Note : Les descriptions sont présentées dans la langue officielle dans laquelle elles ont été soumises.
CA 02812577 2013-04-15
,
,
WOUND DRESSING
CROSS-REFERENCE TO RELATED APPLICATION
[0001] This application claims priority from and benefit of U. S. Provisional
Application
Serial No. 61/635,320, filed April 19, 2012, entitled "RENEWAL RAIN DEVICE FOR
WOUND DRESSING", and U.S. Non-Provisional Application Serial No. 13/861,687,
filed April
12, 2013, entitled "WOUND DRESSING".
TECHNICAL FIELD
[0002] The invention relates to wound dressings. More particularly, the
invention relates
to a wound dressing including a highly absorbent layer capable of keeping a
wound clean and
dry.
BACKGROUND OF THE INVENTION
[0003] People may have surgical wounds resulting from various medical
procedures. For
example, large incisions are made into the skin for exploratory surgery or the
removal of tissue.
People may have skin ulcers from various causes. Accidental injuries are
sometimes repaired
with stitches extending over large sections of the skin. Wounds result from
injuries on a
battlefield. In addition, wounds can result from surgically implanted,
indwelling catheters used in
connection with a variety of procedures. Many diabetic patients use indwelling
catheters for
delivering insulin. Patients undergoing long term chemotherapy also may have
an indwelling
catheter. Peritoneal dialysis patients use an indwelling peritoneal catheter
for delivering dialysis
fluid. All of these wounds require proper care to avoid infection and to
facilitate healing.
[0004] Protection of the wound is a significant daily task for these people.
Infection of
the wound must be avoided to prevent unintended complications. Traditional
coverings for post-
surgical wounds include bandages and gauze. One problem with these traditional
coverings is
the requirement that the coverings be frequently changed. Another problem is
injury to the
1
CA 02812577 2013-04-15
wound site caused by removal of the covering. Other problems include increased
risk of
infection and maceration of the skin due to continuous exposure to moisture.
The wounds need to
be covered to keep the wound clean, dry and infection free. Generally, when a
person with a
surgical wound dressing wants to swim, shower or bathe, the person tries to
protect the wound
site against moisture by using makeshift plastic covers taped over the exposed
wound. These
makeshift covers often fail to work, allowing moisture to enter the wound
site. They are not
designed to affirmatively repel or divert moisture away from the wound site.
Usually, the person
does not even know whether leakage has occurred until it is too late. These
makeshift covers are
simply inadequate to protect the wound site against moisture and the risk of
serious infection.
If the covering leaks and the dressing becomes wet the dressing must be
replaced so as not to
inhibit healing of a wound covered by the dressing and/or to inhibit
infection. Moisture can
support the growth of harmful or infectious bacteria in and around the site.
[0005] The need exists for a moisture-proof barrier for use by people who must
use
indwelling catheters or have other wounds to prevent infection due to exposure
to external
sources of moisture. The need also exists for a wound covering which will
absorb fluids from
the wound site, but will keep the wound site dry.
SUMMARY OF THE INVENTION
[0006] The present invention provides an improved barrier which seeks to
overcome the
above mentioned problems. In accordance with one aspect of the present
invention a wound
dressing is provided which includes a base layer with a perimeter area. The
base layer is resistant
to penetration by liquids The base layer includes an inner adhesive band and
an outer adhesive
band and has an open area in a central portion of the base layer. The adhesive
bands may be
made from, for example, polyethylene tape. The inner adhesive band and the
outer adhesive band
have a non-adhesive space between them and are connected to each other by
connection legs
spaced around the non-adhesive space. The inner adhesive band, outer adhesive
band and
2
CA 02812577 2013-04-15
connection legs are covered by a removable protective layer, the protective
layer has a plurality
of perforations spaced about the protective layer with a plurality of non-
perforated sections
between the perforations. When the protective layer is removed, the
perforations cause
separation at the perforations and only one non-perforated section is removed
at a time.
