Note: Descriptions are shown in the official language in which they were submitted.
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
METHOD AND APPARATUS FOR TREATMENT OF VAGINAL ANTERIOR REPAIRS
[0001] FIELD OF THE INVENTION
[0002] The penile implant has been used for decades and provides a selected
This
invention relates generally to the field of urogenital surgery. More
specifically, this
invention relates to the treatment of vaginal or vault prolapse and to a
device suitable
for use in such treatment.
[0003] BACKGROUND OF THE INVENTION
[0004] Vault or vaginal prolapse develops when intra-abdominal pressure pushes
the
vagina outside the body. This condition develops when the utero-sacral
ligaments,
which hold the vagina in position within the body cavity, are severed or
damaged. The
result of such damage is that the vagina has a tendency to invert which is
uncomfortable and unhealthy, and renders the vagina unsuitable for
intercourse.
[0005] Many techniques have been tried to correct or ameliorate the prolapse
and its
symptoms, with varying degrees of success. Nonsurgical treatment of prolapse
involves measures to improve the factors associated with prolapse, including
treating
chronic cough, obesity, and constipation. Other nonsurgical treatments may
include
pelvic muscle exercises or supplementation with estrogen. These therapies may
alleviate symptoms and prevent worsening, but the actual hernia will remain.
Vaginal
pessaries are the primary type of nonsurgical treatment, but there can be
complications
due to vaginal wall ulceration.
[0006] There is a desire to obtain a minimally invasive yet highly effective
device and
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
method that can be used to treat pelvic organ prolapse with minimal to no side
effects.
Such a device should reduce the complexity of the surgical procedure, be
biocompatible, adjustable, and non-toxic. The treatment methods using the
device
should reduce pain, operative risks, infections and post operative hospital
stays.
Further, the method of treatment should also improve the quality of life for
patients.
[0007] SUMMARY OF THE INVENTION
[0008] The invention includes a method and apparatus for cystocele repair. In
one
embodiment, the method includes the steps of: establishing four pathways in
tissue
around a bladder of a patient, introducing an attachment arm into each of the
pathways,
and positioning a support member beneath the bladder of the patient. The
support
member is configured to allow for a variable attachment-arm position, wherein
the
support member has each of the attachment arms connected thereto such that the
bladder of the patient is supported by the support member. A bulge of the
bladder into
a vagina of the patient is reduced as a consequence of applying this method.
[0009] In another embodiment, an apparatus for repairing cystocele includes a
support
surface knitted with a pair of superior attachment arms, and a pair of
inferior attachment
arms, wherein the distance between the pair of superior attachment arms and
the pair
of inferior attachment arms can be increased or decreased.
[00010] In another embodiment, the invention includes a kit for repairing
cystocele.
The kit includes a support apparatus including a pair of superior attachment
arms and a
pair of inferior attachment arms. Each of the attachment arms includes a
connector
2
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
configured to removably mate with a tip of a needle. The kit further includes
a first
needle configured to extend from an incision on the left side of the patient
where a left
inferior edge of the pubic ramus bone of the patient ends at the bottom of the
left
obturator foramen of the patient, through the left obturator foramen of the
patient, to an
incision in the vagina of the patient; and a second needle configured to
extend from an
incision on the right side of the patient where a right inferior edge of the
pubic ramus
bone of the patient ends at the bottom of the right obturator foramen of the
patient,
through the right obturator foramen of the patient, to the incision in the
vagina of the
patient.
[00011] In another embodiment, a surgical implant kit includes an adjustable
support
apparatus including at least two pairs of attachment arms, each of the
attachment arms
comprises a connector configured to removably mate with a tip of a needle.
Each
connector has an aperture configured to receive the tip of the needle. Each
aperture
has a different shape. The kit further includes at least two needles, each
needle having
a tip having a shape configured to removably mate with one aperture of the at
least two
connectors.
[00012] In another embodiment, a surgical implant kit includes an adjustable
support
apparatus including at least two pairs attachment arms, wherein the distance
between
the respective pairs of attachment arms is adjustable. Each of the attachment
arms
includes a connector configured to mate with a tip of a needle, wherein the
connector is
capable of being subsequently removed and reattached to the needle. Each
connector
has identifying indicia thereon. The kit further includes at least two
needles.
