
longitudinal patient position.
Figure 8 contains a schematic illustration of another preferred embodiment of
the instant invention, wherein the multiple resistive ladders are provided so
as to
provide both a lateral and longitudinal patient position.
Figure 9 contains a schematic illustration of another preferred embodiment of
the instant invention, wherein each resistive element is separately readable.
Figure 10 illustrates another preferred embodiment, wherein the number of
interconnect electrical conduits has been reduced by one.
Figure 11 contains a preferred electronic monitor embodiment, wherein no
microprocessor is utilized.
8
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
Figure 12 contains an optical switch embodiment suitable for use with the
instant invention, wherein a foam block or similar material is used as an
optical
attenuator.
Figure 13 contains another preferred optical switch embodiment wherein
misalignment of two optical fibers is used as an optical attenuator.
Figure 14 contains still another preferred optical switch embodiment which
utilizes a movable plate or similar structure to block passing between two
sections of
optical fiber, thereby attenuating the amount of light passing therebetween.
Figure 15 illustrates a preferred sensor embodiment, wherein optical switches
and attenuators are used instead of electrical resistors.
DETAILED DESCRIPTION OF THE INVENTION
According to a preferred aspect of the instant invention, there is provided an
electronic patient monitor for use with a patient sensor, wherein the attached
sensor is
at least suitable for determining the location of the patient in the bed or
chair through
the use of a resistive ladder.
GENERAL ENVIRONMENT OF THE INVENTION
Generally speaking, electronic patient monitors of the sort discussed herein
work by first sensing an initial status of a patient, and then generating a
signal when
that status changes (e.g., the patient changes position in the bed, the
patient fails to
change position in the bed, the patient leaves the bed, the sensor changes
from dry to
wet, the temperature of the sensor changes, etc.) or , in some cases, if the
initial
condition persists for too long a period of time (e.g., if the patient has not
moved
during a predetermined time interval). Turning now to Figure 1 wherein the
general
environment of one specific embodiment of the instant invention is
illustrated, in a
9
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
typical arrangement a pressure sensitive mat 100 sensor is placed on a bed 20
where it
will lie beneath a weight-bearing portion of the reclining patient's body,
usually the
buttocks and / or shoulders. Generally speaking, the mat 100 / electronic
monitor 50
combination works as follows. When a patient is placed atop the mat 100, the
patient's weight compresses it, thereby closing an internal electrical
circuit. This
circuit closure is sensed by the attached electronic patient monitor 50 and,
depending
on its design, this closure may signal the monitor 50 to begin monitoring the
patient
via the mat 100. Additionally, in some embodiments, the monitoring phase is
initiated by a manually engaged switch. Thereafter, when the patient's status
changes
(e.g., if weight is removed from the sensing mat 100, thereby breaking the
electrical
circuit, or if the patient changes position on the mat 100) this change is
sensed by the
attached electronic patient monitor 50 which responds to the changing
condition
according to its internal design and/or programming.
In some configurations, the changed circumstance of the patient will result in
a
signal or alarm being sent to notify a caregiver of the event. For example, if
the
patient has risen to his or her feet and left the bed, an electronic signal
will be sent to a
remote nurses / caregivers station via electronic communications line 60. In
other
arrangements, and more pertinent to the instant disclosure, if the patient's
circumstance does not change for some period of time (e.g., if the patient has
remained motionless within the bed or chair) an alarm will be sounded. In
still other
arrangements, an alarm might be sounded if, for example, the patient's skin
temperature rises, which can in some instances be a precursor to the formation
of a
decubitus ulcer. Note that additional electronic connections not pictured in
this figure
might include a monitor power cord to provide a source of AC power although,
as
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
generally pictured in this figure, the monitor 50 can certainly be configured
to be
either battery or AC powered. In other configurations, if the monitor 50 is
designed
to track the patient's position in the bed, a change in position would not
necessarily
result in an alarm being generated, but rather such a change might be recorded
by the
monitor 50 for later review and analysis by the staff or for purposes of
monitoring the
patient's movement history as is discussed at greater length hereinafter.
Similarly, if
the patient has not moved for some predetermined period of time, that
circumstance
could also generate an alarm. Those of ordinary skill in the art will
recognize that the
previous examples are just a few of the many variations of this general scheme
that
are possible.
In another common arrangement, and as is illustrated in Figure 2, a pressure
sensitive chair sensor 200 might be placed in the seat of a wheel chair or the
like for
purposes of monitoring a patient seated therein. As has been described
previously, a
typical configuration utilizes a pressure sensitive mat 200 that is connected
to an
electronic chair monitor 250 that is suspended from the chair 30. Because it
is
anticipated that the patient so monitored might choose to be at least somewhat
mobile,
the monitor 250 will usually be battery powered and will signal a patient
change event
(or, patient non-change event) via an internal speaker, rather than a
hardwired nurse-
call. Of course, those of ordinary skill in the art will understand that in
some
instances the monitor 250 can be configured to communicate wirelessly with the
nurses' station through RF, IR, ultrasonic or other communications technology.
PREFERRED EMBODIMENTS
In accordance with a first aspect of the instant invention and as is generally
shown in Figure 3A, there is provided a patient sensor 300 which is designed
to
11
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
determine at least an approximate longitudinal position of the patient on the
sensor
and, additionally, to determine an occluded length of the sensor.
In a first preferred arrangement, a mat-type sensor with a resistive (or
similar
component) ladder which is comprised of a plurality of resistive elements
arrayed in a
spaced apart configuration is used to determinate at least a longitudinal
position of the
patient on the sensor. As is illustrated in Figure 3B, the preferred mat 300
is
comprised of three layers: upper 350 and lower 360 non-conductive layers, and
inner
spacer 355 which is positioned between and separates the upper 350 and lower
360
layers.
In a preferred arrangement, the pressure sensitive mat of the instant
invention
is generally rectangular in shape and provides external electrical
connectivity by way
of electrical line 305 and connector 308. Preferably the connector 308 will
take the
form of an RJ-11 or similar connector. As is best illustrated in Figure 3B,
the
preferred sensor 300 is comprised of a "sandwich" of three layers: two outer
nonconductive layers 350 and 360, and, preferably, an inner nonconductive
central
spacer 355. In the preferred embodiment, each of these layers is made of a
flexible
material such as polyester. Additionally, it has been contemplated by the
inventors
that polyethylene layers might be bonded to each of these of the components
350,
355, and 360 to make it possible to fuse them together as a single unit by,
for
example, heat sealing, or, alternatively, by pressure sensitive adhesive.