[0007] An inner layer includes an outer edge defining an inner layer area. The
inner
layer area includes a plurality of drain holes inward of the outer edge and
spaced near the
perimeter of the inner layer. In one embodiment, the inner layer is generally
rectangular in shape
and includes four sides and the plurality of drain holes are spaced such that
each is generally
centered on one of the four sides. The inner layer being resistant to
penetration by liquids. An
absorbent layer is adjacent the inner layer. The absorbent layer is preferably
made from
hydrophilic non-swelling foam, that is capable of absorbing and retaining
fluids", but other
suitable materials are possible. The absorbent layer may include a moister
sensor, such as a
cobalt strip to indicate that the absorbent layer has absorbed liquid.
[0008] An outer layer is adjacent the absorbent layer and is resistant to
penetration by
liquids. The one of the inner layer and outer layer includes an adhesive band.
The adhesive
band defines an area inward of the adhesive band which is at least as large as
the open area of
the base layer. The adhesive band is covered by a removable protective layer.
The protective
layer has a plurality of perforations spaced about it with a plurality of non-
perforated sections
between the perforations such that when the protective layer is removed, the
perforations cause
separation at the perforations and only one non-perforated section is removed
at a time. The
outer layer is adapted to be placed over the open area of the base layer and
to be attached to the
base layer by the adhesive band of the outer layer.
[0009] In another embodiment, a wound dressing is provides which includes an
inner
layer with an outer edge defining an inner layer area. The inner layer area
includes a plurality of
drain holes inward of the outer edge and spaced near the perimeter of the
inner layer. The inner
3
CA 02812577 2013-04-15
layer is resistant to penetration by liquids. An absorbent layer is adjacent,
but not attached to, the
inner layer.
[0010] An outer layer is adjacent, but not attached to, the absorbent layer.
The outer
layer is resistant to penetration by liquids and includes an inner adhesive
band, and an outer
adhesive band. The inner adhesive band defines an area inward of the inner
adhesive band
which is at least as large as the inner layer area. The inner adhesive band
and the outer adhesive
band define a non-adhesive space between them and are connected by connection
legs spaced
around the non-adhesive space. The inner adhesive band, outer adhesive band
and connection
legs are covered by a removable protective layer which has a plurality of
perforations spaced
about the protective layer with a plurality of non-perforated sections between
the perforations
such that when the protective layer is removed, the perforations cause
separation at the
perforations and only one non-perforated section is removed at a time.
BRIEF DESCRIPTION OF THE SEVERAL VIEWS OF THE DRAWINGS
[0011] The foregoing and other objects, features, and advantages of the
invention will be
apparent from the following drawings and more particular description of the
preferred
embodiments of the invention.
[0012] FIG. 1 is a perspective view of the present invention;
[0013] FIG. 2 is a front elevation view of the invention of FIG. 1;
[0014] FIG. 3 is an exploded perspective view of the invention of FIG. 1;
[0015] FIG. 4 is a perspective view of a second embodiment of the present
invention;
[0016] FIG. 5 is a front elevation view of the invention of FIG. 4; and
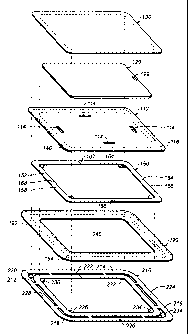
[0017] FIG. 6 is an exploded perspective view of the invention of FIG. 4.
DETAILED DESCRIPTION OF THE INVENTON
[0018] Throughout the following description, specific details are set forth in
order to
provide a more thorough understanding of the invention. However, the invention
may be
4
CA 02812577 2013-04-15
practiced without these particulars. In other instances, well known elements
have not been
shown or described in detail to avoid unnecessarily obscuring the disclosure.
Accordingly, the
specification and drawings are to be regarded as illustrative rather than
restrictive. It is to be
further noted that the drawings are not to scale.