[00013] In yet another embodiment, the invention includes a surgical implant
kit
3
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
including an adjustable support apparatus having at least two pairs of
attachment arms.
Each of the attachment arms includes a connector configured to removably mate
with a
tip of a needle. The kit further includes at least four needles, each needle
having a
handle and each handle having a color matching a color of a corresponding
connector.
[00014] BRIEF DESCRIPTION OF THE DRAWINGS
[00015] A more complete appreciation of the invention and many of the
attendant
advantages thereof will be readily obtained as the same becomes better
understood by
reference to the following detailed description when considered in connection
with the
accompanying drawings, wherein:
[00016] Figure 1 is a fragmentary top view of a variable attachment arm
support
apparatus;
[00017] Figure 2 is a fragmentary top view of an alternative embodiment of the
variable
attachment arm support apparatus;
[00018] Figure 3 is a side view of an attachment arm of a variable attachment
arm
support apparatus of the present invention;
[00019] Figure 4 is a top view of an attachment arm of a variable attachment
arm
support apparatus of the present invention;
[00020] Figure 5 is a fragmentary top view of the variable attachment arm
support
apparatus that has been modified in accordance with the present invention;
[00021] Figure 6 is a fragmentary top view of the variable attachment arm
support
apparatus that has been modified in accordance with the present invention;
[00022] Figure 7 is a close up view of the weave pattern of an embodiment of
the
4
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
variable attachment arm support apparatus;
[00023] Figure 8 is a close up view of an alternate weave pattern for the
variable
attachment arm support apparatus;
[00024] Figure 9 is a top view of a surgical kit of an embodiment of the
present
invention;
[00025] Figure 10 is a perspective view of an embodiment of a right superior
needle
(the superior needle held in the surgeon's right hand) of the present
invention;
[00026] Figure ills a top view of an embodiment of the right superior needle
of the
present invention;
[00027] Figure 12 is a bottom view of an embodiment of the right superior
needle of
the present invention;
[00028] Figure 13 is a left side view of an embodiment of the right superior
needle of
the present invention;
[00029] Figure 14 is a right side view of an embodiment of the right superior
needle of
the present invention;
[00030] Figure 15 is a front view of an embodiment of the right superior
needle of the
present invention;
[00031] Figure 16 is a rear view of an embodiment of the right superior needle
of the
present invention;
[00032] Figure 17 is a side perspective view of an embodiment of a left
inferior needle
shaft of the present invention, without a handle;
[00033] Figure 18 is a front perspective view of an embodiment of the left
inferior
needle shaft of the present invention, without a handle;
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
[00034] Figure 19 is a right side view of an embodiment of a left inferior
needle shaft of
the present invention, without a handle;
[00035] Figure 20 is a bottom view of an embodiment of the left inferior
needle shaft of
the present invention, without a handle;
[00036] Figure 21 is a front view of an embodiment of the left inferior needle
shaft of
the present invention, without a handle;
[00037] Figure 22 is a front view of an embodiment of a set of four needles
and a
support apparatus with four connectors, wherein the connectors are matched to
the
needles using colors;
[00038] Figure 23 is a perspective view of a first needle tip and removable
connector of
an embodiment of the present invention;
[00039] Figure 24 is a perspective view of a second needle tip and removable
connector of an embodiment of the present invention;
[00040] Figure 25 is a front view of a patient showing the four needle entry
incisions;
[00041] Figure 26 is a perspective view of a right superior needle tip
entering the left
superior incision (the superior incision on the patient's left side);
[00042] Figure 27 is a perspective view of a right superior needle tip exiting
the vaginal
incision;
[00043] Figure 28 is a front view of a right superior needle tip exiting the
vaginal
incision;
[00044] Figure 29 is a perspective view of a right superior needle tip
connected to the
right superior connector (the superior connector on the surgeon's right side);
[00045] Figure 30 is a perspective view of the superior attachment arms and
the
6
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
support member in place and the inferior attachment arms extending outside the
vaginal
incision;
[00046] Figure 31 is a perspective view of a right inferior needle tip exiting
the vaginal
incision;
[00047] Figure 32 is a perspective view of all the attachment arms and the
support
member in place and the sheaths removed;
[00048] Figure 33 is a top cross-sectional view of a removal tool disengaging
a
connector from a needle tip during a first phase.