Preferably, the inner surface of upper member 350 will contain a screened or
printed pattern of electrically conductive material such as silver-based ink
or,
alternatively, carbon ink black, etc., which renders portions of that surface
electrically
conductive. In a preferred arrangement, the screened material is laid onto the
inner
12
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
surface of upper member 350 in such a way that at least two different
electrically
isolated circuits are created. In Figure 3B, a first circuit 335 is created
which is
preferably accessible via either connector 320 or 325. Preferably, contact
circuit 335
will contain a plurality of cross members 338 which are interleaved with the
corresponding cross members 333 from circuit 323. As can be seen, one
preferred
optional feature of this circuit is that it by measuring the resistance from
connector
320 to connector 325 it is possible to determine the actual value of the
single resistive
element 331 (i.e., to determine the actual resistance of the "calibration
resistor"). In a
preferred embodiment, the calibration resistive element 331 will be sized to
have the
same value as the sensing elements 330, although those of ordinary skill in
the art will
recognize that this is not essential. A principal reason for including such a
separate
resistive element circuit is that it permits the instant invention to
accommodate
manufacturing variations that might occur in printing the conductive portions
of the
mat 300. That is, in the preferred arrangement the resistive elements 330 and
331 will
formed of conductive ink and will be printed onto the nonconductive layer 350.
Although this method of creating the circuits 323 and 335 is very cost
effective, batch
variations in ink thickness, conductivity, etc., can cause each of the
resistive elements
to be different in value than was called for in the specification. Obviously,
to the
extent that this variation is relatively large and not otherwise accounted
for, the
determination of the patient's position on the sensor could be made
unreliable. One
method of potentially reducing this inaccuracy is by individually
recalibrating each of
the resistors each time the mat is used (e.g., by having the caregiver
successively
individually activate each of the switches 410 through 470) at the direction
of the
CPU. A more efficient alternative, however, is to separately measure the
resistive
13
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
value of calibration element 331, and provided that any manufacturing
variation that
might be present in resistive elements 330 is comparably present in
calibration
element 331, modify the calculations that are described hereinafter according
to
methods well known to those of ordinary skill in the art to account for less
than
perfect manufacturing. For example, if the resistance of the calibration
element 331 is
expected to be 100 ohms, and the actual measurement gives 90 ohms, then it is
straightforward to adjust the calculations that produce the patient's location
to reflect
this variation (e.g., by simply scaling all measured resistances by the factor
100/90).
Finally, note that another way of calibrating the preferred resistive ladder
is by putting
a constant current into connector 310 while no patient is present and reading
the
resulting voltage at 310 while grounding 315. Assuming for purposes of
illustration
that all of the resistive elements 330 have the same nominal value, this
reading will
make it possible to determine the total number of resistors in the system, as
well as
the actual total resistivity. To the extent the measured resistivity differs
from the
nominal resistivity, subsequent readings can be adjusted proportionally.
Circuit 333 is preferably accessible by both connector 310 and connector 315.
As was mentioned previously, this circuit preferably has a plurality of cross
members
333 which are interleaved with, but electrically isolated from, cross members
338 of
contact circuit 335. Additionally, circuit 333 contains a plurality of
identical resistive
elements 330 which are connected in series. By measuring the resistance across
connectors 310 and 315 it is possible to measure the total resistance in the
circuit 333.
Central spacer 355 is preferably made of a flexible and resilient material
such
as polyester and contains a plurality of apertures 340 therethrough. The
location of
each aperture 340 should at least approximately coincide with the interleaved
cross
14
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
members 333 and 338 when the surfaces 350, 355, and 360 are assembled into the
single sensor 300.
Upper member 360 preferably contains a plurality of conductive elements 380,
which at least partially span the apertures 340. In the preferred embodiment,
conductive elements 380 are configured such that when weight is placed on the
mat
300, that pressure will force the conductive elements 380 through one or more
apertures 340 and into contact with circuits 323 and 335. More particularly,
conductive elements 380 are configured such that when they come into contact
with
cross members 333 and 338 they cause an electrical short between discrete
circuits
323 and 335. Further, and is explained in more detail below, based on the
measured
resistances across connectors 310, 315, 320, and/or 325 it is possible to
reconstruct
the location of the patient on the mat, as well as the proportion of the mat
300 which
is compressed (or, more generally, occluded) by the patient, the latter
measure being
indicative of the orientation of the patient on the mat 300. Additionally, non-
conductive support elements 390 are preferably superimposed upon the
conductive
elements 380 to help prevent inadvertent contact between the conductive
elements
380 and the cross members 333 and 338 through the apertures 340 when there is
no
patient on the mat 300.
In the preferred embodiment, circuits 323 and 335 are laid onto their
respective non-conductive surfaces 350 and 360 by printing with a flexible
conductive
ink such as silver-based ink. Additionally, it is preferable for purposes of
manufacturing efficiency that resistive elements 330 be formed of the same ink
or
other conductive material as is used to create the circuits 323 and 335. As
those of
ordinary skill in the art will understand, resistive elements 330 can readily
be formed
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
to match a desired resistive value by simply adding length to the path
traveled by
electricity in completing the circuit. Because the conductive material has an
inherent
resistance, adding length to the path correspondingly increases the resistance
of the
circuit. As a consequence, in the preferred embodiment the resistive elements
330 are
formed by printing additional lengths of the same conductive material used
elsewhere
in circuits 323 and 335. One obvious advantage of this approach is that it is
more cost
effective to print all of the elements of the mat in a single pass.
Additionally, if a
discrete resistor were to be used that element could very well introduce a
hard bump
or bulge in the mat surface, which might prove to be uncomfortable for the
patient
resting thereon. That being said, those of ordinary skill in the art will
recognize that
there are many ways that resistive or other elements suitable for use with the
instant
invention could be introduced into the circuits 323 and 335.
Turning now to Figure 4, this figure contains a schematic illustration of a
preferred embodiment of the circuits of Figure 3. As can be seen, the closure
of
switches 410, 420, 430, 440, 450, 460 and/or 470 engage different numbers of
resistive elements 330. This arrangement allows the attached electronic
monitor to
determine at least approximately the position of the patient on the sensor 300
and the
number of switches (410 to 460) that have been closed by the patient's weight,
this
latter count being representative of the patient's position on the mat.
