Note: Descriptions are shown in the official language in which they were submitted.
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
1
Description
Title of Invention: A BALLOON DILATATION CATHETER FOR
TREATMENT OF PARANASAL SINUS DISEASES
Technical Field
Hi The present invention relates to a steerable sinus balloon catheter
and it relates to use
of this catheter in treatment of paranasal sinus diseases with some improved
functions.
Said improvements are based on providing illumination at the distal tip of the
catheter
without the need for an external source by means of adding light source and
optic
fibers into the structure of the catheter.
Disclosure of Invention
Technical Problem
[2] In order to provide thorough understanding of the present invention,
sinus system
anatomy has to be considered. Therefore, paranasal sinus system anatomy is
shortly
described below.
1131 Paranasal sinuses are four pairs of cavities found within the cranium
or within the
cranial bones surrounding the nose and they are normally filled with air.
These are the
frontal sinuses found at the brow region above the eyes, the maxillary sinuses
found
within each of the cheekbones, the ethmoid sinuses found just behind the nose
bridge
and between the eyes, and the sphenoid sinuses found behind the eyes and the
ethmoid
sinuses.
[4] Paranasal sinuses comprise ducts called ostium for drainage of mucus,
air, and other
substances and their movement within the sinus system. In case of occurrence
of in-
flammation in the tissues forming this duct and the ostiums, it would cause
swelling of
these tissues and prevention of normal liquid flow. Said inflammation may
occur due
to allergy, toxic substances, nose polyps, and other factors. Pathological
increase that
occurs in the inflammatory tissue in time would cause permanent disruption of
liquid
flow within the sinus system.
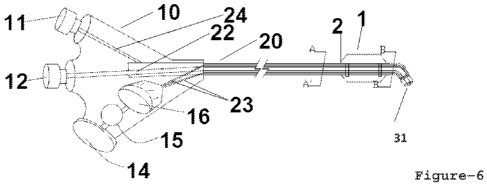
1151 Sinusitis; is the situation wherein one or more of the four paired
sinus couples are
chronically or episodically blocked due to inflammation and swelling. The most
sig-
nificant symptom of chronic sinusitis is nasal blockage that becomes severe at
night.
The basic problem behind chronic sinusitis is arrival of inadequate air to
sinuses as a
result of blockage of the sinus ducts.
[6] Nowadays, sinusitis is a frequently encountered disease that affects
large pop-
ulations. Recently, especially as a result of the improvements made in medical
technology, the technologies and devices, which both increase the chance of
success in
chronic sinusitis surgical treatment with less trauma and greatly reduces the
risk of
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
2
complication, have been presented to use.
1171 Considering above described sinus anatomy, the devices and
visualization techniques
used during surgical intervention in dark and narrow sinus structures are of
great im-
portance in terms of the success of treatment. In the known status of the art,
sinus op-
erations are generally endoscopically made. Thanks to the use of endoscope in
sinus
surgery and the improvements made, these surgeries can be made intranasally.
In this
way, external incision made in the classical sinus surgery is no more
required.
1181 This method used in the prior art is called Functional Endoscopic
Sinus Surgery and
it is based on cutting of the hypertrophic sinus tissue and bones of the
patient by en-
doscopic surgery and thus broadening of the narrowed or blocked ostiums and
providing normal drainage. Nose endoscopes are optic tools providing the
facility to
reach and illuminate the dark regions in the nasal cavity without making an
externally
visible incision.
1191 Although endoscopic sinus surgery is among the methods that are
frequently
preferred, it is observed to cause some complications. Pain and haemorrhage of
the
patient following surgery can be given as examples to the disadvantages of
this
surgical treatment method. Moreover, it is also known that many patients
continue to
have the symptoms although they have gone through a series of endoscopic
surgical
operations.
[10] Moreover, important organs and anatomic structures found around the
sinuses may
be damaged as a result of the non-rigid and non-flexible structures of the
medical in-
struments used in this surgery. And this is the main reason of pain following
surgery.
In addition to these, it also has the disadvantage of having long recovery
period.
[11] Since a great deal of the problems encountered is caused by inadequate
consideration
of the anatomy during surgery due to various reasons, the need for surgical
navigation
has occurred and improvements are made in this field. As a result, computer-
aided
surgery used in various fields is improved to be used in endoscopic sinus
surgery.
[12] This method developed for computer-aided sinus surgery is based on
real time
monitoring of the functional parts of the instruments used during surgery with
the help
of a special device and software within the complex sinus anatomy with a
margin of
error that is less than 1 mm.