[00049] Figure 34 is a top cross-sectional view of a removal tool disengaging
a
connector from a needle tip during a second phase.
[00050] DETAILED DESCRIPTION OF THE PREFERRED EMBODIMENTS
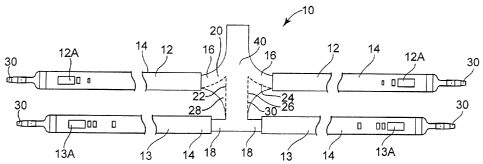
[00051] Referring now to the drawings, wherein like reference numerals
designate
identical or corresponding parts throughout the several views, figures 1
illustrates a
variable attachment surgical support apparatus 10 of the present invention.
The
apparatus 10 is configured to be surgically implanted in a female patient to
repair
anterior prolapse of the vagina. The present invention may be used to correct
central
defects, midline defects, or both midline and central defects at once. In the
embodiment
shown in Figures 1, apparatus 10 comprises two superior attachment arms 12,
two
inferior attachment arms 13, and a support member 40. Each of attachment arms
12
and 13 include a connector 30. Each attachment arm 12 and 13 is covered by a
sheath
14. Attachment arms 12 and 13 are connected to support member 40 by known
means.
7
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
[00052] Sheath 14 is preferably of fabricated of polyethylene, although a
variety of
materials, such as polypropylene, nylon, polyester, or TeflonTm may be used
while
remaining within the scope of the invention. The sheath is configured to be
removed
from the attachment arm after the attachment arm is in the desired position in
the body.
[00053] Attachment arms 12 and 13 are preferably about 19 inches long and
about
0.433 inches wide. The attachment arms 12 and 13 are about 0.024 inches thick.
Attachment arms 12 and 13 are fabricated of a knit 4 or 6 mil polypropylene
monofilament and are heat set at about 280-300 degrees Fahrenheit for 5-8
minutes.
Also, in one embodiment, support member 40 is about 10 cm long by about 5 cm
wide
and about 0.021 inches thick. Member 40 is knitted of 4 mil polypropylene
monofilament and heat set at about 310-330 degrees Fahrenheit for about 5-8
minutes.
Both the attachment arm and support member have a stitch count of 27.5
courses/inch
( 2 courses) and 13 wales/inch ( 2 wales).
[00054] In another embodiment, the attachment arms are knitted with bar
settings of:
Bar 1:1/0, 2/1 and Bar 2: 0/1, 1/2. The support member is a large pore mesh,
knitted
with bar settings of: Bar 1:1/0, 2/3, 211, 2/3, 1/0, 1/2, 1/0, 1/2; Bar 2:
1/0,2/3,2/3, 1/0;
and Bar 3:2/3, 1/0, 112, 1/0, 2/3, 2/1, 2/3, 2/1. The attachment arms are
connected to
the support member after knitting. Weaving according to a given bar pattern is
described, for example, in "Warp Knitting Production" by Dr. S. Raz, Melliand
Textilberichte GmbH, Rohrbacher Str. 76, D-6900 Heidelberg, Germany (1987),
the
contents of which are incorporated by reference herein.
[00055] Attachment arms 12 and 13 and or sheaths 14 may also include indicia
thereon to signify the correct orientation for implantation into a patient.
The indicia may
8
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
include various markings, colors, apertures, symbols, or combinations thereof.
Further,
the indicia may be located on the attachment arms, the sheaths, or both. In
the
embodiment shown in Figures 1 and 2, sheaths 14 around attachment arms 12
include
indicia 12A to show that attachment arms 12 are the superior attachment arms,
and
sheaths 14 around attachment arms 13 include indicia 13A to show that
attachment
arms 13 are the inferior attachment arms.
[00056] Apparatus 10 includes dilating connectors 30. Suitable dilating
connectors are
disclosed in Published U.S. Patent Application Serial Nos. 2002/151762 and
2002/147382 and U.S. Patent Application Serial No. 10/386,897, filed Mar. 11,
2003.