According to a preferred arrangement, given the circuit configuration of
Figure 4, it is possible to determine the position and orientation of the
patient on the
mat according to the following preferred scheme. First, as an initial
calibrating
measurement and as has been described previously, it is preferred that the
resistance
between connectors 325 and 320 be measured and, assuming that any significant
16
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
variation in ink quality or quantity has affected every resistive element 330
in the
same general fashion, this measurement can be used to determine the
approximate
resistance of a single resistive element in the circuit which then provides a
correction
factor that can be applied in subsequent calculations.
Continuing with the discussion of Figure 4, note that by measuring the
resistance (or alternatively the voltage or any other similar quantity)
between leads
315 and 320 an estimate of the patient's position on the mat may be determined
(circuit "Cl" hereinafter). More specifically, the measured resistance will be
indicative of the nearest switch (410 through 460) to the connector-end that
is
engaged. By way of example, and assuming for purposes of illustration only
that each
resistive element 330 is the same value, if contacts 440 and 450 are both
engaged, the
measured resistance between 315 and 320 will be approximately three times the
resistance of individual resistor 330. Obviously, the calculated resistive
value across
these contacts will vary depending on the precise combination of contacts that
are
engaged and the values of the resistances. Further, it is readily possible to
build a
table or develop an equation that relates the measured resistance to every
possible
position of the patient on the mat 300. For example, Table 1, which follows,
contains
a listing of voltages normalized to .,1 volt that would be measured across the
leads
indicated as a function of the number and location of switches engaged. Note
that in
the preferred embodiment, the resistive elements 330 are resistors and the
preferred
normalized resistance of each is about 100 ohms, with the values in column Cl
below
being normalized to 1 volt.
17
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
Table 1: Fractional Voltage Arising from Different Combinations of
Closed Switches 410 to 470
Row 410 420 430 440 450 460 470 Cl Fraction C2 Fraction
1 0.875 7/8 0.875 7/8
2 0.750 6/8 0.857 6/7
3 0.625 5/8 0.833 5/6
4 0.500 4/8 0.800 4/5
0.375 3/8 0.750 3/4
6 0.250 2/8 0.667 2/3
7 0.125 1/8 0.500 1/2
8 0.857 6/7 0.857 6/7
9 0.714 5/7 0.833 5/6
0.571 4/7 0.800 4/5
11 0.429 3/7 0.750 3/4
12 0.286 2/7 0.667 2/3
13 0.143 1/7 0.500 1/2
14 0.833 5/6 0.833 5/6
0.667 4/6 0.800 4/5
16 0 0.500 3/6 0.750 3/4
17 = 0.333 2/6 0.667 2/3
18 0.167 1/6 0.500 1/2
19 0.800 4/5 0.800 4/5
0.600 3/5 0.750 3/4
21 0.400 2/5 0.667 2/3
22 0.200 1/5 0.500 1/2
23 = 0.750 3/4 0.750 3/4
24 0.500 2/4 0.667 2/3
= 0.250 1/4 0.500 1/2
26 = 0.667 2/3 0.667 2/3
27 0.333 1/3 0.500 1/2
18
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
Row 410 420J 430 440 450 460 470 C1 Fraction C2 Fraction
28 11 1 11-J 0 0.500 1/2 0.500 1/2
By way of explanation, the column labeled "C 1" contains resistances
measured across contacts 315 and 320 with voltage applied to 310 and with 315
being
grounded with switches 410 through 470 closed as indicated. The values stored
in the
column labeled "C2" are the resistances measured across contacts 315 and 320
with
voltage applied to 325 and with 315 being grounded with switches 410 through
470
closed as indicated. Finally, each cell that contains a bullet therein
indicates that the
corresponding switch 410 through 470 is closed.
Note that in some instances it is necessary to measure both circuits to
uniquely
determine the location and number of switches compressed. For example, the
normalized voltage that would be observed when only switch 420 is closed
(0.75,
Row 2) is the same as would be observed if switches 410 through 450 were
closed
(0.75, Row 23). In such an instance, reference to the second circuit C2
(contacts 315
and 320) makes it possible to automatically differentiate between these two
cases, as
the C2 normalized voltages for these two conditions are 0.857 and 0.750
respectively.
Additionally, given the preferred arrangement of the instant invention, it is
also readily possible to determine using the total number of switches/contacts
that the
patient's weight has closed. Those of ordinary skill in the art will recognize
that the
resistance between contacts 315 and 320 provides such a measure, preferably
when
used in concert with the "nearest switch" calculation developed above (circuit
"C2",
hereinafter). As a specific example, consider the case where the patient's
weight has
forced switches 440 and 450 into contact. The previous calculation has will
have
19
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
determined that at least switch 450 (the nearest) has been engaged. Given this
information together with the results from Table 1, it is possible to
determine how
many contiguous switches have been closed by the patient's weight on the mat.
Of course, a principal reason for acquiring this information is so that it can
be
determined whether or not a patient has exhibited sufficient activity to skip
the next
scheduled assisted "turn". That is, in a typical arrangement a physician will
prescribe
that a patient be manually turned at some predetermined time interval, e.g.,
every two
hours, so that the patient does not rest for too long a period of time in one
position.
As has been described previously, assisted turning is disruptive to the
patient and
taxing on the staff and, to the extent that the patient has already moved
himself or
herself, it may be that the next scheduled turn may and should be skipped.
However, those of ordinary skill in the art will recognize that not every
movement by a patient is sufficient to reoxygenate the tissues that have been
compressed by the patient's weight. For example, if a patient is resting on
his or her
right side and moves laterally across the bed without changing orientation,
such a
simple relocation would not relieve pressure from the compressed tissue and,
as a
consequence, the patient would likely still need to be manually turned.
Thus, it is preferred by the instant inventors that the location information
which is obtained from the mat 300 be combined with logic (whether implemented
by
discrete logic, one or more gate arrays, analog circuitry, or via a CPU /
software
combination, etc.) to help determine whether or not the patient has moved
significantly, where a significant move is one that persists at least long
enough for
there to be sufficient reoxygenation of the previously compressed tissues.
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
According to another preferred embodiment, there is provided an invention
substantially as described above, but wherein the number of switch closures is
determined by preferably applying a constant current to connector 320 while
grounding either 310 or 315 and measuring the resulting voltage. Table 2 which
follows illustrates how various switch closures will be reflected in the
measured
voltages.