[13] In spite of the improvements made in the field of visualization, with
the purpose of
eliminating the drawbacks mentioned above as the non-rigid and non-flexible
structures of the medical instruments used giving harm to important organs and
anatomic structures around the sinuses and correspondingly occurrence of post-
operation pain in the patients and having long recovery period etc, some
improvements
are made in the tools and methods. In addition to these, balloon dilatation
method can
be given, which is frequently preferred, and minimizes the damage given to the
tissue
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
3
and bones.
[14] Treatment of diseases by means of inflating balloon etc. flexible
structures within the
nose is known from the patent Nos US 6027478 and US 5546964. However, these
patents relate to use of the said inflatable flexible structures in treatment
of nasal
bleeding etc. diseases.
[15] The main principle of using balloon dilatation in sinuses is reaching
the sinus duct
with the help of sufficiently thin catheters without damaging tissues and
broadening of
the blocked area via balloon. In more detail, in this method, a flexible
balloon catheter
is inflated at the blocked region and then removed. In this way, blocked sinus
ducts are
broadened and normal flow is obtained. Balloon dilatation is known to be a
method
used alone or together with other endoscopic surgery techniques.
[16] In the prior art, during balloon dilatation method, visualization
(imaging) is achieved
by means of fluoroscopy or endoscopy and illumination is made by means of
luminous
guide wires. Balloon dilatation method is used in maxillary sinus, frontal
sinus, and
sphenoid sinus diseases, and can not be used alone in ethmoid sinuses.
[17] Patent publication no US 2011/00224652 can be given as an example to
the
documents using sinus treatment tools operating with the use of inflatable
balloons.
Said patent discloses; a balloon dilatation catheter comprising a rigid
internal guide
wire and a movable shaft in connection with a balloon adapted such that it
would skid
over this internal guide wire.
[18] The American patent no US 2008/00208243 Al discloses a balloon
catheter having a
previously adjusted angle in order to be able to be pushed into the sinuses
and
comprising a hard hypotube. In order to be able to position the balloon
catheter in the
desired ostium during surgical operation, the balloon catheter has to be
pushed forward
within the complex sinus anatomy. The catheter, which is the subject of the
said patent
application, does not enable pushing forward easily and without giving damage
to
other tissues within the sinus anatomy due to its rigid structure and
previously de-
termined fixed angle. Moreover, the problem of not fitting of a fixed-angle
catheter
formed of hard hypotube into different sinus anatomies of different people is
another
disadvantage for doctors. And production of various catheter sets having
different
fixed angles for patients having different anatomic structures is not a
practical solution,
which is quite expensive.
[19] An application made for bringing solution to the above said problem is
the ap-
plication no US 2006/0004323 Al. The invention of this application is
developed for
providing easy navigation within the complex sinus anatomy. The purpose of the
invention is to provide surgical instruments and methods about the use of
these in-
struments, which have form and flexibility that would be adapted to sinus
structures
varying according to different patients.
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
4
[20] The requirement for the surgeon to hold the endoscope with one hand
and manipulate
the surgical instruments with the other hand can be given as an example to the
problems about visualization encountered during endoscopic surgery and balloon
di-
latation method. As a result of the need for integrating surgical instruments
with the
endoscope, sinus guide catheters, which can be used transnasally, and are
connected to
an endoscope are developed. The patent application with publication no US
2006/0063973 Al can be given as an example to similar patents.
[21] Briefly, if the prior art sinus balloon dilatation instruments and
methods, various
examples of which are given above, are to be assessed in general terms, it can
be said
that the main problem is the lack of instruments, which has a structure to be
used easily
within the sinus anatomy, and at the same time helps providing an effective
visu-
alization. Starting from the prior art products and methods, in the balloon
dilatation
method, two general systems are presently used for observing the position of
the
balloon within the sinus anatomy.
[22] One of these is visualization by fluoroscopy technique, as described
above. In this
method, balloon catheter marker bands are used. As known, fluoroscopy is
formation
of the view of the patient on a fluorescent screen by means of an X-ray
source.
Although the level of X-rays used in this treatment method is low, the
patients and the
doctors are exposed to high level of radiation as a result of the long
exposure time. In
addition to this, a radiology laboratory is required, which brings limitation
to the envi-
ronments where the operation can be made.
[23] In order to eliminate the problem of using fluoroscopy device for
providing ap-
propriate location of the balloon catheter in the sinus ducts, guide wires
providing light
at the tip part are developed, and thus operations can be made on the frontal
and
maxillary sinuses without using fluoroscopy. In this method, first of all, the
guide wire
enters into the sinuses with the help of shape-adjusted sinus guide. Following
entrance
of the wire into the sinus cavity, the light emitted from the tip of the guide
wire can be
observed outside the area of operation, on the face of the patient. In this
way, entrance
of the guide into the sinus cavity is observed. Afterwards, the balloon
catheter is sent
forward from the sinus entrance on this guide wire. Since the guide wire
cannot
support the balloon catheter, a sinus guide has to support the catheter for
entrance into
the sinus structures with the correct angle.