[00057] Before implantation, support member 40 may be trimmed based on patient
anatomy to provide a variable attachment arm position. Shape of support member
40
allows the attachment arm positions to be customized to repair a cystocele
without
lifting a patient's bladder and without placing undue tension on the bladder
or vaginal
wall. For example, Figure 1 illustrates a support member configured to
maximize the
distance between superior arms 16 and the inferior arms 18. Support 40 is cut
along
lines 20 and 22 to remove section 28. Similarly, support 40 is cut along lines
24 and 26
to remove section 30. This results in the configuration illustrated in Figure
5. In this
configuration, the distance between superior arms 16 and inferior arms 18 can
be
maximized. Superior arms 16 are flexible to allow for movement to a position
substantially parallel to inferior arms 18, or a position substantially skewed
to inferior
arms 18.
[00058] An alternative embodiment of the variable attachment surgical support
apparatus 10 is shown in Figure 2. Before implantation, support member 40 can
be
9
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
trimmed to minimize the distance between superior arms 16 and the inferior
arms 18.
Support 40 is cut along lines 42 and 32 to remove section 38. Similarly,
support 40 is
cut along lines 34 and 36 to remove section 44. This results in the
configuration
illustrated in Figure 6. In this configuration, the distance between superior
arms 16 and
inferior arms 18 can be reduced. Superior arms 16 are flexible to allow for
movement to
a position substantially parallel to inferior arms 18, or a position
substantially skewed to
inferior arms 18.
[00059] With reference to Figures 3 and 4, an embodiment of a attachment arm
for a
surgical apparatus is shown. In one embodiment, attachment arm 12 includes
tensioning suture 17. Tensioning suture 17 passes through the mesh of
attachment
arm 12 multiple times, as shown in Figures 3 and 4. Tensioning suture 17 is
affixed to
attachment arm 12 at points 19, to allow transfer of tension from the suture
to the
attachment arm. In one embodiment, tensioning sutures are included in all the
attachment arms 12 and 13 of the support apparatus. Tensioning suture 17 is
configured to eliminate slack in a attachment arm that is already surgically
implanted in
the body. By tightening the attachment arm with suture 17, rather than pulling
on the
attachment arm itself, the surgeon prevents damage to the attachment arm due
to
deformation. Damage to surrounding tissues due to excessive movement of the
attachment arm during adjustment can also be avoided. Attachment arm 12 also
includes a connection point for loosening suture 16. Loosening suture 16 is
pulled by
the surgeon to loosen the installed support member, if necessary.
[00060] Apparatus 10 can be fabricated from a variety of synthetic and non-
synthetic
material. Suitable non-synthetic materials include allografts, homografts,
heterografts,
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
autologous tissues, cadaveric fascia, autodermal grafts, dermal collagen
grafts,
autofascial heterografts, whole skin grafts, porcine dermal collagen,
lyophilized aortic
homografts, preserved dural homografts, bovine pericardium and fascia lata.
Other
examples of suitable materials include those disclosed in published U.S.
patent
application Ser. No. 200210072694. Specific examples of synthetic materials
include,
but are not limited to, polypropylene, cellulose, polyvinyl, silicone,
polytetrafluoroethylene, polygalactin, Silastic, carbon-fiber, polyethylene,
nylon,
polyester (e.g. Dacron) polyanhydrides, polycaprolactone, polyglycolic acid,
poly-L-lactic
acid, poly-D-L-lactic acid and polyphosphate esters. See Cervigni et al., The
Use of -
Synthetics in the Treatment of Pelvic Organ Prolapse, Current Opinion in
Urology
(2001), 11:429-435.
[00061] With reference to Figure 9, in another aspect, the present invention
includes a
surgical kit 400. The kit 400 preferably includes at least two superior
needles 70R and
70L. Right superior needle 70R is configured to be held in the surgeon's right
hand and
such that the tip of the needle enters an incision on the left side of the
patient where the
left adductor longus tendon of the patient inserts into a left portion of the
pubic ramus
bone of the patient, lateral to the edge of the pubic ramus bone, and travels
through the
top of the left obturator foramen to exit through an incision in the vagina of
the patient.
Left superior needle 70L is configured to be held in the surgeon's left hand
and such
that the tip of the needle enters an incision on the right side of the patient
where the
right adductor longus tendon of the patient inserts into a right portion of
the pubic ramus
bone of the patient, lateral to the edge of the pubic ramus bone, and travels
through the
top of the right obturator foramen to exit through an incision in the vagina
of the patient.