Table 2: Fractional Current Arising from Different Combinations of
Closed Switches 410 to 470
Row 410 420 430 440 450 460 470 C3 C3* C4 C4**
Volts Volts
1 =*** 2.9167 7 0.4167 1
2 2.5000 6 0.8333 2
3 2.0833 5 1.2500 3
4 1.667 4 1.667 4
5 1.2500 3 2.0833 5
6 0.8333 2 2.5000 6
7 0.4167 1 2.9167 7
8 2.5000 6 0.4167 1
9 2.0833 5 0.8333 2
10 1.667 4 1.2500 3
11 1.2500 3 1.667 4
12 0.8333 2 2.0833 5
13 0.4167 1 2.5000 6
14 2.0833 5 0.4167 1
1.667 4 0.8333 2
16 = 1.2500 3 1.2500 3
21
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
Row 410 420 430 440 450 460 470 C3 C3* C4 C4**
Volts Volts
17 0.8333 2 1.667 4
18 = = 0.4167 1 2.0833 5
19 1.667 4 0.4167 1
20 1.2500 3 0.8333 2
21 0.8333 2 1.2500 3
22 0.4167 1 1.667 4
23 1.2500 3 0.4167 1
24 = 0.8333 2 0.8333 2
25 0.4167 1 1.2500 3
26 0.8333 2 0.4167 1
27 0.4167 1 0.8333 2
28 0.4167 1 0.4167 1
By way of explanation, the values in the column headed by "C3 Volts" are the
voltages read between 320 and 315 with a constant current, for example 4.167
mA,
being applied to 320. Switches 410 through 470 are closed if a bullet is
present in the
corresponding column. The values stored in the column labeled "C4 Volts" are
the
voltages read between 320 and 310 with a constant voltage applied to 320, and
with
switches 410 through 470 being closed as indicated. If, for instance, each
resistor 330
has been chosen to be 100 ohms, the voltage drop across each is 0.4167 volts.
Thus,
the number of resistors in the circuit may be calculated (assuming a given
number of
switch closures) and the results of such a calculation may be found in the
columns in
the Table 2 labeled C3 and C4. Note that each cell in the previous table that
contains
a bullet therein indicates that the corresponding switch 410 through 470 is
taken to be
closed. The values in the column headed by "C3" are the number of resistors
read
22
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
between 320 and 315 while a constant current is applied to 320 with switches
410
through 470 being closed as indicated. The values stored in the column labeled
"C4"
are the number of resistors read between 320 and 310 with a constant voltage
being
applied to 320 and with switches 410 through 470 being closed as indicated.
As should be clear in be reference to the previous table, by monitoring the
measured voltage of the instant preferred sensor along two different paths, it
is readily
possible to determine which of the switches 410 through 470 are closed either
individually or in combination. Note that the method of determining patient
location
with this embodiment is analogous to that discussed previously in the case
where
voltage application was utilized.
In practice and as is generally illustrated in Figures 5, 6, and 11, the
instant
invention would be used as follows. As a first step, the sensor 300 would be
placed
into electronic communication with an electronic patient monitor 500.
Typically,
such a monitor 500 will contain an interface port 520 which preferably takes
the form
of a standard connector (e.g., an RJ-11-type connector) into which the sensor
cord 305
is plugged. Within the monitor 500, will preferably be found a microprocessor
620
which might additionally utilize a separate timer / clock chip 640 to assist
it in
measuring the various time intervals that are useful and necessary in the
monitoring of
an at-risk patient. Of course, those of ordinary skill in the art will
recognize that a
separate (or external) clock chip 640 is not strictly necessary and, instead,
software
timing loops could readily be used instead. Finally, it is customary to
include some
amount of computer RAM/ROM 610 in which to store program instructions and
variable values. That being said, those of ordinary skill in the art will
recognize that
such RAM/ROM 610 need not be external to the microprocessor 602 but might,
23
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
instead, be incorporated into the microprocessor 602 according to methods well
known to those of ordinary skill in the art.
Although the previous monitor embodiment 500 was microprocessor-based,
those of ordinary skill in the art will recognize that the simple
functionality that is
minimally required of this monitor could readily be implemented with discrete
logic
components. As is generally suggested in Figure 11, sensor port 1110 could be
monitored by detector 1120 which might be comprised of, by way of example
only, a
position detection circuit, a window comparator, a sample-and-hold circuit,
and a
differential amplifier circuit. The detector circuit 1120 would preferably
work in
combination with one or more timers 1130, which timers would preferably
include a
timer for monitoring the doctor-prescribed turn interval (e.g., a two-hour
timer) and a
separate timer to determine whether the patient has maintained a changed
position for
a period of time sufficient to allow reoxygenation of the previously-
compressed
tissues (e.g., a ten-minute timer). Finally, if the alarm conditions are
satisfied, an
alarm circuit 1140 would be triggered which preferably would sound an audible
alarm
via speaker 1150 which might be directly incorporated into the patient monitor
1100
or situated remotely thereto, e.g., at a nurses station.
After the patient has been placed on the sensor 300 and the monitor 500 has
been initialized, a determination of the patient's location and an estimate of
his or her
orientation will be made. The orientation will preferably be established by
reference
to the percentage of the mat 300 that is occluded. That is, if only a few
(e.g., one or
two) of the switches 410 through 470 are closed, the patient is likely lying
on his or
her side. However, if a larger number are closed (e.g., 3 or 4 or more), the
patient is
likely lying on his or her back or stomach. Of course, those of ordinary skill
in the art
24
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
will recognize that it is not the number of switches that are closed that is
determinative of the patient orientation, but rather the proportion of the
switches that
are closed when compared with the total number of switches, such a proportion
being
a measure of the length of the contact area between the patient and the sensor
300.
Thereafter, the monitor 500 will continue to monitor the patient's location
and
orientation to determine whether or not the patient has moved. However, and as
is
well known to those of ordinary skill in the art, determining whether or not
the patient
has "moved" is not enough: the patient who is lying, say, on his right side
and who
moves sideways in the bed is still in risk of decubitus ulcers. Thus, by
analyzing the
location of the patient together with the number of switches engaged it will
be
possible to tell at least approximately whether the patient has truly moved to
so that
manual turning will not be necessary. For example, if the patient's weight has
caused
only two of the switches 410-460 to be engaged, that patient is likely lying
on his or
her side. However, if the weight distribution of the patient later changes to
engage
four of the switches 410-460, it is likely that the patient has rolled onto
his or her back
or stomach. Thus, the patient is unlikely to need to be manually turned.