[24] Since the illumination provided by the luminous guide wire would only
show the
position of the guide wire entering into the sinus, there would be still need
for visu-
alization of the balloon position. However, only the proximal tip of the
balloon can be
visualized by means of endoscopic camera.
[25] The main purpose of the invention of the present application is to
eliminate the above
said problems. In the prior art instruments, illumination is provided by means
of
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
separate devices or guide wires. The purpose is to provide a sinus balloon
catheter,
which is more advantageous than the prior art instruments, and which provides
an illu-
mination system at the tip part. In this way, it enables more effective
observation of the
sinus balloon catheter position in the sinus ducts.
Brief Description of The Invention
[26] The invention of the present application is a sinus balloon catheter
providing illu-
mination at its distal tip. It provides visualization by using a separate
endoscopic
camera as in the prior art. Here, the important part is, it not only enables
observation of
the proximal tip of the balloon (1), but also provides the advantage of
observing the
position of the distal tip, thanks to the system providing illumination at the
distal tip of
the catheter. In other words, the light spread from the catheter tip part can
be observed
at the outer part of the operation area, which is, on the face of the patient.
[27] In addition to this, since the said optic fibers (23) support the
required pushing ca-
pability, the need for using a separate guide wire is eliminated. In this way,
a flush
lumen (22) found in the catheter structure can be used for sinus irrigation
when
required.
[28] Another advantage is having the illumination system (14, 15, 16) at
the hub (10) of
the catheter instead of having in a separate device. In this way, illumination
can be
made without the need for using a separate light source or a connection. This
would
naturally increase the ergonomics of the surgical instrument for the doctor.
[29] The catheter of the invention is basically formed of a hub (10) and a
shaft (20).
Catheter comprises a balloon inflation-deflation port (11) in the hub (10)
part, a battery
(14) performing the task of power source (14), a LED (Light Emitting Diode)
(16)
performing the task of light source (16), and on-off button (15). Moreover, it
comprises
a chamber for battery, accumulator etc. power source (14). It comprises one or
more
optic fibers (23) providing illumination at the catheter tip part in its body.
[30] In one embodiment of the invention, said catheter tip part is made of
soft and flexible
material. In another embodiment of the invention, the tip of the catheter is
made of
hard and transparent material performing the task of a lens. Said catheter can
have
previously shape-adjusted linear form, previously shape-adjusted curved form,
or re-
shapeable and steerable form in accordance with the embodiments/configurations
to be
preferred. Moreover, in any embodiment, the present invention catheter can
comprise
flush lumen (22).
Solution to Problem
Detailed Description of The Invention
[31] The sinus illumination system (14, 15, 16, 23) of the invention
relates to having the
optic fibers (23), which provide light transmission to the target region, in
balloon
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
6
catheter structure. An embodiment of the novel sinus balloon catheter of the
present
invention developed for paranasal sinus surgery is shown in Figure-1. Novel
balloon
dilatation catheter, comprises a hub (10), which enables manipulation by means
of
being held by an operator from the proximal tip, and also forms the weld; a
balloon
inflation-deflation port (11) found on the said hub (10) body; and a light
source (16)
found on the said hub (10) body. Said light source (16) can be a high power
led (16).
Moreover, it comprises accumulator, battery (14) etc., and a chamber for these
and an
on-off button (15).
[32] The invention comprises one or more optic fibers (23) laying along its
inner body
(25) and providing transmission of light to the distal tip of the sinus
balloon dilatation
catheter. As described above, different from the prior art sinus balloon
dilatation
catheters, said catheter comprises the light source (16) required for
illuminating of the
sinus cavities in its structure, and thus the operator using the said catheter
can see the
position of the balloon (1) without the need for using external sources and
devices, X-
ray etc. methods harmful for the health of both the patient and the operator.
Usage of
the catheter without the need of being connected to another light source (16)
also
provides advantage in terms of ergonomic purposes.
[33] The sinus balloon dilatation catheter of the invention has elongated
form and
comprises a tubular catheter shaft (20) extending in distal direction from the
said
catheter hub (10) part. Said tubular catheter shaft (20) cross-section view is
shown in
Figure-1A and at the outermost, it comprises the outer jacket (26), and
towards the
inner part, balloon inflation-deflation lumen (24), inner body (25), and one
or more
fiber optics (23) are found, respectively.
[34] In other embodiments, there is not an extra outer jacket (26) and
elements structured
in the inner body (25). In other words, said catheter shaft (20) comprises a
lumen (24)
which has optic fibers (23) laying along inside of it or a lumen (24) and
optic fiber (23)
which are laying along inside the inner body(25).