11
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
[00062] In alternative embodiments of the present invention, the kits may
further
include the needles described in published U.S. patent application Ser. Nos.
20023-
006S246-Al; 2002-0151762-A1; 2002-0147382-A1; 2002-0107430-A1, U.S. patent
application Ser. No. 2002-0099258-A1 and U.S. patent application Ser. No. 2002-
0099259-A1; and U.S. Provisional Application Serial Nos. 60/263,472, filed
Jan. 23,
2001; 60/269,829, filed Feb. 20, 2001; 60/281,350, filed Apr. 4, 2001;
60/295,068, filed
Jun. 1, 2001; 60/306,915, filed Jul. 20, 2001, and 60/332,330, filed Nov. 20,
2001. In an
embodiment that is particularly suitable for a. transobturator surgical
procedure, the
needles include needles as described in U.S. patent application Ser. No.
10/306,179
filed Nov. 27, 2002.
[00063] Various elements of the kits of the present invention may be packaged
together as shown in Figure 9 with a cover 52 and tray 54. Alternatively, the
individual
elements may be separately packaged or packaged in subassemblies depending on
a
variety of factors such as shelf life and sterilization requirements. They may
be
assembled at the manufacturing location or at the healthcare location. Any
suitable
sterilization procedure may be utilized to sterilize the contents of a kit.
Suitable
sterilization techniques include, but are not limited to, steam, ethylene
oxide, electron
beam, vapor (e.g. hydrogen peroxide or peracetic acid), gamma or plasma
procedures.
[00064] The kit shown in Figure 9 includes a support apparatus including a
mesh
support member 40. It should be readily apparent to one skilled in the art
that kits using
biological support members, as described above, may be made, and these
modifications are within the scope of the invention as claimed. Further, a kit
comprising
a biologic graft may have the biologic graft pre-attached to the attachment
arms, or the
12
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
graft may be separate from the attachment arms and require the surgeon to
attach the
attachment arms to the graft, as discussed below. The kit shown in Figure 9
also
includes four needles: right inferior needle 60R, left inferior needle 601_,
right superior
needle 70R, and left superior needle 70L. Embodiments of these needles are
shown in
Figures 10-21 and are described herebelow.
[00065] Figures 10-16 illustrate an embodiment of right superior needle 70R of
the
present invention. (Left superior needle 70L is a mirror image of the right
superior
needle 70R.) Right superior needle 70R includes indicia 71R, handle 72R, shaft
74R,
curved portion 76R, and tip portion 78R. lndicia 71R designates whether the
needle is
the right or left needle by pointing to the surgeon's right or left side, as
the surgeon
holds the needle handle. (The surgeon's right side corresponds to the
patient's left
side.)
[00066] An exemplary shaft of left inferior needle 60L without handle 62L is
illustrated
in Figures 17-21. (Right inferior needle 60R is a mirror image of the left
inferior needle
60L.) Left inferior needle 601_ includes a handle 62L, a shaft 64L, a curved
portion 66L,
and a tip portion 68L. Left inferior needle 60L is configured to be held in a
surgeon's left
hand such that tip 68L enters an incision 530L on the right side of the
patient where a
right inferior edge of the pubic ramus bone of the patient ends at a bottom of
the right
obturator foramen of the patient, and travels through the right obturator
foramen to exit
through an incision in the vagina of the patient. Right inferior needle 60R is
configured
to be held in a surgeon's right hand such that tip 68R enters an incision on
the left side
of the patient where a left inferior edge of the pubic ramus bone of the
patient ends at a
bottom of the left obturator foramen of the patient, and travels through the
left obturator
13
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
foramen to exit through an incision in the vagina of the patient. This is
shown in Figure
31. The above-described needles may be disposable or reusable.
[00067] Figures 23 and 24 are perspective views of a needle tips having a
cross
sections that are configured to match the cross sections of a connector
aperture. Figure
23 shows that the cross section of portion 450 of needle tip portion 478 is a
triangle.
The cross section of portion 450 matches triangle shaped aperture 460 in
connector
490. Figure 24 shows that the cross section of portion 451 of needle tip
portion 479 is a
square. The cross section of portion 451 matches square shaped aperture 461 in
connector 491.