In a typical arrangement, the patient will be monitored continuously by an
attached electronic patient monitor during the time that he or she is bed-fast
or chair-
fast. Usually, the attending physician will prescribe a turn interval for the
patient, the
turn interval being the frequency with which the staff must manually turn the
patient
so that the compressed tissues can reoxygenate. A two-hour turn interval is
commonly used. A preferred embodiment of the instant invention operates by
determining an initial orientation of the patient on the sensor and then
thereafter
repeatedly redetermining the patient's position over time to ascertain whether
or not
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
he or she has moved. Those of ordinary skill in the art will understand that
there is no
set sampling frequency or period of time between measurements of the patient's
position that need be used, but that the sampling interval must necessarily be
shorter
than the turn interval and, preferably, will be on the order of once a minute
or so.
Further, there is no requirement that the successive checks of the patient's
position be
equally spaced in time, although that is also preferred. Thus, when the period
of time
between successive patient measurements is alluded to herein, that time period
should
be understood to be shorter than the patient's turn interval and otherwise
could be
arbitrarily closely spaced in time.
In another preferred embodiment of the instant invention, there is provided a
sensor substantially as described above, but wherein a plurality of spaced-
apart
longitudinally aligned resistive ladders are utilized so as to give a
horizontal and
vertical profile of the patient's orientation in the bed, i.e., to provide
both a
longitudinal and vertical measurement of the patient's location. As is
generally
indicated in Figure 7, in a preferred arrangement the resistive ladder of
Figures 3 and
4 is spatially configured so as to give an approximate "X" and "Y" location of
the
patient on the sensor 700, where "X" is preferably measured with respect to
the width
of the bed and the "Y" with respect to its length. As is best illustrated in
Figure 7, by
spatially varying the location of the resistive elements 330 and the switches
410 -
470, it is possible estimate, not only the lateral location of the patient on
the mat, but
also his or her vertical position relative to the head (or foot) of the bed.
In more
particular, consider the case where switches 440, and 460 are closed ("Case
1") in
comparison with the case where, say, switches 450, and 470 are closed ("Case
2").
Generally speaking, the combination of switches in Case 1 would be interpreted
as a
26
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
patient who is higher (i.e., closer to the head) of the bed than the
combination of Case
2. Thus, it should be clear that the preferred arrangement - which utilizes a
series of
staggered switches - can be used to obtain general information about the
vertical
location of the patient in the bed.
However, note that, in addition to giving an approximate "X" and "Y" position
of the patient in the bed as has been discussed previously, the instant sensor
700 can
provide dynamic / real-time information about the patient's condition by
monitoring
the changing closure patterns of its switches over time. For example, in the
previous
scenario where the closure pattern of Case 1 is followed directly by the
pattern of
Case 2, the patient is likely sliding toward the foot of the bed. Further, and
in another
preferred embodiment, this information will be utilized to estimate the amount
of
shear experienced by the patient's tissue during this time period.
Thus, in another preferred arrangement, there is provided a sensor and
attached electronic patient monitor substantially as described above, but
wherein the
patient monitor utilizes information from the time-varying switch closures to
help
identify those patient's that are at risk of decubitus ulcers by virtue of
shear stress
placed on their tissues, a sheer stress being a force that is tangent to the
skin's surface.
As is well known to those of ordinary skill in the art, the amount of shear
experienced
by a patient is increasingly recognized as another factor in predicting the
occurrence
of decubitus ulcers. A patient's sliding down in the bed is an obvious source
of such
stress, and may, indeed, cut off oxygenated blood to the patient's tissues by
capillary
deformation, thereby increasing the risk of injury. If an at-risk patient can
be
automatically identified and the staff notified, additional manual
intervention, or a
change to another bed or chair, might circumvent the occurrence of ulcer
formation
27
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
entirely. Needless to say, it is much better to prevent decubitus ulcers than
to treat
them. Additionally, shear that is caused by sliding can indicate a general
restlessness
in the patient, which might be correlated with an increase in his or her pain
or anxiety
level. Those of ordinary skill in the art will recognize the utility of being
able to
automatically identify such a change in patient condition and to notify the
staff so that
intervention is possible if it is necessary.
According to another preferred embodiment, there is provided a mat
substantially as described above, but wherein there are two or more resistive
ladders
configured in a roughly parallel arrangement. As is generally indicated in
Figure 8, in
a preferred arrangement two or more electrically isolated resistive ladders
are utilized,
each such ladder being independently accessible via connectors 810 through 825
and
830 through 845, respectively. As should be clear by reference to this figure,
switches 850 through 862 are separately readable to determine which are
closed.
These switches, in combination with switches 864 through 876 provide a
horizontal,
as well as a vertical, image of the patient's position. Given this sort of
arrangement, it
is possible to determine vertical and horizontal changes in the patient's
position and,
if desired, to estimate whether or not the patient's body is experiencing
shear. As a
specific example of how the presence of shear might be sensed, if the contract
area
(occluded region) of the mat remains constant, but the vertical (i.e., "Y")
location of
the patient indicates the he or she has moved down in the bed, the patient is
likely
being exposed to shear and the staff should be notified of this problem.
Needless to
say, there could be many more such parallel arrays of resistive elements than
the two
arrays that are illustrated in the embodiment of Figure 8.
28
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
According to still another preferred embodiment, there is provided a patient
sensor substantially as described above, but wherein each resistive element is
made
part of a separate circuit that is individual readable by the microprocessor
620. That
is, and as is generally indicated in Figure 9, in a preferred arrangement each
switch
910 through 924 is separately readable by virtue of the individual electrical
lines
coming to it. That is, rather than using a four-element electrical line 305, a
nine-
element line is preferably used instead, wherein each of the conductive
elements
leading to switches 910 through 924 is kept electrically isolated from the
others. This
means that a patient monitor in electrical communication with the embodiment
of
Figure 9 can directly determine which of the switches is closed, e.g., by
bringing each
connecting line into a separate port in the microprocessor (or other
programmable
device) of the monitor. Note that in this case, the resistive elements 330
might take
any resistive value that is greater than or equal to zero. Finally, note that
although the
switches in Figure 9 and elsewhere in this disclosure are normally opened,
those of
ordinary skill in the art will recognize that normally closed switches could
be used
instead and that the procedure for determining patient location discussed
previously
would not need to modified materially in order to determine the patient's
position.