[35] Catheter shaft (20) outer jacket (26) and inner body (25) material can
be selected
from thermoplastic elastomers, polymer, or polyester groups comprising
polyamide,
polyether block amides, thermoplastic urethane, polyurethane, and pet etc.
materials.
These materials can be used alone or in combination.
[36] In the embodiments comprising outer jacket (26), the outer jacket (26)
is formed in a
way that it would cylindrically surround the inner body (25) and sized such
that space/
gap would be left between them. Outer jacket (26) outer diameter can be about
1,5 mm
and inner diameter can be about 1,2 mm.
[37] This space forms the lumen (24) which provides inflation-deflation of
the balloon (1)
by means of passing liquid or gases through it. And the balloon (1) is found
at the
distal tip of the catheter shaft (20) and its position and the balloon-shaft
weld (2) are
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
7
seen in the figures. Also, marker bands (3) are found on the balloon (1).
[38] In the said embodiments which are not comprising outer jacket (26),
inflation-
deflation is made via the tubular-form lumen (24) formed along the inner body
(25)
instead of the coaxial space found between the lumen (24), inner body (25),
and outer
jacket (26).
[39] In more detail, in one of the two different embodiments, not
comprising outer jacket
(26), an inflation-deflation lumen (24) is found as extending within the inner
body (25)
and the optic fiber (23) or fibers (23) are also extended within the lumen
(24) along the
shaft (20). In the region of the balloon (1), one or more inflation-deflation
holes (50)
are configured on the inner body (25). Said inflation-deflation holes (50) are
the spaces
that provide the passage of the substances, which are sent from the lumen (24)
with the
purpose of inflating or deflating the balloon (1), through the lumen (24)
towards the
balloon (1).
[40] In the other embodiment, a tubular inflation-deflation lumen (24)
extending within
the inner body (25) and optic fiber (23) or fibers (23) extending along the
shaft (20)
beside this tubular lumen (24) are found. When the tubular inflation-deflation
lumen
(24) reaches the region where the balloon (1) is found, it reaches the inner
region of the
balloon (1) by being bent outwards. Said region is an inflation-deflation hole
(50)
opened from the inner body (25) towards the balloon (1).
[41] The sinus balloon dilatation catheter of the present invention can
comprise a soft
flexible tip (30) or a tip in the form of a hard transparent lens. This soft
and flexible
material used at the catheter tip part is selected from transparent polymer,
polyurethane, and soft thermoplastic elastomers. And the hard and transparent
material
used at the catheter tip part can be selected from the group formed of high
index
plastic, polycarbonate, and conventional plastic materials.
[42] Moreover, the sinus balloon dilatation catheter of the present
invention can comprise
a linear (30) or a previously shape-adjusted curved (31) or a steerable (33)
and op-
tionally a re-shapeable (33) tip in different embodiments. The angle of
curvature of the
previously shape-adjusted curved tip is formed such that, it would enter the
sinus ducts
in the most suitable manner and it is preferably 1100 or 40 or any angle
between these
two values. Also, in different embodiments, the sinus balloon dilatation
catheter can
comprise one or more lumen, flush lumen (22). These embodiments will be
described
in detail in the following sections.
[43] In the embodiment described above and shown in Figure-1, the tip part
(30) of the
catheter has linear form and is made of soft and flexible material.
[44] Catheter tip part can have curved, or in other words, circular form
(31) such that it
would adapt the structure of sinus cavities. Alternatively, it can have an
optionally re-
shapeable (33) distal tip, which can be added later on. The angle of curvature
is the
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
8
most suitable angle for entering into sinus ducts such that it is preferably
1100 or 40
or any angle between these two values.
[45] In Figure-2 and Figure-3, other embodiments of the sinus balloon
dilatation catheter,
which is the subject of the invention, are shown, and as also described above;
the tip
part of the catheter has previously shape-adjusted curved form (31) and is
made of soft
and flexible material. Figure-2 shows a catheter comprising an optic fiber
(23), while
Figure-3 shows a catheter comprising more than one optic fiber (23). While the
optic
fibers (23) can be made of fiber glass material, it can also be formed of
polymers with
appropriate optic light refraction index.
[46] Figure-2A, is the cross-section view of the catheter shaft (20) having
previously
shape-adjusted (31) curved tip form shown in Figure-2 and it is the same with
Figure-
1A when looked starting from the outside towards the inner parts. In Figure-
3A, the
cross-section view of the catheter shaft (20) having previously shape-adjusted
(31)
circular tip form shown in Figure-3 is shown and starting from the outside, it
is formed
of the outer jacket (26), balloon inflation-deflation lumen (24), inner body
(25), and
more than one optic fibers (23) in this inner body (25).