[00068] In one embodiment each needle tip has a cross section that matches the
cross
section of an aperture of the corresponding connector, and the tip cross
section is
incompatible with the other connector apertures. For example, the cross
section of the
portion 450, a triangle, would not fit in aperture 461, a square, and vice
versa. Thus,
even if the connectors are confused, it is physically impossible for a surgeon
to insert
the needle tip in the incorrect connector without damaging the tip or
connector. Other
shaped tips and apertures are possible while remaining within the scope of the
invention.
[00069] Figures 25-32 illustrate an exemplary method for using the disclosed
surgical
support apparatus 10 having a mesh support member 40. In preparation for
surgery,
the patient is placed in a modified dorsal lithotomic position with hips
flexed, legs
elevated in stirrups and buttocks even with edge of the surgical table. The
patient's
bladder is emptied. A catheter is not required during the procedure, but may
aid in
identifying the urethra during the procedure. A weighted vaginal retractor or
other
14
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
suitable vaginal retraction may also be used.
[00070] Next, it is necessary to mark the length of the vaginal incision with
a skin
pencil starting below the bladder neck, over the most prominent part of the
prolapse, to
the lowermost part of the prolapse. (Variations may occur in specific
incisions due to
individual technique and patient anatomy.) An incision is made over this
marking. The
incision site may be infiltrated with saline, if desired. An Allis forceps is
placed on the
incision margin to expose the incision. The patient's bladder is dissected off
the vagina
up to the lateral sulcus and posterior to the vaginal vault. This dissection
allows
palpation of the medial edge of the inferior pubic ramus, assisting in guiding
the superior
and inferior needles to the exit points free from the bladder. The patient's
cystocele
may then be reduced using midline plication.
[00071] Markings are then made to identify the locations for needle entry
incisions.
The vaginal dissection is completed prior to marking needle entry incisions to
allow for
digital palpation along the ischiopubic ramus. The needle entry points are
palpated
internally and externally with the thumb and index finger before marking, as
discussed
hereafter.
[00072] Next, the edge of the ischiopubic ramus is palpated beginning at the
level of
the vaginal incision, continuing along the edge of the bone cephalad toward
the level of
the clitoris denoting where the adductor longus tendon inserts into the pubic
ramus.
The superior skin incisions are marked approximately at this location and
lateral to the
edge of the bone. The markings are made according to the same method on both
sides
(right and left) of the patient's body. Both marks lie in a straight line at
the approximate
level of the clitoris. The edge of the inferior pubic ramus is palpated until
it ends at the
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
bottom of the obturator foramen. The inferior skin incisions are then marked.
The
inferior skin incisions are located at a point approximately 3 centimeters
below and 2
centimeters lateral to the superior marks. Again, the markings are made
according to
the same method on both sides of the patient's body.
[00073] A small vertical stab incision is made over all four markings to
provide needle
entry incisions. Right superior incision 540R, left superior incision 540L,
right inferior
incision 530R, and left inferior incision 530L are all shown in Figure 25.
(Right and left
with regard to the incisions are the patient's right and left sides.)
[00074] The surgical kit described with reference to Figure 9 is opened. The
package
integrity is checked to ensure that the kit was not compromised in shipping,
and the
components of the kit are inspected for damage.
[00075] The following method describes the attachment arms on the surgeon's
right
side (the patient's left side) being surgically installed before the
attachment arms on the
surgeon's left side (the patient's right side). However, it should be readily
apparent to
one skilled in the art that the attachment arms of either side could be
installed first, and
this modification is within the scope of the invention as claimed.
[00076] Tip 78R of right superior needle 70R is then inserted through left
superior
incision 540L, through the left obturator foramen, and then through the
vaginal incision
524. Tip of right superior needle 70R is pointed perpendicular to the skin
with tip 78R in
the left superior incision 540L, shown in Figure 33. The thumb from the
surgeon's right
hand is on the outside curve of needle to control the needle movement as it
perforates
the obturator membrane and muscle. The right thumb pushes the needle through
the
obturator muscle and membrane. The needle shaft and handle is positioned at a
45
16
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
angle to the patient's vertical axis and close to the patient's body. The
needle handle is
rotated to move the needle tip and curve around the posterior surface of the
ischial
pubic ramus toward the vaginal incision and index finger. (If the needle tip
hits the
pubic bone during rotation, the needle is retracted. The needle tip is then
penetrated
beyond initial insertion depth and rotate again toward the vaginal incision.)