[0019] Figures 1 through 3 illustrate a first embodiment of the invention.
Referring to
Figs 1 and 2, the wound dressing 10 includes an inner layer 12, an absorbent
layer 20, an outer
layer 30 and a backing layer 50.
[0020] Referring to Fig. 3, the inner layer 12 is constructed of a suitable
material resistant
to penetration by liquids, such as such as medical grade non-allergenic
polyethylene, although
other materials such as, for example, polyurethane, will work. Preferably, the
inner layer 12 is
between 1 and 2 mils thick, although thicknesses outside this range are
acceptable. The inner
layer 12 is shown as generally rectangular, but a variety of shapes are
possible such as, square,
round, oval or other suitable shapes. The inner layer 12 includes drainage
holes 14 spaced about
the perimeter 16 of the inner layer 12.
[0021] The absorbent layer 20 is preferably made from a material such as
hydrocolloid,
which is capable of absorbing liquids such as blood, exudate, and other
liquids, entering through
the drain holes 14. The absorbent layer 20 is sized such that it is no larger
than the inner layer
12. The shape of the absorbent layer preferably generally conforms to that of
the inner layer 12.
Preferably, the absorbent layer 20 has a thickness of between 4 mm and 12 mm.
The absorbent
layer 20 can include a moisture indicator 22, such as, for example, a cobalt
strip.
[0022] The outer layer 30 is constructed of a suitable material such as
medical grade non-
allergenic polyethylene which is resistant to penetration by liquids although
other materials such
as for example, polyurethane, will work. Preferably, the outer layer 30 is
between 1 and 2 mils
thick, although thicknesses outside this range are acceptable. The outer layer
30 is preferably
larger than the inner layer 12. Preferably, the shape of the outer layer
generally conforms to that
of the inner layer 12. An outer adhesive band 32 is located near the perimeter
34 of the outer
layer 30. An inner adhesive band 36 is placed inward from the outer adhesive
band 32. The
width of the outer adhesive band 32 and the inner adhesive band 36 will vary
depending on the
size of the wound dressing. Preferably, the adhesive band is made from medical
grade, double-
CA 02812577 2013-04-15
coated clear polyethylene tape with a non-sensitized acrylic pressure
sensitive adhesive.
Between the outer adhesive band 32 and the inner adhesive band 36 is a non-
adhesive space 38.
Legs 40 connect the outer adhesive band 32 and inner adhesive band 36 at
various locations.
The precise locations of the legs 40 may change depending on the size and
shape of the wound
dressing 10.
[0023] A removable protective backing 50 covers the outer adhesive band 32,
the inner
adhesive band 36 and the legs 40. Preferably, the protective backing 50
includes multiple
sections 52, 54, 56 and 58 spaced about the protective backing 50 and
perforations 62, 64, 66 and
68 between the sections 52, 54, 56 and 58. It will be understood by those of
ordinary skill in the
art that fewer or more sections will work equally as well. The removable
protective backing 50
preferably includes tabs 70, 72, 74 and 76. The removable backing 50 also
includes legs 78
corresponding to the legs 40 connecting the adhesive bands 32 and 36.
[0024] To place the wound dressing 10 over a wound, the protective backing 50
is pulled
by one of the tabs 70, 72, 74 or 76. For example, section 52 is pulled away
from outer adhesive
band 32 and inner adhesive band 36. The section 52 breaks from the adjacent
sections 54 and 58
at the perforations 62 and 68. The exposed portions of the outer adhesive band
32 and inner
adhesive band 36 are placed on the skin (not shown). The process is repeated
for the next
sections 54 and 56. The last remaining section 58 is pulled off and the
adhesive layer is
attached to the skin (not shown), creating a seal and covering which is
resistant to penetration by
liquids from the outside. Because the adhesive bands 32 and 36 are placed on
the skin (not
shown) in sections, prior to the attachment of the last section, the
relatively warmer air
underneath the wound dressing 10 begins to move from the area underneath the
wound dressing
to the area beyond the wound dressing 10, taking the warm moist air out from
underneath the
wound dressing 10.