[47] In Figure-4 and Figure-5, again different embodiments of the invention
are shown
and the B cross-sections of the catheter shaft (20) distal tip are given.
Since this part is
found after the balloon (1), the balloon inflation-deflation lumen (24) does
not
continue here and it is clearly seen in the cross-section. Figure-4A cross-
section is the
same with the previously described ones and figure-4B is formed of the inner
body
(25) and the optic fiber (23) starting from the outside. In Figure-5, catheter
comprising
more than one optic fiber (23) is shown. In the cross-section views of this
catheter
shaft (20), the number of optic fibers (23) within the inner body (25) is more
than one.
[48] As described above, in different embodiments of the invention, the
sinus balloon di-
latation catheter can comprise a flush lumen (22) and a port (12) in
connection with
this. An embodiment of this invention comprising flush lumen (22) is shown in
figure-
6 and figure-7, and figure-7 is the view of the catheter comprising more than
one optic
fiber (23).
[49] As it is seen in these figures, the balloon dilatation catheter
comprises one flush port
(12) formed on the hub (10) of the proximal tip and one flush lumen (22)
extending
towards distal direction from this flush port (12) in the inner body (25)
found in the
catheter shaft (20). This flush port (12) can be configured by means of a
conventional
interface such as Luer connector.
[50] The cross-sections of the catheter shaft (20) distal tip shown in
Figure-6, before and
after the balloon (1) are given as the cross-section A and cross-section B in
Figure-6A
and Figure-6B, respectively. In Figure-6A, outer jacket (26), balloon
inflation-
deflation lumen (24), inner body (25), and flush lumen (22) found in the inner
body
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
9
(25) are present starting from outside towards the inner parts. In Figure-7A,
it is seen
that more than one optic fiber (23) are found within the inner body (25).
11511 The cross-sections of the distal tip of the catheter embodiments
shown in Figure-7,
before and after the balloon (1) are given as the cross-section A and cross-
section B in
Figure-7A and Figure-7B, respectively. The outer jacket (26) and the balloon
(1)
inflation-deflation lumen (24) shown in the cross-section A of the catheter is
not
included in the cross-section B, which is the distal tip cross-section found
after the
balloon (1).
11521 In another embodiment of the present invention sinus balloon
catheter, an alternative
steerable or re-shapeable (33) distal tip can be found as described above. In
the em-
bodiments comprising a steerable distal tip (33), shape adjustment wire (21)
is found in
the inner body (25) within the catheter shaft (20) providing adjustment of the
curvature
required for the said steerability and form adaptation and a shape adjustment
wheel
(13) is found for controlling it.
11531 Said shape adjustment wheel (13) is found at the catheter hub (10)
part and the shape
adjustment wire (21) connected to it extends towards the distal direction and
continues
up to the catheter tip part. In this way, adjustments about the balloon
dilatation catheter
orientation and position can be made.
11541 In Figure-8 and Figure-9, different views of the said embodiment of
the invention is
given and in Figure-8, a catheter not comprising flush lumen (22) and port
(12) is
shown, whereas the catheter shown in Figure-9 comprises a flush lumen (22) and
port
(12).
11551 In the most comprehensive embodiment of the invention shown in Figure-
9, it
comprises a balloon inflation-deflation port (11), a flush port (12), a shape
adjustment
wheel (13), and a light source (14, 15, 16) at the catheter hub (10) part; the
catheter
shaft (20) part extending towards distal direction in elongated form comprises
outer
jacket (26) at the outermost part and towards the inner parts it comprises
balloon
inflation-deflation lumen (24), inner body (25), shape adjustment wire (21)
and one or
more optic fibers (23) and flush lumen (22) in the inner body (25). The cross-
section of
the distal tip of this catheter shaft (20) described is given in Figure-9A.
And balloon
(1) is present at the distal tip of the said catheter and marker bands (3) are
found on the
balloon (1).
11561 In the above said embodiment of the invention, catheter tip can have
soft, flexible
form or hard, transparent (lens) form.
11571 The first one of the above said embodiments that is based on not
having outer jacket
(26) in the catheter shaft (20) structure and having inner body (25) as the
outermost
layer, and having the components in extended form within the said inner body
(25) is
given in Figure 11. As also can be seen there, the coaxial space found within
the inner
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
body (25) forms the inflation-deflation lumen (24). Passage of the gases or
liquids to
the balloon (1) is ensured by means of the inflation-deflation holes (50)
opened from
the lumen (24) towards the balloon (1). As it would also be understood from
AA'
section of the catheter shaft (20) in Figure 11A, the layers from outside-in
are inner
body (25), inflation-deflation lumen (24), and optic fiber (23). The number of
optic
fibers (23) extending within the lumen (24) can be more than one in different
em-
bodiments. Section BB' of the tip part (31) is given in Figure 11B.