The needle
tip is palpated with the surgeon's finger. The finger meets the needle tip as
it moves
around the pubic ramus. (If the needle tip cannot be located, the needle tip
is retracted
to just behind the pubic ramus and advanced again.) The needle tip is guided
by the
surgeon with the surgeon's finger towards the vaginal incision until the
needle tip
extends through the vaginal incision, shown in Figures 27 and 28.
[00077] The support member is then oriented so that the tail of the graft
points away
from the surgeon. The right superior connector is connected to the tip of the
right
superior needle, the tip extending out of the vaginal incision, as shown in
Figure 36.
The superior needle connectors are closest to the leading edge of the graft
that will be
below the bladder neck.
[00078] Before attaching the connectors, the surgeon ensures that the self-
fixating
mesh and graft are not twisted. However, the connectors are removable once
snapped
onto the needle. This feature of the invention enables the physician to make
adjustments to support member 40 as needed. For example, a surgeon may wish to
remove area 28 and area 30 of support member 40 to increase the distance
between
superior arms 16 and inferior arms 18. Alternatively, a surgeon may wish to
remove
area 38 and area 44 of support member 40 to decrease the distance between
superior
arms 16 and inferior arms 18.
17
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
[00079] The connector 30 is attached to the needle 78 and the needle is
rotated back
through the skin incision pulling the connector and associated insertion
sheath and graft
into position. The process is then repeated with the left needle on the
patient's right
side.
[00080] During the procedure, it may be desirable to remove the connector 30
from the
needle 78. This process will be discussed with reference to Figures 33 and 34.
Connector 30 includes deflector tabs 102 and 104. Needle 78 is inserted into
connector
30 and locked in place between tabs 102 and 104. To retract needle 78 from
connector, removal tool 106 is used. Removal tool 106 includes a first
inclined surface
108 and a second inclined surface 110. As tool 106 is moved toward needle 78,
surface 110 contacts tab 102 and surface 108 contacts tab 104. As tool is
moved
closer toward needle 78, tab 102 moves away from tab 104 as shown in Figure
34.
This configuration allows for deflection of the connector 30 to enable the
needle 78 to
separate from connector. Tool 106 can be disposed into connector 30 through
aperture
112. Tool can be removed from aperture, or slidably fastened thereto while
remaining
within the scope of the invention. It shall be understood that removal tool
106 can
comprise a variety of configurations while remaining within the scope of the
invention.
[00081] The partially implanted apparatus is shown in Figure 37, with superior
attachment arms and support member 40 implanted and the inferior attachment
arms
extending outside the body through the vaginal incision. The insertion sheaths
and
mesh are then cut below the indicia on the end portion of the plastic sheath
and
discarded. This step allows the sheath to slide freely relative to the mesh.
The sheaths
are not removed at this time.
18
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
[00082] Next, the tip of the right inferior needle is inserted through left
inferior incision
530L, through the left obturator foramen, and then through the vaginal
incision. The tip
of the right inferior needle is pointed perpendicular to the skin with the tip
in the left
inferior incision. The exit point for the needle is confirmed to be clear of
the bladder wall
by the surgeon placing their right index finger at the distal end of the
vaginal incision
and visualizing where needle exits the distal end of vaginal incision. The
surgeon's right
thumb is on the outside curve of needle to control the needle movement as it
perforates
the obturator membrane and muscle. The right thumb pushes the needle through
the
obturator muscle and membrane.
[00083] The needle shaft and handle is positioned parallel to the patient's
vertical axis
and close to the patient's body. The needle handle is rotated, moving the
needle tip and
curve toward the distal end of the vaginal incision. The surgeon must use care
during
this step to prevent bleeding. The needle tip is then palpated as it moves
through the
distal end of the vaginal incision. The right inferior needle tip is shown
extending
outside the vaginal incision in Figure 31.
[00084] The right inferior connector is connected to the right inferior needle
tip. Again,
before attaching the connectors, the surgeon ensures that the self-fixating
mesh and
graft are not twisted. However, the connectors are removable once snapped onto
the
needle. The needle is rotated back through the skin incision pulling the
connector and
associated plastic insertion sheath and graft into position. The above process
is
repeated with the left inferior needle on the patient's right side.