[0025] Figures 4 to 6 illustrate a second embodiment of the invention.
Referring to Figs.
4 and 5, the wound dressing 110 includes an inner layer 112, an absorbent
layer 120, an outer
layer 130 and a base layer 190.
[0026] Referring to Fig. 6, the inner layer 112 is constructed of a suitable
material
resistant to penetration by liquids, such as medical grade non-allergenic
polyethylene, although
6
CA 02812577 2013-04-15
,
,
other materials such as, for example, polyurethane, will work. Preferably, the
inner layer 112 is
between 1 mil and 2 mils thick, although thicknesses outside of this range
will work. The inner
layer 112 is shown as generally rectangular, but a variety of shapes are
possible such as, square,
round etc. The inner layer 112 includes drainage holes 114 spaced about the
perimeter 116 of
the inner layer 112. Preferably, an adhesive band 140 is located near the
perimeter 116 of the
inner layer 112. It will be understood by those of ordinary skill in the art
that the adhesive band
140 could be placed on the outer layer 130 instead of the inner layer 112. The
width of the
adhesive band 140 may vary depending on the size of the wound dressing.
100271 The absorbent layer 120 is preferably made from a material capable of
absorbing
liquids such as a material such as hydrocolloid, which is capable of absorbing
liquids such as
blood, exudate, and other liquids. The absorbent layer 120 is sized such that
it is no larger than
the inner layer 112. Preferably, the absorbent layer 120 has a thickness of
between 4 mm and 12
mm, although thicknesses outside this range will work. The absorbent layer 20
can include a
moisture indicator 122, such as, for example, a cobalt strip
100281 The outer layer 130 is constructed of a suitable material such as
medical grade
non-allergenic polyethylene which is resistant to penetration by liquids
although other materials
such as, for example, polyurethane will work. Preferably, the outer layer 130
is between 1 mil
and 2 mils thick, although thicknesses outside of this range will work.
[0029] A removable protective backing 150 covers the adhesive band 140.
Preferably,
the protective backing 150 includes multiple sections 152, 154, 156 and 158
spaced about the
protective backing 150 and perforations 162, 164, 166 and 168 between the
sections 152, 154,
156 and 158. It will be understood by those of ordinary skill in the art that
fewer or more
sections will work equally as well.
[0030] A base layer 190 is provided and includes an outer adhesive band 192
and an
inner adhesive band 194. The base layer 190 has an open center area 240. A
removable
protective backing 210 covers the outer adhesive band 192, the inner adhesive
band 194.
Preferably, the protective backing 210 includes multiple sections 212, 214,
216 and 218 spaced
about the protective backing 210 and perforations 222, 224, 226 and 228
between the sections
212, 214, 216 and 218. It will be understood by those of ordinary skill in the
art that fewer or
7
CA 02812577 2014-08-21
more sections will work equally as well. The removable protective backing 150
preferably
includes tabs 230, 232, 234 and 236.
[0031] To place the wound dressing 110 over a wound, protective backing layer
section
212 is removed by pulling on tab 230. Protective backing layer section 212
will break away
from sections 214 and 218 at perforations 222 and 228. The exposed portion of
adhesive bands
192 and 194 are placed on the skin (not shown). The remaining sections of the
adhesive bands
192 and 194 are placed on the skin the same manner.
[0032] Next, the removable protective backing 150 is removed from the adhesive
band
140 on the inner layer 112. The inner layer 112 is placed so that it covers
the open center area
240 and the adhesive band 140 attaches to the base layer 190.
[0033] As will be apparent to those skilled in the art in light of the
foregoing disclosure,
many alterations and modifications are possible in the practice of this
invention without
departing from the scope thereof as defined by the appended claims.
8