[58] The other embodiment without outer jacket (26) is shown in figure 12.
Here, a
tubular inflation-deflation lumen (24) is found within the shaft (20) formed
by the
inner body (25). This lumen (24) extends up to the region where balloon (1) is
found
and makes an outward curve, which is towards the balloon (1) and ends at the
space of
the balloon (1). In this way, the inflation-deflation hole (50) through which
the liquids
or gases would be transferred to the balloon (1) is formed. As it would also
be seen
from section AA' of the catheter shaft (20) of this embodiment shown in Figure
12A,
the inner body (25) is found at the outermost part and an inflation-deflation
lumen (24)
is found within this inner body (25) and the optic fiber (23) extend just
nearby. Optic
fiber (23) extends towards the end. Section BB' of the shaft (20) can be seen
in Figure
12B. Since the lumen (24) ends at the balloon (1), only the inner body (25)
and the
optic fiber (23) extending within the inner body (25) are seen in section BB'.
[59] In all of the above said embodiments of the present invention
catheter, the power
source (14), on-off button (15), and light source (16) are found in the hub
(10) body. In
addition to these parts described, they can be optionally included in the
mechanism as
a separate apparatus (40) comprising the power source (14), on-off button (15)
and
light source (16) components. In order to include the said apparatus (40) into
the
catheter structure, a separate apparatus integration port (41) is found on the
hub (10).
In this way, an apparatus (40) comprising high power light source (16), power
source
(14), and on-off button (15) can be optionally integrated into the hub (10)
structure and
provide light transmission to the optic fiber (23). This apparatus integration
port (41)
found on the hub (10) can be applied to all of the above said embodiments of
the
invention. Said apparatus (4) and the integration port (41) are given in
detail in figure-
10. Moreover, the cross-section views of the said catheter are given in
Figures-10A
and 10B.
[60] In order to summarize the advantages of the novel catheter embodiment,
which is
developed for solving the problems related to the use of medical devices found
in the
prior art, and described above according to the figures, a comparison is made
below
with the prior art.
[61] In the prior art, while balloon dilatation surgery is performed, the
doctor places a
sinus guide catheter through the nostril via endoscopic view in order to reach
the sinus
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
11
ostium. Endoscope provides the doctor with the facility to see the sinus
cavities
through the nasal passage in order to be sure that the catheter is inserted in
the correct
and suitable position. Afterwards, a sinus guide wire or another sinus
illumination
system is inserted into the target sinus by means of sinus guide catheter.
Following
confirmation of the desired location via light (or fluoroscopy), the balloon
catheter is
inserted into the sinus cavity through the sinus guide wire or sinus
illumination system
and positioned to be inflated in the blocked ostium and the position of the
catheter is
confirmed by endoscopic view. Then, it is inflated to broaden and open the
said
blockage. When the said operation is complete, the balloon is deflated and
removed.
Afterwards, an irrigation catheter can be used to clean the inflammation and
mucus
found in the sinus by means of being pushed forward on the sinus guide wire or
the il-
lumination system. Integrated irrigation system is present in some of the
balloon
catheter structures and these catheters make the procedure easier.
[62] While balloon dilatation surgery is made with the novel device, the
doctor inserts a
sinus guide catheter through the nostril for the balloon catheter embodiments
that are
not steerable. Use of endoscope camera can be preferred in order to make sure
that the
doctor inserts the catheter to the correct and appropriate position.
Afterwards, the sinus
catheter of the present invention emitting light from the distal tip is pushed
towards the
sinus duct with the help of guide catheter or alone if it is a steerable
catheter. After the
light found at the tip of the catheter entering the sinus duct illuminates the
sinus cavity
and is seen from the outside and confirmed, the balloon (1) is inflated to
broaden and
open the blockage. The balloon (1) is deflated when this operation is
complete. If the
catheter embodiment comprises the flush lumen (22), then flush and irrigation
can be
made.
[63] As a result; with the novel sinus balloon dilatation catheter, the
need for a separate
guide wire is eliminated and the need for endoscopic visualization is reduced
by
providing better confirmation of the balloon position. By means of the
fibreglass inner
part (23) found within the catheter body, the need for a guide wire that would
help
supporting of the catheter and pushing of the catheter into the ostia would be
eliminated.
[64] With the illumination system (14, 15, 16) found in the catheter hub
(10) part, the
need for using a separate source is eliminated.
[65] Illumination is provided at the tip part of the catheter in order to
enable safer con-
firmation of the balloon (1) position.