[00085] The insertion sheath and mesh are then cut below the indicia on the
end
portion of the plastic sheath and discarded. This step allows the sheath to
slide freely
19
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
relative to the mesh. The sheaths are not removed at this time.
[00086] Next, it is desirable to perform a cystoscopy to check the integrity
of the uterus
and bladder. Any vaginal retraction is then removed to allow adjusting the
tension of
the mesh to reduce bladder bulge. The surgeon confirms the mesh is lying flat
and not
overlapping under the vaginal wall. The superior leading edge of the support
member
should be positioned below the bladder neck without tension. The inferior tail
portion of
the support member should is positioned at the distal end of the vaginal
incision or
towards the vaginal apex without tension.
[00087] If the mesh needs to be loosened, an instrument may be placed between
the
mesh and vaginal wall and pulled down, or away from the vaginal wall until
proper
tension is achieved. Each of the four plastic sheaths are removed and
discarded, while
ensuring the support member graft is not over tensioned. Once the plastic
sheaths are
removed, further adjustment is minimized.
[00088] If the mesh requires tightening, the tensioning suture exiting the
skin incision
on each side is grasped using a hemostat. The suture is wrapped around the
hemostat
to improve the grip and pulled up or out to tighten until proper tension is
achieved. To
loosen a biologic graft, the surgeon uses a hemostat or a clamp to pull from
each of the
hanging loosening sutures. The surgeon uses the clamps to pull down and loosen
the
attachment arm mesh as desired. The surgeon should exercise caution to avoid
pulling
on tab 18 on loosening suture 16 to loosen the attachment arm mesh.
[00089] Next, the surgeon cuts one end of each loosening suture and pulls tab
18 until
the entire loosening suture is removed. The mesh is then trimmed at the level
of the
subcutaneous tissue and all five incisions are closed. Excess vaginal tissue
may be
CA 02704205 2010-04-29
WO 2009/058131 PCT/US2007/082990
excised. Variations of this step may occur due to individual technique and
patient
anatomy. The final implanted apparatus is shown in Figure 32.
[00090] After the operation, a catheter and/or vaginal pack can be used at the
discretion of the surgeon, but should be removed prior to discharge. During
this time,
antibiotic prophylaxis should be given. The ability of the patient to empty
the bladder
should be confirmed prior to discharge.
[00091] If a biologic graft is used, the following steps are performed before
making the
vaginal incision. The biologic graft is removed from the package and prepared
per
included instructions, if needed. A precut biologic is prepared by orienting
the graft with
the tail portion pointing at the surgeon. The graft material is inserted into
the open
clamp using printed marks as guides to center the graft. (The printed side of
the plastic
sheath is facing the surgeon as the surgical apparatus is placed in the body.)
The
clamp is released to secure graft material. A desired suture is passed up
through the
clamp using a suturing mark as a guide. The suture is then passed down using
the
opposite suturing mark as the guide. The passed sutures are then secured using
the
surgeon's knot(s) of choice. Additional throws are made if needed. The clamp
sutures
are cut by passing a scissors or a scalpel down the scissors slot on each side
of the
clamp. The clamps are then removed. The clamp attachment sutures remain with
the
clamp. The surgeon assesses the attachment of the graft material mesh tape.
The
protective sheath is slid over the mesh connection to aid deployment.
[00092] The preceding steps are repeated on the opposite side of the graft.
The
sutures are passed such that the attachment knots are all on the same side of
the graft.
The biologic is placed in a saline bath to keep it hydrated during the
remainder of the
21
CA 02704205 2014-03-27
procedure. The graft tail is trimmed at the time of vaginal marking and
dissection to
reflect patients anatomy, if needed.
[00093] In addition, when using the biologic graft, the surgeon should
exercise care
when drawing the attachment arm through the body so that the sheath covers the
graft
connections and that the graft material and graft connections are not damaged.
[00094] Various modifications and variations of the present invention are
possible in
view of the above teachings. It is therefore to be understood that the
drawings and
descriptions herein are offered by way of example to facilitate comprehension
of the
invention and should not be construed to limit the scope thereof.
22