Additionally, it should be noted in connection with Figures 4 and 9 that it
would be readily possible to create switches that are based on optical, rather
than
electrical, properties, wherein the resistive element takes the form of an
optical
attenuator. That is, if the electrical conductor 930 were instead replaced by
some sort
of optical fiber, if resistive elements 330 included sections of optical
fiber, and, if, for
example, the amplitude or frequency of light passing through the switch were
changed
(e.g., attenuated or amplified) when the patient were present on the sensor,
closure of
29
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
the switches 910 - 924 could be determined by, for example, monitoring the
amplitude of light received through lead 940.
Figure 12 illustrates a first preferred optical switch that would be suitable
for
use with an optical embodiment of the instant invention. In this embodiment a
block
of open cell foam or similar material acts as the optical attenuator. By way
of
explanation, a light source 1210 is provided at one end of an optical conduit
1220
(e.g., a section of fiber optic cable). Light is transmitted through the
optically
conductive material 1220 until it reaches optical attenuator 1230, which in
one
preferred embodiment is a low density open cell foam. A portion of the light
that falls
on the attenuator 1230 will be transmitted therethrough to optical conduit
1240 (e.g., a
section of fiber optic cable) where it will be further conducted to photo-
sensor 1250.
As is well know to those of ordinary skill in the art, when open cell foam is
compressed (e.g., via the weight of the patient on the sensor) its density
increases and
it becomes less transparent to light. Thus, by measuring the intensity of
light that is
received at photo-sensor 1250 it will be possible to determine whether or not
the foam
block is compressed and, hence, which of the switches within the sensor are
"closed".
In a preferred arrangement, an initially calibrated amount of light that is
transmitted
through the attenuator 1230 when the foam is not compressed will be
continuously
compared with the actual amount of light received from light source 1210.
According to a second preferred optical switch embodiment, and as is
generally illustrated in Figures 13A, and 13B, there is provided an optical
attenuator
which utilizes misalignment of two optical conduits as a means of attenuating
the
optical signal when the patient is present on the sensor. When the patient is
not
present on the sensor (Figure 13A) the ends of optical conduits 1320 and 1340
will be
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
in near direct alignment and much of the light that emanates from the source
conduit
1320 will be received by receiver conduit 1340, depending, of course, on the
distance
between the two conduits. The patient's weight on the sensor, which is
typically
made to be at least somewhat flexible for purposes of the increasing the
patient's
comfort, would tend to misalign the two optical conduits (Figure 13B) and
reduce the
amount of light transmitted between them. A photo-sensor 1250 in optical
communication with the receiving conduit 1340 would thus be readily able to
determine whether or not the switch was engaged depending on the level of
light
received. Preferably, a reference level of light transmissivity will be
established while
the mat is empty so that deviations therefrom can be identified. The optical
attenuation in this case is brought about by the degree of physical
misalignment
between the sections of optical conduit. Preferably a calibration value will
be
provided against which the currently measured optical intensity will be
measured
which will then provide an indication of when the termini of the two conduits
1320
and 1340 are in alignment. Pressure on the sensor (which is typically made to
be at
least somewhat flexible for purposes, of increasing the patient's comfort)
will force the
two conduits into at least partial misalignment, thereby reducing the amount
of light
transmitted therebetween (Figure 13B). Thus, by monitoring the quantity of
light
received through a plurality of such optical switches it is possible to
determine the
patient's position location on the sensor and the amount of the sensor that is
occluded
which is, of course, correlated with the patient's orientation. .
In still another preferred optical switch embodiment and as is generally
indicated in Figure 14, there is provided an optical switch suitable for use
with the
instant invention, wherein a shutter 1430 moves downward under the pressure of
the
31
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
patient's weight to block the transmission of light between source conduit
1220 and
receiver conduit 1240. Clearly, placing a photo sensor 1250 in optical
communication
with receiver conduit 1240 would make it possible to determine whether or not
the
subject switch were open and, hence, whether the patient were present on the
sensor.
As a final example of an optical embodiment of the instant invention, there is
provided in Figure 15 a preferred arrangement wherein a plurality of optical
attenuators 1530 (e.g., any of the attenuators of Figures 12 to 14, but the
embodiment
of Figure 14 would likely be best suited) are placed in series with light
collectors
1540 - 1570 interspersed in between. Preferably and for purposes of the
instant
embodiment, the light originating from all of the light collectors 1540 - 1570
will be
additively combined through junction 1595 into a single optical conduit where
it can
be read by photo-sensor 1250. For purposes of illustration only, the
attenuators will
be assumed to be the shutters 1430 of Figure 14. According to one preferred
embodiment, light sources 1510 and 1520 will be positioned at opposite ends of
the
light conduit 1590 and alternately activated. That is, light source 1510 will
be
activated while source 1520 is dark, and then light source 1510 will be
darkened
while source 1520 is activated. The reason for this arrangement is that it
allows a
patient's location and occlusion to be readily determined using a single photo-
sensor
1250. If, for example, optical attenuators 1532 - 1535 are engaged (i.e., the
shutters
of these optical attenuators are in the "down" or blocking position) light
from source
1510 will be received only at, collector 1540, with the remaining collectors
1545 -
1570 being dark. However, when optical source 1520 is activated, light will be
received at collectors 1560 through 1570, with the remaining collectors being
dark
(i.e., 1540 through 1555) being dark. Given this information, it is possible
to
32
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
determine the number of switches open (or engaged) on the left and on the
right and,
thus, the position and amount of occlusion of the sensor by the patient. Note
that in
many ways the operation of the optical embodiment of Figure 15 is analogous to
the
operation of the electrical embodiment of Figure 4. Finally, note that, if
desired a
calibration optical attenuator 1539 could added so that, by reading the amount
of light
transmitted therethrough and comparing the observed value with the presumably
known nominal value for this element, a correction factor could be established
that
could be applied to the other attenuators 1531 - 1538.