[66] Briefly; the invention is a balloon dilatation catheter developed for
solving the said
problems and providing the said advantages in treatment of paranasal sinus
diseases,
and it comprises:
11671 a flexible and elongated-form tubular shaft (20), which has a
proximal and a distal
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
12
tip, and through which a primary lumen (24) and an inner body (25) passes; a
hub (10)
fixed at the proximal tip of the said tubular shaft (20); a primary port (11)
that is
connected to the primary lumen (24) passing through the said tubular shaft
(20) in the
said hub (10) body; an inflatable member (1) found at the distal tip of the
flexible
elongated shaft (20) and having internal part that is connected to the said
primary
lumen (24); an illumination system (14, 15, 16) permanently adapted to the hub
(10)
body and providing illumination at the distal part of the said inflatable
member (1) and
the distal tip of the tubular shaft (20) for safer correction of the said
inflatable member
(1) position, and comprising at least one power source (14), on-off button
(15) and at
least one light source (16); and one or more fiber optics (23), which extend
longi-
tudinally towards distal direction within the inner body (25) found in the
tubular shaft
(20) from the said light source (16) up to the distal tip of the tubular shaft
(20), and
which thus transmits light towards the distal part of the inflatable member
(1) and the
distal tip of the catheter.
[68] Briefly, in another embodiment:
[69] The invention comprises a shape adjustment wire (21), which provides
orientability
to catheter and gives optional shape adjustment capability to its tip part,
and extends
longitudinally from the proximal hub (10) body up to the distal tip within the
inner
body (25) found in the tubular shaft (20); and a shape adjustment wheel (13)
found on
the hub (10) body and connected to the shape adjustment wire (21) and
providing
control of the shape adjustment wire (21).
[70] Briefly, in another embodiment:
[71] It comprises a secondary lumen (22) extending longitudinally up to the
distal tip
within the inner body (25) found in the tubular shaft (20); and a secondary
port (12)
connected to the said secondary lumen (22) in the hub (10) body.
[72] Briefly, in different embodiments:
[73] One or more marker bands (3) are found on the inflatable member (1)
found in its
structure. The primary lumen (24) connected to the inflatable member (1) is an
inflation-deflation lumen (24) used for inflating and deflating the inflatable
member
(1) when required by means of passing liquids or gases through it; and the
primary port
(11) that is found on the hub (10) body and connected to the said primary
lumen (24) is
an inflation-deflation port (11). The inflatable member (1) found at the
distal tip of the
tubular shaft (20) is balloon (1). The secondary lumen (22) that extends
longitudinally
up to the distal tip within the inner body (25) found in the tubular shaft
(20) is a flush
lumen (22) that is used for irrigation when required; and the secondary port
(12) that is
connected with the said secondary lumen (22) in the hub (10) body is a flush
port (12).
In different embodiments, the invention has a soft and flexible tip (30) or a
hard and
transparent tip (30). It may have a linear-shaped or a previously shape-
adjusted curved
CA 02878001 2014-12-29
WO 2013/179217
PCT/1B2013/054396
13
shaped or a re-shapeable and steerable tip (33). Any part of the tubular shaft
(20) and
the catheter tip has a structure that can be bendable to adapt the sinus
cavities. Catheter
can have conical tip.
[74] As a result; said paranasal sinus operations can be made in much safer
manner than
the past and in more ergonomic and easier way for the doctors thanks to the
above said
advantages. Operation steps would be reduced by means of elimination of the
need for
separate illumination systems and use of guide wire, and thus the operation
time would
be reduced.
Brief Description of Drawings
[75] Figure-1: is the view of a linear and soft tip embodiment of the sinus
balloon di-
latation catheter.
[76] Figure-1A: is the cross-section view of the catheter shaft of a linear
and soft tip em-
bodiment of the sinus balloon dilatation catheter.
[77] Figure-2: is the view of an embodiment of the sinus balloon dilatation
catheter,
which is previously shape-adjusted as curved and has soft tip.
[78] Figure-2A: is the cross-section view of the catheter shaft of an
embodiment of the
sinus balloon dilatation catheter, which is previously shape-adjusted as
curved and has
soft tip.
[79] Figure-3: is the view of an embodiment of the s inus balloon
dilatation catheter,
which has previously curved shape-adjusted and soft tip and comprises more
than one
optic fiber.
[80] Figure-3A: is the cross-section view of the catheter shaft of an
embodiment of the s
inus balloon dilatation catheter, which has previously curved shape-adjusted
and soft
tip and comprises more than one optic fiber.
[81] Figure-4: is the view of a previously curved shape-adjusted tip
embodiment of the
sinus balloon dilatation catheter.
[82] Figure-4A: is the cross section view of a previously curved shape-
adjusted tip em-
bodiment of the sinus balloon dilatation catheter.
[83] Figure-4B: is the cross section view of the distal tip a previously
curved shape-
adjusted tip embodiment of the sinus balloon dilatation catheter.
[84] Figure-5: is the view of an embodiment of the sinus balloon dilatation
catheter,
which has previously curved shape-adjusted tip and comprises more than one
fiber
optics.
[85] Figure-5A: is the cross-section view of an embodiment of the sinus
balloon di-
latation catheter, which has previously curved shape-adjusted tip and
comprises more
than one fiber optics.
11861 Figure-
5B: is the cross-section view the distal tip of an embodiment of the sinus
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
14
balloon dilatation catheter, which has previously curved shape-adjusted tip
and
comprises more than one fiber optics.
[87] Figure-6: is the view of an embodiment of the previously curved shape-
adjusted tip
sinus balloon dilatation catheter comprising flush lumen.
[88] Figure-6A: is the cross-section view of an embodiment of the
previously curved
shape-adjusted tip sinus balloon dilatation catheter comprising flush lumen.
[89] Figure-6B: is the cross-section view of the distal tip of an
embodiment of the
previously curved shape-adjusted tip sinus balloon dilatation catheter
comprising flush
lumen.
[90] Figure-7: is the view of an embodiment of the previously curved shape-
adjusted tip
sinus balloon dilatation catheter comprising flush lumen and more than one
optic fiber.
[91] Figure-7A: is the cross-section view of an embodiment of the
previously curved
shape-adjusted tip sinus balloon dilatation catheter comprising flush lumen
and more
than one optic fiber.
[92] Figure-7B: is the cross-section view of the distal tip of an
embodiment of the
previously curved shape-adjusted tip sinus balloon dilatation catheter
comprising flush
lumen and more than one optic fiber.
[93] Figure-8: is the view of the steerable and re-shapeable tip embodiment
of the s inus
balloon dilatation catheter.
[94] Figure-8A: is the cross-section view of the steerable and re-shapeable
tip em-
bodiment of the s inus balloon dilatation catheter.
[95] Figure-9: is the view of the steerable and re-shapeable tip embodiment
of the s inus
balloon dilatation catheter comprising flush lumen.
[96] Figure-9A: is the cross-section view of the steerable and re-shapeable
tip em-
bodiment of the s inus balloon dilatation catheter comprising flush lumen.
[97] Figure-10: is the view of the external apparatus integrated at the hub
part of the sinus
balloon dilatation catheter and the embodiment comprising port for this
apparatus.
[98] Figure-10A: is the cross-section view of the sinus balloon dilatation
catheter em-
bodiment comprising integration port for the apparatus.
[99] Figure-10B: is the cross-section view of the distal part of the sinus
balloon dilatation
catheter embodiment comprising integration port for the apparatus.
[100] Figure-11: is a view of an embodiment of the sinus balloon dilatation
catheter not
comprising outer jacket and comprising primary lumen through which optic fiber
passes.
[101] Figure-11A: is a cross sectional view of an embodiment of the sinus
balloon di-
latation catheter not comprising outer jacket and comprising primary lumen
through
which optic fiber passes.
111021 Figure-11B: is a cross sectional view of a distal tip of an
embodiment of the sinus
CA 02878001 2014-12-29
WO 2013/179217 PCT/1B2013/054396
balloon dilatation catheter not comprising outer jacket and comprising primary
lumen
through which optic fiber passes.
[103] Figure-12: is a view of an embodiment of the sinus balloon dilatation
catheter not
comprising outer jacket and comprising optic fiber and tubular primary lumen.
[104] Figure-12A: is a cross sectional view of an embodiment of the sinus
balloon di-
latation catheter not comprising outer jacket and comprising optic fiber and
tubular
primary lumen.
[105] Figure-12B: is a cross sectional view of a distal tip of an
embodiment of the sinus
balloon dilatation catheter not comprising outer jacket and comprising optic
fiber and
tubular primary lumen.
[106] References
[107] 1. inflatable member (balloon)
[108] 2. inflatable member (balloon) weld
[109] 3. inflatable member (balloon) marker bands
[110] 10. hub (catheter weld)
[111] 11. inflatable member (balloon) inflation-deflation port (primary
port)
[112] 12. flush port (secondary port)
[113] 13. shape adjustment wheel
[114] 14. power source (battery, accumulator etc.) and chamber
[115] 15.on-off button
[116] 16. light source (LED etc.)
[117] 20. tubular shaft
[118] 21. shape adjustment wire
[119] 22. flush lumen (secondary lumen)
[120] 23. optic fiber
[121] 24.inflation-deflation lumen (primary lumen)
[122] 25. inner body
[123] 26. outer jacket
[124] 30. soft flexible tip
[125] 31. curved soft flexible tip
[126] 33. steerable tip
[127] 40. integrated illumination apparatus
[128] 41. apparatus integration port
111291 50. inflation-deflation hole