Note that if a microprocessor is utilized as a component of the monitor 500,
the only requirement that such a component must satisfy is that it must
minimally be
an active device, i.e., one that is programmable in some sense, that it is
capable of
recognizing signals from a bed mat or similar patient sensing device, and that
it is
capable of initiating the sounding of one or more alarm sounds in response
thereto. Of
course, these sorts of modest requirements may be satisfied by any number of
programmable logic devices ("PLD") including, without limitation, gate arrays,
FPGA's (i.e., ' field programmable gate arrays), CPLD's (i.e., complex PLD's),
EPLD's (i.e., erasable PLD's), SPLD's (i.e., simple PLD's), PAL's
(programmable
array logic), FPLA's (i.e., field programmable logic array), FPLS (i.e., fuse
programmable logic sequencers), GAL (i.e., generic array logic), PLA (i.e.,
programmable logic array), FPAA (i.e., field programmable analog array), PsoC
(i.e.,
programmable system-on-chip), SoC (i.e., system-on-chip), CsoC (i.e.,
configurable
system-on-chip), ASIC (i.e., application specific integrated chip), etc., as
those
acronyms and their associated devices are known and used in the art. Further,
those
of ordinary skill in the art will recognize that many of these sorts of
devices contain
33
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
microprocessors integral thereto. Thus, for purposes of the instant disclosure
the
terms "processor," "microprocessor" and "CPU" (i.e., central processing unit)
should
be interpreted to take the broadest possible meaning herein, and such meaning
is
intended to include any PLD or other programmable device of the general sort
described above.
Additionally, in those embodiments taught herein that utilize a clock or timer
or similar timing circuitry, those of ordinary skill in the art will
understand that such
functionality might be provided through the use of a separate dedicate clock
circuit or
implemented in software within the microprocessor. It might further be
obtained with
discrete, linear, timers and logic circuitry: a microprocessor is not strictly
required,
but is merely convenient. Thus, when "clock" or "time circuit" is used herein,
it
should be used in its broadest sense to include both software and hardware
timer
implementations.
Finally, and according to still another preferred embodiment, there is
provided
a patient sensor substantially similar to that disclosed previously, but
wherein the
number of connecting electrical leads has been reduced. As is illustrated
generally in
Figure 10, those of ordinary skill in the art will recognize that by using
diodes 1005 it
is possible to eliminate connectors 310 and 315 and replace them with a single
electrical lead 1010. That being said, it should be noted that, in reality,
the number of
connectors has not been reduced but rather only the number of interconnects.
As a
consequence, for purposes of the instant disclosure and the claims that
follow, when it
is noted that three conductors are required, that language should not be
limited to
those cases where three discrete interconnects are utilized, but rather should
be
understood in the broader sense to mean any configuration of conductors and
34
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
connectors that is adequate to allow an attached electronic patient monitor to
determine the number of switch closures when a patient is present on the
sensor.
CONCLUSIONS
Although the preferred embodiment of the instant invention utilizes a ladder
of
electrical resistors to determine the position of the patient on the sensor,
it should be
clear to those of ordinary skill in the art that capacitive or inductive
elements, some
combination of same, semiconductors. (e.g., forward biased diodes or zener
diodes),
temperature sensors (e.g., thermocouples), piezoelectric elements, etc. could
readily
be used instead. Of course, rather than measuring the resistance across leads
310
through 325 it would be possible to measure the resonance time constant (RC or
LC
time constant) or some other quantity representative of the number of circuits
that are
closed in the mat. In fact, the instant invention could also be configured to
operate by
calculating the various travel times of an electronic pulse that is sent
through the
instant circuitry (e.g., as measured by a Ditmico tester). Note that, in the
preferred
embodiment, the resistive elements 330 are preferably created by screening
additional
lengths of the electrically conductive material onto the mat surface, thereby
creating
increased resistance. This additional length would also result in an increased
travel
time as well, so a technique that measured the travel time of an electronic
pulse from,
say, 320 to 310 and from 315 to 320 would be able to determine the number of
switches closed by the patient's weight. Thus, as used herein, when the term
"resistive value" is used to describe the measurement of some electrical
property of
the circuit, it should be understood that the quantity that is actually
measured might be
different from "resistance" and, instead, could be any other property that is
representative of the number of switches that are closed in the attached mat
including,
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
without limitation, capacitance, voltage, transit time, etc. Similarly, when
reference is
made herein to electrical properties, electrical conductors, and electrical
resistors that
same language should be understood to also include optical properties, optical
conductors, and optical attenuators.
Additionally, although the preferred arrangement includes an array of
identical
resistive elements, those of ordinary skill in the art will recognize that
this
arrangement is not required. It is certainly possible that some combination of
different-valued resistive elements (e.g., different resistor values) might be
used and,
in such a circumstance, methods similar to those discussed herein could be
used to
determine exactly which switches are closed when a patient is present on the
device.
Those of ordinary skill in the art will recognize that the preferred
embodiment,
with its plurality of switches, could easily be manufactured with any number
of
separate switches. At the limit, of course, these switches when spaced closely
together begin to approximate a continuum of contact points. Thus, it should
be noted
and remembered that the instant inventors have determined that the invention
taught
herein might be implemented in substantially the same way in the form of a
single
continuous resistive element. In such an embodiment, preferably the single
continuous resistive element will be used with a plurality discretely spaced
activation
(e.g., switches 410 through 460), the goal being to determine the nearest
point of
contact of the patient to one end of the mat and the occluded / contact area.
Further, note that the instant invention may be utilized to detect when a
patient
is moving toward the edge of the sensor with the intent of exiting the bed. It
should
be clear that if none of the mat switches are engaged, the patient is no
longer present
on the mat and, presumably, will have left the bed or chair into which he or
she had
36
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
been placed. Thus, the instant invention can function in connection with a
conventional "exit monitor" and be used to signal the nursing staff when a
patient has
risen. This much should be clear. However, note that, because the preferred
mat
embodiment has numerous switches distributed along its length, it is possible
to
utilize the instant invention determine when a patient is preparing to leave
the bed
and, if so desired, signal that intent to the nursing staff. Note that the
preferred
embodiment has switches distributed throughout the length of the mat,
including
switches that are proximate to each end. Typically, when a patient is
intending to
leave the bed, his or her weight is relocated laterally to the exit side as a
prelude to
exiting. Further, the speed with which the patient moves toward the edge of
the bed
may also be telling, with faster movements toward the bed edge usually being
indicative of a patient that is preparing to exit the bed. Through the use of
the instant
invention, it is possible to determine when the patient's weight so-shifts by
looking
for instances when only the switches proximate to one end of the mat are
engaged.
Additionally, the velocity at which the patient moves toward the edge may also
be
calculated. In the event that the patient approaches the edge of the bed and /
or
approaches the edge of the bed in excess of a predetermined velocity, a signal
will
preferably be sent to the nursing staff, thereby allowing the staff to
intervene before
the patient has had time to stand and fall.
Additionally, although it is preferred that the instant sensor be placed under
the patient's hips or back, that is not the only possible orientation. Of some
additional
concern is the condition of the patient's heels, elbows, and other bony
prominences.
Each of these sites can potentially be a site at which decubitus ulcers can
develop.
Although the sensor of the instant invention could certainly be positioned
under any
37
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
of these areas and/or multiple sensors could be used (e.g., one under each
area of
concern), more practically speaking the those of ordinary skill in the art
will recognize
that monitoring the patient's movement at his or her hips allows at least some
general
inferences about the other locations of concern (e.g., if the patient has
rolled on his or
her side it is likely that the heels are in a position to reoxygenate, etc.)
Further, it should be noted and remembered that, although a preferred
embodiment of the instant invention employs a discrete central spacer, that is
not
absolutely required. That is, it is certainly possible that the role of the
"spacer" could
be filled by a series of noncontiguous nonconductive "dots" or other discrete
shapes
that have been imprinted across the conductive elements 380 (e.g. the support
elements 390). Thus, for purposes of the instant invention, the terms "spacer"
and
"central spacer" should be broadly interpreted to include any structure that
serves to
separate the upper 350 and lower 360 members of the instant invention when
there is
no weight on the mat 300. Similarly, when the central spacer is described as
having
"apertures", it should be recognized that these might take the form of the
embodiment
of Figure 3 (i.e., holes formed within an otherwise solid central member) or
they
might take them form of spaces between adjacent support members (e.g., non-
conductive dots), etc. In any case, a principle function of the "apertures" is
to allow
the upper 350 and lower 360 members to come into contact when pressure is
applied
to the mat and, thus, any sort of structure that permits or facilitates that
operation
should be considered to be an "aperture" for purposes herein.
Additionally, although it is preferable that the resistive elements 330 be
screened onto the inner face of the mat 300 and thus be integrated with the
mat, it
should be clear that separate discrete electronic components could readily be
used
38
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
instead. For example, discrete resistors could be affixed to the mat 300 to
serve in
place of screened-on resistive elements 330. Those of ordinary skill in the
art will
recognize that such an arrangement - provided that some provision were to be
made
so that the resistors could not be felt through the mat 300 by the patient -
would
function identically to the preferred embodiment discussed above.
Note further that a preferred electronic monitor of the instant invention
utilizes
a microprocessor with programming instructions stored therein for execution
thereby,
which programming instructions define the monitor's response to the patient.
Although ROM is the preferred apparatus for storing such instructions, static
or
dynamic RAM, flash RAM, EPROM, PROM, EEPROM, or any similar volatile or
nonvolatile computer memory could be used. Further, it is not absolutely
essential
that the software be permanently resident within the monitor, although that is
certainly preferred. It is possible that the operating software could be
stored, by way
of example, on a floppy disk, a magnetic disk, a magnetic tape, a magneto-
optical
disk, an optical disk, a CD-ROM, flash RAM card, a ROM card, a DVD disk, or
loaded into the monitor over a network as needed. Additionally, those of
ordinary
skill in the art will recognize that the memory might be either internal to
the
microprocessor, or external to it, or some combination. Thus, "program memory"
as
that term is used herein should be interpreted in its broadest sense to
include the
variations listed above, as well as other variations that are well known to
those of
ordinary skill in the art.
Additionally, although the preferred embodiment of the instant invention
utilizes a plurality of resistive elements 330 organized in a serial
arrangement,
alternative circuit configurations (e.g., parallel, or some other arrangement)
could
39
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
certainly be employed instead. All that is required for purposes of the
instant
invention is that the mat circuit, what ever its configuration, be capable of
determining at least an occluded / contact region and a location from one end
of the
mat. Of course, a sensor which yielded a distance from each end of the mat
would
allow an immediate calculation of the occluded or contact region. Those of
ordinary
skill in the art will be able to devise many alternative configurations of the
instant
invention beyond those suggested herein.
Further, it should be noted and remembered that, although the preferred
embodiment of the instant invention has the two circuits 323 and 335 and the
resistive
elements 330 and 331 all physically located on the same surface of mat 300, it
should
be clear that various permutations of this arrangement are possible. Indeed,
the only
requirement is that the resistive elements 330 be in electrical communication
with the
circuits 323 and 325 so that the sensor 300 functions as has been described
previously. Thus, it would be within the spirit of the instant invention if
the resistive
elements 330 were to be located, say, on the central spacer 355 or on the
inner face of
mat surface 360. Similarly, the two circuits 323 and 335 need not be
physically
resident on the same mat element 350, but could instead be on opposite mat
elements
so long as they can be selectively closed to indicate at least a patient's
approximate
lateral location as a function of the number of switches closed. Additionally,
those of
ordinary skill in the art will recognize that it is certainly possible that
the sensor 300
might be made a part of, or incorporated, into the bed itself or some other
structure.
Finally, it should be noted that the term "nurse call" as that term has been
used herein should be interpreted to mean, not only traditional wire-based
nurse call
units, but more also any system for notifying a remote caregiver of the state
of a
CA 02532600 2006-01-16
WO 2005/082250 PCT/US2004/022348
patient, whether that system is wire-based or wireless (e.g., R.F.,
ultrasonic, IR link,
etc.). Additionally, it should be clear to those of ordinary skill in the art
that it may or
may not be a "nurse" that monitors a patient remotely and, as such, nurse
should be
broadly interpreted to include any sort of caregiver, including, for example,
untrained
family members and friends that might be signaled by such a system.
Thus, it is apparent that there has been provided, in accordance with the
invention, a patient sensor and method of operation of the sensor that fully
satisfies
the objects, aims and advantages set forth above. While the invention has been
described in conjunction with specific embodiments thereof, it is evident that
many
alternatives, modifications and variations will be apparent to those skilled
in the art
and in light of the foregoing description. Accordingly, it is intended to
embrace all
such alternatives, modifications and variations as fall within the spirit of
the appended
claims.
41